- Record: found
- Abstract: found
- Article: not found
Recent Developments in Drug Discovery for Leishmaniasis and Human African Trypanosomiasis
review-article

Advait S. Nagle
† ,
Shilpi Khare
† ,
Arun Babu Kumar
‡ ,
Frantisek Supek
† ,
Andriy Buchynskyy
‡ ,
Casey J. N. Mathison
† ,
Naveen Kumar Chennamaneni
‡ ,
Nagendar Pendem
‡ ,
Frederick S. Buckner
∥ ,
Michael H. Gelb
‡
,
§ ,
Valentina Molteni
†
,
03 November 2014
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
1
Introduction to Leishmaniasis
Leishmaniasis is a parasitic disease that presents four main clinical
syndromes: cutaneous leishmaniasis (CL), mucocutaneous leishmaniasis
(MCL), visceral leishmaniasis/kala azar (VL), and post kala azar dermal
leishmaniasis (PKDL). Causative Leishmania are protozoan
parasites that are transmitted among mammalian hosts by phlebotomine
sandflies. In mammalian hosts, parasite cells proliferate inside the
host phagocytic cells as round amastigotes. Infection of sandflies
with Leishmania occurs during insect feeding on infected
mammalian hosts. After introduction into the insect gut together with
the blood meal, Leishmania amastigotes transform
into elongated flagellated promastigotes that propagate in the insect
gut. A new round of infection is initiated after the infected sandfly
takes a blood meal from a naïve mammalian host and introduces Leishmania parasites
into the bite wound in the host dermis
(Scheme 1). More than 20 different Leishmania species have been found to cause human
leishmaniasis
(Table 1).
Leishmaniasis is endemic in
98 countries and is closely associated
with poverty. More than a million new cases are reported per year
and 350 million people are at risk of contracting the infection. For
the most severe form of leishmaniasis, VL, ∼300 000
new cases are estimated to occur annually resulting in ∼40 000
deaths. Approximately 90% of all VL cases occur in 3 endemic foci:
1. India, Bangladesh, and Nepal; 2. East Africa; and 3. Brazil. In
spite of the high prevalence, currently available treatments for leishmaniasis
are inadequate. Pentavalent antimonials, the standard treatment for
leishmaniasis for many decades, are not efficacious in Bihar (∼60%
of VL cases worldwide) any longer due to widespread resistance to
the drug in this region. Several new VL treatments have emerged during
the past 10–15 years, but each has serious shortcomings (summarized
in Table 2). These include paromomycin (injectable,
long treatment, region-dependent efficacy), miltefosine (cost, teratogenicity,
long treatment), and liposomal amphotericin B (cost, hospitalization,
region-dependent efficacy). An additional challenge is represented
by patients with HIV/VL coinfections who are more difficult to cure
(lower initial and final cure rates), have greater susceptibility
to drug toxicity, and have higher rates of death and relapse.
Due to the limitations of the existing treatments, better drugs
are urgently needed. Ideally, new VL drugs would be efficacious across
all endemic regions, would affect cure in ≤10 days, and would
cost <$10 per course (for a complete target product profile for
new VL drugs, which was formulated by DNDi, see Table 4).
1
Here we describe the disease
history and parasite biology followed by a summary of the currently
available treatments and, finally, review reports of novel small molecules
with antileishmanial activity.
2
Background of Leishmaniasis
2.1
History and Biology of Leishmaniasis
Depending on the
disease symptoms, leishmaniasis diagnosis typically
falls into one of four major categories: visceral (VL), mucocutaneous
(MC), post kala azar dermal (PKDL), or cutaneous leishmaniasis (CL).
The earliest Old World records describing lesions with CL character
go back to the seventh century BCE.
2
Detailed
reports from Arab physicians in the 10th century describe CL in various
regions of what is today called the Middle East.
2
Old World VL, or kala azar, characterized by an enlarged
spleen, was first recognized in India in 1824. However, the symptoms
were confused with those of malaria, and attempts were then made to
treat the patients with quinine.
3
Clear
recognition of VL as a distinct disease was achieved in 1900 after
William Leishman and Charles Donovan independently identified Leishmania donovani
parasites in the spleens of kala azar
patients.
4
At about the same time Leishmania parasites were also observed in samples obtained
from CL lesions. In 1908, Nicolle isolated the parasite from a cutaneous
lesion and established the similarity between cutaneous and visceral
forms of the disease with regard to the causative agent.
