- Record: found
- Abstract: found
- Article: found
Functional respiratory imaging: heterogeneity of acute exacerbations of COPD
Abstract
Background
Exacerbations of COPD are a major burden to patients, and yet little is understood about heterogeneity. It contributes to the current persistent one-size-fits-all treatment. To replace this treatment by more personalized, precision medicine, new insights are required. We assessed the heterogeneity of exacerbations by functional respiratory imaging (FRI) in 3-dimensional models of airways and lungs.
Methods
The trial was designed as a multicenter trial of patients with an acute exacerbation of COPD who were assessed by FRI, pulmonary function tests, and patient-reported outcomes, both in the acute stage and during resolution.
Results
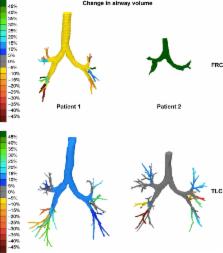
Forty seven patients were assessed. FRI analyses showed significant improvements in hyperinflation (a decrease in total volume at functional residual capacity of −0.25±0.61 L, p≤0.01), airway volume at total lung capacity (+1.70±4.65 L, p=0.02), and airway resistance. As expected, these improvements correlated partially with changes in the quality of life and in conventional lung function test parameters. Patients with the same changes in pulmonary function differ in regional disease activity measured by FRI.
Conclusion
FRI is a useful tool to get a better insight into exacerbations of COPD, and significant improvements in its indices can be demonstrated from the acute phase to resolution even in relatively small groups. It clearly visualizes the marked variability within and between individuals in ventilation and resistance during exacerbations and is a tool for the assessment of the heterogeneity of COPD exacerbations.
Most cited references21
- Record: found
- Abstract: found
- Article: not found
The connection between chronic obstructive pulmonary disease symptoms and hyperinflation and its impact on exercise and function.
- Record: found
- Abstract: found
- Article: not found
Validation of computational fluid dynamics in CT-based airway models with SPECT/CT.
- Record: found
- Abstract: found
- Article: not found