- Record: found
- Abstract: found
- Article: found
T Helper 9 Cells: A New Player in Immune-Related Diseases
review-article
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
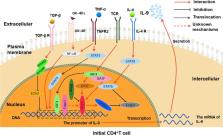
The helper T cell 9 (Thelper-9, Th9), as a functional subgroup of CD4 +T cells, was first discovered in 2008. Th9 cells expressed transcription factor PU.1 and cytokine interleukin-9 (IL-9) characteristically. Recent researches have shown that the differentiation of Th9 cells was coregulated by cytokine transforming growth factor β, IL-4, and various transcription factors. Th9 cells, as a new player, played an important role in various immune-related diseases, including tumors, inflammatory diseases, parasite infection, and other diseases. In this article, we summarize the related research progress and discuss the possible prospect.
Related collections
Most cited references55
- Record: found
- Abstract: found
- Article: not found
Transforming growth factor-beta 'reprograms' the differentiation of T helper 2 cells and promotes an interleukin 9-producing subset.
- Record: found
- Abstract: found
- Article: not found
IL-21 and TGF-beta are required for differentiation of human T(H)17 cells.
Li. Yang, David Anderson, Clare Baecher-Allan … (2008)
- Record: found
- Abstract: found
- Article: not found
Control of immunity by the TNFR-related molecule OX40 (CD134).
Michael Croft (2010)