5
The majority of CL cases in the Old World are
caused by two Leishmania species: L. major and L. tropica.
In the New World, CL and
MCL cause disfiguring conditions and these have been depicted on sculptures
dating back to the fifth century. References to leishmaniasis are
also found in the writings of Spanish missionaries from the 16th century.
6
In 1911, Gaspar Vianna discovered that leishmaniasis
in South America was caused by a different Leishmania species from that in the Old
World, and coined a new name, L. brazilienses, for this species.
7
The species name was later corrected to L. braziliensis.
8
In the 1960s, additional Leishmania
species causing CL in Latin America, were recognized such as L. mexicana.
9
In 1937, the causative
agent of VL in the New World was designated as a distinct species,
named L. chagasi.
10
However,
this species is indistinguishable from L. infantum, the species that causes VL in
southern Europe.
11
Leishmania parasites are protozoa
belonging to
the Kinetoplastida order and Trypanosomatidae family. Over 20 species
have been shown to be pathogenic in mammals, with affected hosts including
domesticated and sylvatic animals. The parasites are transmitted indirectly
between hosts by two different genera of hematophagous sand flies: Phlebotomus and
Lutzomyia in the Old and
New Worlds, respectively.
The life cycle of the Leishmania parasite is characterized
by two distinct morphologies (Scheme 1): the
elongated and flagellated promastigote, found in the alimentary tract
of the female sand fly vector, and the round nonmotile amastigote,
present in the bloodstream and tissues of the mammalian host. As an
infected sand fly takes a blood meal from a naïve host, it
regurgitates infective promastigotes at the bite site. The parasites
are subsequently taken up by host dendritic cells and macrophages
in the dermal layer of the skin. Here, they differentiate into amastigotes
and multiply within phagolysosomes (via binary fission) while resisting
degradation by lysosomal enzymes. Upon lysis of infected macrophage
and dendritic cells, the parasites disseminate via the lymph and circulatory
system and go on to infect other macrophages of the reticulo-endothelial
system. The parasites persist in macrophages present in the spleen,
bone marrow, liver, and lymph nodes and induce extensive inflammation
and increased hematopoiesis.
12
Infected
patients serve as parasite reservoirs and can infect naïve
sandflies when infected macrophages are ingested as part of the sandfly
blood meal. After the parasite-infected macrophage is ingested by
the sandfly, the amastigotes transform into promastigotes in the insect
midgut, multiply, and migrate to the proximal end of the gut, where
they remain until the next cycle of vector–host infection and
transmission.
12c,12d,13
Scheme 1
Life Cycle of Leishmania Parasites (source: Public
Health Image Library, provided by CDC- DPDx/Alexander J. da Silva,
Ph.D., Blaine Mathison)
2.2
Clinical Description and Diagnosis of Leishmaniasis
2.2.1
Visceral Leishmaniasis and Post Kala Azar
Dermal Leishmaniasis
VL is the most severe form of the disease
and typically results in death if left untreated.
14
The clinical features generally manifest 2–6 months
after infection, and these include prolonged fever, splenomegaly,
hepatomegaly, pancytopenia, progressive anemia, and weight loss.
12c,12d,15
Latent cases may remain undiagnosed
until the patient becomes immunocompromised, with symptoms then appearing
only several years after infection.
12c,12d,14,15b
Darkening of the skin
occurs in patients (particularly in South Asia) and defines the origin
of the disease synonym kala azar (black fever in the Hindi language).
12d,16
VL patients are at high risk for bacterial coinfections, including
pneumonia, tuberculosis, and gastrointestinal (GI) infection.
12c
Both Leishmania and HIV target
the immune system, and coinfections are found in overlapping HIV/VL-endemic
areas, specifically Ethiopia, Brazil, and India.
17
Furthermore, the risk of developing VL is approximately
100- to 2000-times greater in patients infected with HIV compared
to non-HIV individuals.
18
HIV/VL coinfected
patients have a reduced CD4+ T-cell count (below 200 cells/μL)
and generally present symptoms similar to those observed in HIV-negative
patients, including fever, splenomegaly, pancytopenia, lymphadenopathy,
lethargy, and gastrointestinal issues. Co-infections are also more
refractory to treatment and often require VL rescue therapy with an
alternative drug.
