- Record: found
- Abstract: found
- Article: found
CONSORT 2010 Statement: updated guidelines for reporting parallel group randomised trials
other

23 March 2010
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
The CONSORT statement is used worldwide to improve the reporting of randomised controlled trials. Kenneth Schulz and colleagues describe the latest version, CONSORT 2010, which updates the reporting guideline based on new methodological evidence and accumulating experience
Related collections
Most cited references22

- Record: found
- Abstract: found
- Article: found
Long Term Outcomes Following Hospital Admission for Sepsis Using Relative Survival Analysis: A Prospective Cohort Study of 1,092 Patients with 5 Year Follow Up
Joshua Davis, Vincent He, Nicholas Anstey … (2014)
- Record: found
- Abstract: found
- Article: found
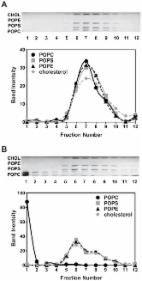
Preparation of Artificial Plasma Membrane Mimicking Vesicles with Lipid Asymmetry
Qingqing Lin, Erwin London (2014)

- Record: found
- Abstract: found
- Article: found
Outcomes in Patients with Acute and Stable Coronary Syndromes; Insights from the Prospective NOBORI-2 Study
Farzin Fath-Ordoubadi, Erik Spaepen, Magdi El-Omar … (2014)