- Record: found
- Abstract: found
- Article: found
GLP-1R Agonist Liraglutide Activates Cytoprotective Pathways and Improves Outcomes After Experimental Myocardial Infarction in Mice
Read this article at
Abstract
OBJECTIVE
Glucagon-like peptide-1 receptor (GLP-1R) agonists are used to treat type 2 diabetes, and transient GLP-1 administration improved cardiac function in humans after acute myocardial infarction (MI) and percutaneous revascularization. However, the consequences of GLP-1R activation before ischemic myocardial injury remain unclear.
RESEARCH DESIGN AND METHODS
We assessed the pathophysiology and outcome of coronary artery occlusion in normal and diabetic mice pretreated with the GLP-1R agonist liraglutide.
RESULTS
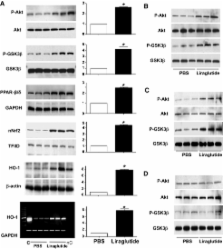
Male C57BL/6 mice were treated twice daily for 7 days with liraglutide or saline followed by induction of MI. Survival was significantly higher in liraglutide-treated mice. Liraglutide reduced cardiac rupture (12 of 60 versus 46 of 60; P = 0.0001) and infarct size (21 ± 2% versus 29 ± 3%, P = 0.02) and improved cardiac output (12.4 ± 0.6 versus 9.7 ± 0.6 ml/min; P = 0.002). Liraglutide also modulated the expression and activity of cardioprotective genes in the mouse heart, including Akt, GSK3β, PPARβ-δ, Nrf-2, and HO-1. The effects of liraglutide on survival were independent of weight loss. Moreover, liraglutide conferred cardioprotection and survival advantages over metformin, despite equivalent glycemic control, in diabetic mice with experimental MI. The cardioprotective effects of liraglutide remained detectable 4 days after cessation of therapy and may be partly direct, because liraglutide increased cyclic AMP formation and reduced the extent of caspase-3 activation in cardiomyocytes in a GLP-1R–dependent manner in vitro.
Related collections
Most cited references38
- Record: found
- Abstract: found
- Article: not found
Cardioprotective and vasodilatory actions of glucagon-like peptide 1 receptor are mediated through both glucagon-like peptide 1 receptor-dependent and -independent pathways.
- Record: found
- Abstract: found
- Article: not found
Glucagon-like peptide-1 receptor is involved in learning and neuroprotection.
- Record: found
- Abstract: found
- Article: not found