19
Post kala azar
dermal leishmaniasis, or PKDL, is a form of dermal
leishmaniasis that may appear months to years after effective treatment
of VL and exhibits distinct features based on geography (Indian and
Sudanese PKDL).
12d,15b,20
The clinical symptoms include papule skin lesions on the face, which
gradually increase in size to form nodules all over the body and which
can further transform into large plaques (Indian) or ulcers (Sudanese).
These nodules have been shown to contain Leishmania parasites, so that PKDL patients
become a reservoir of parasites
for future transmission.
12d,20,21
While most cases of PKDL present as severe dermatitis, the spread
of infection can lead to blindness (via the mucosal membranes) and
to nerve damage (primarily in Indian PKDL).
22
Early detection and treatment are crucial determinants of
the prognosis
for infected patients, and for prevention of transmission. Diagnostic
tests include direct parasite detection (by microscopic visualization),
use of PCR for quantification and determination of the infecting species
determination by PCR, serological tests, and antigen-detection tests.
12c,23
The presence of amastigotes can be microscopically observed in patient
lymph nodes, bone marrow, or splenic aspirates, and has been used
for both diagnosis and evaluation of successful therapy. Quantitative
assessment of parasite burden has been improved with use of PCR to
amplify Leishmania gene targets such as 18S rRNA,
the kinetoplast (mitochondrial) DNA, ß-tubulin, and cytochrome b.(23a,24) While direct
parasite detection
is the most dependable method for disease confirmation, complications
from hemorrhage during splenic aspiration (0.1% of individuals) do
arise, and examination requires high fidelity, skilled expertise,
and established laboratories for sample collection and evaluation.
12c,23a
Serological tests monitor specific antileishmanial antibodies and
include the direct agglutination test (DAT) or fast agglutination
screening test (FAST), indirect immunofluorescence assay test (IFAT),
and the rK39-based immunochromatographic test (ICT).
12c,23a
The antigen-detection tests represent an alternative to antibody
detection. KAtex, a latex agglutination test which detects a low molecular
weight glycoconjugate antigen in the urine of patients, shows high
selectivity for parasite, but has low sensitivity.
12c,23a,25
For HIV/VL coinfected patients,
diagnosis by direct visualization and quantification are highly reliable
and sensitive, as the parasite burden has been shown to be more than
10-fold higher in HIV-positive (versus HIV-negative) patients.
17,26
Diagnosis of PKDL is based on previous history of VL and results
from the various clinical and serological tests. As sample collection
(via tissue biopsy) is quite invasive and parasite loads tend to be
low in papulae, detection of infection is not always straightforward
and misdiagnosis of leprosy is common.
27
The splenic aspirate collection method is less invasive and is currently
shows the greatest promise for diagnosis of PKDL in a reliable and
noninvasive manner.
27
Overall, the
diagnostic tests need to be improved for greater sensitivity
and specificity, low cost and convenience, greater throughput, and
ease of sample collection and test administration.
12c,14,23a
Table 1
Leishmania Species
Reported to Cause Human Infections and Associated Leishmaniasis Syndromes
2.2.2
Cutaneous and Mucocutaneous
Leishmaniasis
The most common form of the disease, cutaneous
leishmaniasis (CL)
exhibits various clinical presentations dependent on the Leishmania species (Table
1) and the mode of transmission.
CL starts with an erythematous preulcer papule at the site of the
sand fly bite. This may self-cure within months or undergo slow-healing
with severe scarring.
28
Rarer manifestations
of CL include diffuse cutaneous leishmaniasis (DCL) and MCL, a life-threatening
condition.
28a,29
MCL is characterized by
disfiguring and destructive lesions of the mucosal membranes and is
usually observed months or even years after the CL lesions, in approximately
1–10% of CL patients.
13,28a,30
In addition to ulcerative lesions and erythema around the nose and
lips, MCL patients initially present with nasal congestion and nasal
septal granulomas (both anterior and posterior), lymphadenopathy,
fever, hepatomegaly, and scars from previous CL incidence. Later stage
MCL patients may exhibit additional complications within the nasal
cavity (edema, septum perforation) and periodontitis, with eventual
destruction of oronasopharyngeal mucosa and airway obstruction.
31
Diagnostic tests for the various forms
of CL are similar to those
used to identify VL and include parasite collection (cutaneous skin
scraping of center/margin of ulcer) and subsequent microscopic visualization
via Giemsa staining, punch biopsy, needle aspirate and parasite culturing,
serological antibody detection, and PCR quantification.
