- Record: found
- Abstract: found
- Article: found
Kimura’s disease with membranoproliferative glomerulonephritis: a case report with literature review
Read this article at
Abstract
Background: Kimura's disease is a rare disease and its etiology is still unclear. Here we reported a case with lymphadenopathy complicated with secondary membranoproliferative glomerulonephritis.
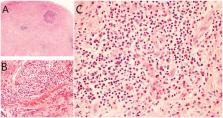
Case presentation: A 46-year-old Chinese man presented with bilateral tumor-like nodules over his neck during the past 6 months and developed edema for 15 days. His blood pressure was 145/90 mmHg, multiple 1 × 1 cm masses were found over bilateral post-auricular and submandibular areas, along with trace edema of the lower extremities. Laboratory data showed an increased peripheral eosinophil count at 3.66 × 10 9/L (50% of total leukocytes), with a 24-hour urine total protein of 8 g and a serum albumin of 19 g/L, and serum IgE of 2930 IU/ml (<100 IU/ml). The patient underwent renal biopsy, which revealed membranoproliferative glomerulonephritis with eosinophilic infiltration of the interstitium. Lymph node biopsy showed eosinophilic lymphoid follicular granuloma. Bone marrow biopsy showed no abnormalities. A diagnosis of Kimura's disease was then established. We started him on prednisone 60 mg/day (1 mg/kg), and tapered the dose to 55 mg/day 2 months later, followed by a gradual reduction of 2.5 mg every 2 weeks. Valsartan was given for blood pressure control. His neck nodules shrank after 2 weeks of treatment and complete renal remission was achieved 3 months later. No relapse occurred after follow-up for 31 months.
Conclusion: Kimura's disease can present with bilateral neck nodules and nephrotic syndrome (membranoproliferative glomerulonephritis), and prednisone can be a suitable choice of treatment.
Related collections
Most cited references15
- Record: found
- Abstract: found
- Article: not found
Increase of Th2 and Tc1 cells in patients with Kimura's disease.
- Record: found
- Abstract: found
- Article: not found
Idiopathic membranoproliferative glomerulonephritis: does it exist?
- Record: found
- Abstract: found
- Article: not found