- Record: found
- Abstract: found
- Article: found
Intake of saturated and trans unsaturated fatty acids and risk of all cause mortality, cardiovascular disease, and type 2 diabetes: systematic review and meta-analysis of observational studies

Read this article at
Abstract
Objective To systematically review associations between intake of saturated fat and trans unsaturated fat and all cause mortality, cardiovascular disease (CVD) and associated mortality, coronary heart disease (CHD) and associated mortality, ischemic stroke, and type 2 diabetes.
Design Systematic review and meta-analysis.
Data sources Medline, Embase, Cochrane Central Registry of Controlled Trials, Evidence-Based Medicine Reviews, and CINAHL from inception to 1 May 2015, supplemented by bibliographies of retrieved articles and previous reviews.
Eligibility criteria for selecting studies Observational studies reporting associations of saturated fat and/or trans unsaturated fat (total, industrially manufactured, or from ruminant animals) with all cause mortality, CHD/CVD mortality, total CHD, ischemic stroke, or type 2 diabetes.
Data extraction and synthesis Two reviewers independently extracted data and assessed study risks of bias. Multivariable relative risks were pooled. Heterogeneity was assessed and quantified. Potential publication bias was assessed and subgroup analyses were undertaken. The GRADE approach was used to evaluate quality of evidence and certainty of conclusions.
Results For saturated fat, three to 12 prospective cohort studies for each association were pooled (five to 17 comparisons with 90 501-339 090 participants). Saturated fat intake was not associated with all cause mortality (relative risk 0.99, 95% confidence interval 0.91 to 1.09), CVD mortality (0.97, 0.84 to 1.12), total CHD (1.06, 0.95 to 1.17), ischemic stroke (1.02, 0.90 to 1.15), or type 2 diabetes (0.95, 0.88 to 1.03). There was no convincing lack of association between saturated fat and CHD mortality (1.15, 0.97 to 1.36; P=0.10). For trans fats, one to six prospective cohort studies for each association were pooled (two to seven comparisons with 12 942-230 135 participants). Total trans fat intake was associated with all cause mortality (1.34, 1.16 to 1.56), CHD mortality (1.28, 1.09 to 1.50), and total CHD (1.21, 1.10 to 1.33) but not ischemic stroke (1.07, 0.88 to 1.28) or type 2 diabetes (1.10, 0.95 to 1.27). Industrial, but not ruminant, trans fats were associated with CHD mortality (1.18 (1.04 to 1.33) v 1.01 (0.71 to 1.43)) and CHD (1.42 (1.05 to 1.92) v 0.93 (0.73 to 1.18)). Ruminant trans-palmitoleic acid was inversely associated with type 2 diabetes (0.58, 0.46 to 0.74). The certainty of associations between saturated fat and all outcomes was “very low.” The certainty of associations of trans fat with CHD outcomes was “moderate” and “very low” to “low” for other associations.
Conclusions Saturated fats are not associated with all cause mortality, CVD, CHD, ischemic stroke, or type 2 diabetes, but the evidence is heterogeneous with methodological limitations. Trans fats are associated with all cause mortality, total CHD, and CHD mortality, probably because of higher levels of intake of industrial trans fats than ruminant trans fats. Dietary guidelines must carefully consider the health effects of recommendations for alternative macronutrients to replace trans fats and saturated fats.
Related collections
Most cited references127

- Record: found
- Abstract: found
- Article: found
Long Term Outcomes Following Hospital Admission for Sepsis Using Relative Survival Analysis: A Prospective Cohort Study of 1,092 Patients with 5 Year Follow Up
- Record: found
- Abstract: found
- Article: found
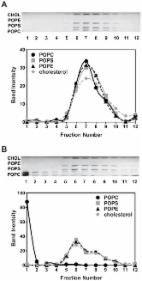
Preparation of Artificial Plasma Membrane Mimicking Vesicles with Lipid Asymmetry

- Record: found
- Abstract: found
- Article: found