28a,29b
2.3
Epidemiology of Leishmaniasis
2.3.1
Visceral Leishmaniasis and Post Kala Azar
Leishmaniasis
There are two types of VL that are defined
by the causative Leishmania species and the parasite
reservoir. The zoonotic form, caused by L. infantum, occurs in the Mediterranean basin
and Central and South America
with dogs being the main parasite reservoir.
12d,15b,32
The more common anthroponotic
form is caused by L. donovani and is predominant
in India, Bangladesh, Nepal, and East Africa.
12c,12d
VL is endemic to rural areas of developing countries and has been
reported in approximately 98 countries in the world; 90% of all cases
occur in six countries in tropical/subtropical regions: India, Bangladesh,
Sudan, South Sudan, Brazil, and Ethiopia.
12c,12d
Approximately 300 000 new cases of VL occur each year leading
to an estimated 40 00 deaths. India has the highest incidence
of the disease with approximately 60% of all new cases occurring in
Bihar state.
12c,12d,14,33
Outbreaks are common during migration or
entry of naïve hosts into endemic areas and an increase in
the immunosuppressed patient population (such as with HIV) has contributed
to the escalation in VL incidence in East Africa.
15b
Additionally, an absence of implementation of cost-effective
control strategies makes VL a major public health concern.
12c
PKDL is prevalent in areas where L. donovani is endemic (India and East Africa) and
occurs
in 50–60% of Sudanese and 10–20% of Indian VL patients
within 6 months to 2–7 years after initial infection.
20,21,22a
Of these cases, approximately
15–20% (India) and 8% (Sudan) of patients do not have a history
of VL, indicating the existence of an asymptomatic infection.
22a,34
Few cases of PKDL caused by L. infantum or L. tropica have been reported.
35
It has been previously shown that the presence of a small population
of infected individuals (0.5%) may lead to a widespread epidemic of
VL infection in India and other regions of Asia; therefore, PDKL patients
play a major role in the spread of the disease, and parasite eradication
should be a high priority.
36,13
2.3.2
Cutaneous Leishmaniasis
Approximately
0.7 to 1.2 million cases of CL occur each year in the Americas, Mediterranean
Basin, the Middle East, and Central Asia. A large fraction (75%) of
CL patients reside in the following ten countries: Afghanistan, Algeria,
Colombia, Brazil, Iran, Syria, Ethiopia, North Sudan, Costa Rica,
and Peru.
33
The disease is caused by L. tropica, L. major, and L. aethiopica in the Old World
(Southern Europe, Middle East, Southwest Asia,
and Africa) or by L. mexicana, L. braziliensis and additional
Leishmania species in the New World (Central and South America,
Table 1).
15a,32
CL cases caused
by L. major and L. tropica (anthroponotic)
and by L. mexicana are characterized by papulae that
typically heal within a few months without medical intervention, whereas
CL caused by L. braziliensis is distinguished by
lesions that frequently metastasize to mucosal tissues (MCL) and are
treated with antileishmanial therapeutics.
15b,28a,32,37
DCL (L. amazonensis) and MCL are complications
of CL that occur primarily in the New World (90% of cases found in
Brazil, Bolivia, and Peru), respectively.
28a
An increasing number of CL cases have been reported in individuals
that have served in the military, international travelers, and endemic
area migrants.
37,38
Travels to Central and South
America account for approximately 40% of CL cases in tourists and
workers in the USA.
39
While some cases
of leishmaniasis introduced into industrialized nations involve VL,
greater than 80% of these are caused by CL. In fact, CL is one of
the most frequent skin disorders in the New World, and accounts for
around 60% of all cases in nonendemic areas.
40
With increasing travel, immigration, and military work in endemic
areas of this disease, the risk levels and incidence are predicted
to increase hence making implementation of precautionary measures
crucial in this selected group.
2.4
Current
Treatments
The focus of this
section is to discuss the drugs already in use for the treatment of
VL. These include pentavalent antimonials, pentamidine, various formulations
of amphotericin B, paromomycin, and miltefosine (Table 2 and Figure 1). As some of
the same
drugs are used for treatment of CL and MCL, the corresponding regimens
for these syndromes (including PKDL) are also briefly described when
applicable. Treatment of VL varies from one endemic region to another;
the WHO recommended regimens for major VL endemic foci are summarized
in Table 3. In general, as discussed earlier,
summarized in Table 2, and described in more
detail in the next sections the current treatment options are inadequate
and new chemical entities are urgently needed (target product profile
in Table 4).
