- Record: found
- Abstract: found
- Article: not found
Relevance of SARS-CoV-2 related factors ACE2 and TMPRSS2 expressions in gastrointestinal tissue with pathogenesis of digestive symptoms, diabetes-associated mortality, and disease recurrence in COVID-19 patients
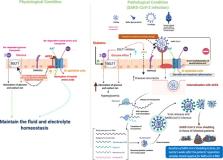
Graphical abstract
Abstract
COVID-19 is caused by a new strain of coronavirus called SARS-coronavirus-2 (SARS-CoV-2), which is a positive sense single strand RNA virus. In humans, it binds to angiotensin converting enzyme 2 (ACE2) with the help a structural protein on its surface called the S-spike. Further, cleavage of the viral spike protein (S) by the proteases like transmembrane serine protease 2 (TMPRSS2) or Cathepsin L (CTSL) is essential to effectuate host cell membrane fusion and virus infectivity. COVID-19 poses intriguing issues with imperative relevance to clinicians. The pathogenesis of GI symptoms, diabetes-associated mortality, and disease recurrence in COVID-19 are of particular relevance because they cannot be sufficiently explained from the existing knowledge of the viral diseases. Tissue specific variations of SARS-CoV-2 cell entry related receptors expression in healthy individuals can help in understanding the pathophysiological basis the aforementioned collection of symptoms.
ACE2 mediated dysregulation of sodium dependent glucose transporter (SGLT1 or SLC5A1) in the intestinal epithelium also links it to the pathogenesis of diabetes mellitus which can be a possible reason for the associated mortality in COVID-19 patients with diabetes. High expression of ACE2 in mucosal cells of the intestine and GB make these organs potential sites for the virus entry and replication. Continued replication of the virus at these ACE2 enriched sites may be a basis for the disease recurrence reported in some, thought to be cured, patients.
Based on the human tissue specific distribution of SARS-CoV-2 cell entry factors ACE2 and TMPRSS2 and other supportive evidence from the literature, we hypothesize that SARS-CoV-2 host cell entry receptor—ACE2 based mechanism in GI tissue may be involved in COVID-19 (i) in the pathogenesis of digestive symptoms, (ii) in increased diabetic complications, (iii) in disease recurrence.
Related collections
Most cited references30
- Record: found
- Abstract: found
- Article: not found
Clinical Characteristics of Coronavirus Disease 2019 in China
- Record: found
- Abstract: found
- Article: not found
SARS-CoV-2 Cell Entry Depends on ACE2 and TMPRSS2 and Is Blocked by a Clinically Proven Protease Inhibitor
- Record: found
- Abstract: found
- Article: not found