Table 2
Overview of Existing VL Drugs
2.4.1
Pentavalent
Antimonials
Antimony
has been used as a therapeutic for several centuries. The first use
of antimony in the modern era dates to 1905, when trivalent sodium
antimonial tartrate was used to treat trypanosomiasis.
41
Use of the trivalent antimonials for the treatment
of CL was first reported by Vianna, and for VL by Di Cristina and
Caronia in Sicily, and Rogers in India in 1915.
42−44
Later this
drug was found to be highly toxic and exhibited side effects such
as cough, chest pain, and depression. The key breakthrough in the
use of antimony for the treatment of leishmaniasis was achieved in
1925 by Brahmachari, who synthesized the pentavalent antimony compound
urea stibamine and discovered it was an effective chemotherapeutic
agent against VL.
45
This discovery saved
millions of lives in India, especially in Assam state, where many
villages were depopulated by VL epidemics. Further progress in antimony
therapy of VL was achieved through synthesis of antimony gluconate
(Solustibosan) in 1937 and sodium stibogluconate (Pentostam) in 1945.
46,47
Currently, there are two formulations of pentavalent antimonials
in use: sodium stibogluconate (1) (100 mg antimony(SbV+)/100 mL) and meglumine antimoniate
(2) (85
mg antimony/100 mL). Both formulations have poor oral absorption and
are given via intramuscular injections or intravenous infusions.
48
Common side effects of pentavalent antimonials
include prolonged QTc interval, ventricular premature beats, ventricular
tachycardia, ventricular fibrillation, and torsades de pointes.
38b,49
Prolongation of QTc interval (>0.5 s) is often associated with
serious
or even fatal cardiac arrhythmias.
50
Arthralgia
and myalgia, elevated hepatic enzymes and pancreatitis are other common
adverse events.
51
Antimonial use causes
more toxicity and mortality in HIV-positive patients, compared to
HIV-positive patients treated with miltefosine or AmBisome, or HIV-negative
patients treated with antimonials.
52
In India, sodium stibogluconate was initially administered at low
doses of 10 mg/kg/day for 6–10 days.
53
These regimens were successful in curing most of the patients until
the late seventies, when several unconfirmed reports of unresponsiveness
appeared. In the eighties, clinical studies were done to determine
the most effective regimen and these concluded in the recommendation
in 1992 to treat VL in India with 20 mg SbV+/kg for 28–30
days.
39,54
During the 1990s and 2000s, the clinical
efficacy of antimonials in Bihar state (where ∼90% of VL cases
in India occur) gradually declined, and more than 60% of VL cases
in this state are now refractory to this treatment although the drug
continues to be effective in surrounding areas (e.g., Uttar Pradesh
state).
55
It is not established with certainty
what factors drove the emergence of antimony-resistant L.
donovani in Bihar. According to one hypothesis, the resistance
to antimonials emerged as the result of large scale misuse of the
drug in Bihar, where in one survey only 26% of patients were treated
according to the WHO guidelines.
56
The
alternative hypothesis is based on the observation that exposure of L. donovani to
low concentration of arsenic leads to emergence
of parasite resistance to pentavalent antimonials. Starting in the
1970s, there was a large scale tapping of aquifers in Bihar to provide
clean drinking water. The Bihari population was at risk from arsenic
exposure due to contamination from naturally occurring trivalent arsenic
in the groundwater. Thus, chronic exposure of the Bihar population
to arsenic in drinking water could have driven emergence of antimony-resistant L.
donovani strains.
57
Even though
pentavalent antimonials continue to be efficacious in other parts
of Southeast Asia, the WHO currently recommends alternative drugs
(AmBisome infusion) as the first line therapy options in this region.
32
As in India, VL in Africa is caused by L. donovani with major disease foci in Sudan,
South Sudan,
and Ethiopia, and
a lower number of cases found in Kenya and Uganda. Recommended treatment
consists of 20 mg/kg of sodium stibogluconate for 30 days.
58
This regimen typically yields >90% cure rates
in HIV-negative patients across the East Africa region.
59
However, monotherapy with pentavalent antimony
is not considered the first line treatment in East Africa according
to the WHO, which recommends combination treatment with pentavalent
antimony and paromomycin.
32
Unlike
in India and Africa, VL in South America is caused by L. infantum (formerly referred
to as L. chagasi). There is
no evidence of significant resistance to pentavalent
antimonials in Brazil and meglumine antimoniate is the first choice
for the treatment of mild and moderate cases of VL.
60
For severe cases (age less than six months or over 65 years
with signs of malnourishment, renal or hepatic insufficiency) and
pregnant women, the Brazilian Health Ministry recommends treatment
with liposomal amphotericin B (AmBisome).
61
A recent retrospective study focusing on a cohort of children treated
with 20 mg/kg per day meglumine antimoniate for 20–40 days
reported efficacy of 96.9% in mild-to-moderate cases, and over 60%
in severe cases.
60
VL in the Mediterranean
countries is caused by L. infantum as well. During
the 1990s, antimonials were the first-line of treatment
in most countries of this region (France, Greece, Italy, Malta, Spain,
Portugal, Albania, Israel, Turkey, Morocco, Algeria, and Tunisia)
with cure rates >95% in immunocompetent patients using regimens
of
20 mg SbV+/kg for 20–30 days.
62
More recently, pentavalent antimonials have been replaced
by AmBisome as the first line of treatment in European countries.
63
Most countries endemic for VL also have
HIV-infected populations
with the highest coinfection rates found in East Africa (up to 25–40%
in parts of Ethiopia) followed by Brazil (∼5%) and India (2–5%).
64
Use of pentavalent antimonials in HIV-infected
patients is no longer recommended by most experts in the field due
to their unacceptable toxicity in this patient group and high rates
of treatment failure.
52a,65
However, because of their low
cost, antimonials at a dose of 20 mg/kg for 28–30 days are
still used when alternative treatments are prohibitively expensive.
HIV infection has consistently been a predictor of poor outcome of
VL treatment (e.g., only 44% cure rate in HIV-positive versus 92%
in HIV-negative patients in one trial in Ethiopia) and associated
with high rates of relapse (15–57%).
65
Antimonials have also been used extensively as the primary
treatment
option for CL and ML, particularly in the New World where there is
a greater risk of mucosal involvement.
66
Administration is either by intralesion injections (limited to Old
World CL infections - up to 5 individual doses separated by 3–7
days) or systemically (20 mg/kg for 20 days for CL and 28–30
days for MCL). Several studies of this drug therapy indicate differences
in effectiveness, with 85–90% cure rates in Old World CL and
26%–100% in South America, depending on country and parasite
species.
67
2.4.2
Pentamidine
Pentamidine (3) has been in use since the 1940s for
treatment of sleeping
sickness.
68
The first use for VL treatment
was reported in India in 1949 and in Spain in 1950.
69,70
Most regimens are based on intramuscular injection or intravenous
infusion of 4 mg/kg of pentamidine (isethionate or methanosulfonate)
per day for a variable number (up to 30) of days. Safety is a major
concern with insulin-dependent diabetes mellitus being the most feared
and irreversible adverse event.
71
This
complication, while not uniformly reported, occurs in 4–12%
of cases. Additional side effects include hypoglycemia, hypotension,
fever, myocarditis and renal toxicity.
72
Pentamidine was used as the second line therapy for treatment
of antimony-refractory cases of VL in India. However, due to its toxicity
and rapidly emerging resistance (frequently to both pentamidine and
antimonials), pentamidine use in India was abandoned in the 1990s
and replaced with amphotericin B deoxycholate as the recommended treatment.
73
During the early years of increased pentamidine
use in India (1978), 10 injections were sufficient to effect cure
in all treated patients. By the early 1990s, 15 or more injections
were required to produce cure in only 67–77% patients.
74
More recently, pentamidine was successfully
used in several cases of HIV-positive patients to prevent VL relapse
following the initial treatment with an alternative drug.
75
Pentamidine is the first option for treatment
of CL caused by L. guyanensis and is recommended
as the first-line treatment
in French Guiana, and in Suriname, where it is the only available
antileishmanial. The typical treatment consists of a single intramuscular
injection of 7 mg/kg of pentamidine isethionate and can be repeated
48 h later in complicated cases. In one study these regimens yielded
78.8 and 83.6% cure rates, respectively.
76
2.4.3
Amphotericin B
Amphotericin B (4) is a polyene antibiotic isolated from Streptomyces
nodosus in 1955, which was identified because of its antifungal
activity.
77
In vitro activity of amphotericin
B on Leishmania was for the first time reported in
1960 and the first successful treatment of patients with VL was reported
in 1963 in Brazil.
78,79
The drug increases membrane permeability
by binding to ergosterol present in the Leishmania plasma membrane.
80
Amphotericin B is
used in complex with deoxycholate or various lipids and all formulations
are administered by intravenous infusion. The deoxycholate form of
the drug has many adverse effects including infusion reactions, nephrotoxicity,
hypokalemia, and myocarditis, and needs close monitoring and hospitalization
for 4–5 weeks. Lipid formulations of amphotericin B are efficacious
at lower doses and have reduced toxicity, but the high cost complicates
treatment of patients in low income settings.
81
In India, amphotericin B was traditionally a second line treatment
for VL, but decreased efficacy of antimonials and pentamidine led
to recommendation for use as a first-line treatment starting in 1990s
in Bihar. Amphotericin B deoxycholate has been used with different
dosing regimens, with a total dose ranging from 7 to 20 mg/kg, and
treatment administered on alternate days or daily for up to 43 days
at either constant or incremental dosing. Amphotericin B regimens
typically produce high cure rates (close to 100%) for both antimony-sensitive
and refractory infections.
82
Several lipid
formulations of amphotericin B (liposomal-AmBisome, lipid complex-Abelcet,
colloidal dispersion-Amphocil, lipid emulsion - Amphomul) have also
been tested; all enabling regimens with ∼100% cure rates.
83
Lipid formulations lead to the rapid concentration
of the drug in organs such as liver and spleen.
84
This greatly reduces adverse effects including nephrotoxicity
and allows delivery of large doses of the drug over short periods
of time. In an open label study in Bihar in 2010, a single dose of
10 mg/kg of AmBisome produced a 96.3% cure rate.
85
The outcome prompted the WHO to recommend this regimen
as the first line treatment for VL in South Asia.
32
Efficacy of amphotericin B deoxycholate in East Africa
(Uganda)
was extensively evaluated in 2003–2004 during an interruption
in supply of antimonial drugs. The regimen consisted of slow infusion
of 1 mg/kg of amphotericin B on alternate days for 30 days (total
dose 15 mg/kg) and produced a 92.4% cure rate.
86
Experience with AmBisome treatment in East Africa suggests
that higher total doses than in India are required to achieve >90%
cure rates. Treatment with 30 mg/kg AmBisome in 6 doses on alternate
days in Sudan produced a 92.6% initial cure rate in HIV-negative patients
but only 59.5% in HIV-positive group. AmBisome was even less effective
in HIV-positive VL relapses (38.0% initial cure, 55.7% parasitological
failure). Of additional interest, a study to determine the optimal
single dose of AmBisome (tested doses include 7.5, 10, 12.5, and 15
mg/kg) in HIV-negative patients in East Africa was concluded and the
results are expected to be published soon.
87
In Latin America, there is much less data on AmBisome’s
efficacy. In Brazil, a total dose of 20 mg/kg has been proven to be
efficacious.
88
The Pan American Health
Organization guidelines for treatment of leishmaniasis in the Americas
have established liposomal amphotericin B (3–5 mg/kg per day
IV for 3–6 days, with a total dose of 20 mg/kg) as one of the
first-line therapeutic options.
In Southern Europe, doses of
3–5 mg/kg per day, up to a
total of 20 mg/kg in different regimens, have been demonstrated to
be effective in up to 99–100% of patients. Total doses of 15,
18, and 24 mg/kg were tested in Italy, with response rates of 91,
98 and 100%, respectively. In Greece, one study administered a total
dose of 20 mg/kg in a short regimen of 2 days, with a cure rate of
98%, versus 90%, when it was administered over 5 days. Because of
the large number of published case series, there is an important accumulation
of evidence regarding the use of liposomal amphotericin B in pediatric
populations in Europe, with high response rates (97% with total doses
of 18–24 mg/kg in different regimens).
89
It has been shown that liposomal amphotericin B reduces the average
duration of hospitalization when compared with antimonials and that
it was effective in cases that did not respond to treatment with antimonials.
90
For all of these reasons and despite the absence
of randomized clinical trials, liposomal amphotericin B is considered
a reference treatment for VL in the Mediterranean countries in both
adults and children.
Amphotericin B deoxycholate (0.7 mg/kg
per day, by infusion, for
25–30 doses) and AmBisome (2–3 mg/kg per day, by infusion,
up to 20–40 mg/kg total dose) are also used for treatment of
CL and MCL infections caused by L. braziliensis and
other species, including L. guyanensis, L.
infantum, and L. aethiopica.(91) In a study completed by Solomon and colleagues,
a dosage of 18 mg/kg total given to patients afflicted with L. braziliensis CL resulted
in an approximately 85% complete
cure in patients within two months.
92
2.4.4
Paromomycin
Paromomycin (5) is an aminoglycoside broad-spectrum antibiotic, first isolated
in the 1950s from Streptomyces krestomuceticus. Paromomycin
inhibits proteosynthesis by binding to 16S rRNA.
93
It was shown to be efficacious for the treatment of CL
in 1966 and for VL in 1990 in Kenya.
94
The
most common adverse event with paromomycin is injection site pain
(55%); however, this typically does not lead to the discontinuation
of therapy. A small fraction of patients experience reversible ototoxicity
(2%) and a rise in hepatic transaminases (6%).
95
In a phase III study in Bihar in 2003–2004,
a paromomycin regimen of 11 mg/kg (15 mg/kg as the sulfate) i.m. for
21 days was shown to be noninferior to amphotericin B (1 mg/kg i.v.
alternate day for 30 days) with final cure rates of 94.6 versus 98.8%,
respectively.
95
The cure rate among those
previously treated with SbV+ or miltefosine was 98%. The
cure rate in pediatric patients was 96% and in females 95%. The main
advantage of paromomycin is its affordability: the cost of the treatment
is only ∼$10 per patient.
A study conducted in 5 centers
in Sudan, Kenya, and Ethiopia compared
the efficacy of paromomycin as monotherapy at a dose of 15 mg/kg per
day for 21 days, antimonials (20 mg/kg per day) as monotherapy for
30 days or the combination of both drugs for 17 days. At 6 months
after the end of treatment, paromomycin monotherapy provided only
a 63.8% average cure rate with very low cure rates observed in 2 Sudan
centers (14.3% and 46.7%).
96
A follow-up
study in East Africa evaluated paromomycin regimens of 15 mg/kg per
day for 28 days, and 20 mg/kg per day for 21 days with final cure
rates of 81% and 80%; however, both regimens were still inferior to
the standard treatment (20 mg/kg of sodium stibogluconate for 30 days
yielded a 94.1% cure rate).
97
There are
no reports on paromomycin use in VL treatment in Latin America and
Mediterranean countries.
Paromomycin in a form of ointment (15%
paromomycin/12% methylbenzethonium
chloride) is also used for the local treatment of noncomplicated Old
World CL by application to the lesion twice daily for 20 days. Experience
with paromomycin ointment for the treatment of New World CL is limited.
In one trial, 20 day treatment twice daily produced 70–90%
cure rates for CL caused by L. mexicana, L. panamensis, and L. braziliensis in Ecuador
and Guatemala.
98
More recently, a novel
paromomycin ointment was described (15% paromomycin, 0.5% gentamycin)
and found efficacious for CL treatment caused by L. major.(99)
2.4.5
Miltefosine
Miltefosine (6; hexadecylphosphocholine) was originally
developed as an
anticancer drug. In the 1990s, several laboratories discovered that
miltefosine has antileishmanial activity,
100
and in 2002, it was approved in India as the first oral treatment
of VL. The most common adverse events include gastrointestinal side
effects and occasional hepato- and nephrotoxicity. Another miltefosine
limitation is teratogenicity, and women of child-bearing age have
to take contraceptives for the duration of treatment and for an additional
3 months afterward due to the long half-life of miltefosine (∼1
week).
101
In 2002 a phase III trial
in India with a regimen of 50–100 mg/day for 28 days resulted
in a 94% cure rate, and miltefosine was selected for the VL elimination
program in India, Nepal, and Bangladesh.
102
However, a recent study suggests that miltefosine efficacy is starting
to decline and a study in 2012 yielded a reduced cure rate of 90.3%.
101
Miltefosine is also efficacious for treatment
of PKDL cases and the recommended regimen includes treatment with
50–100 mg/day for 12 weeks.
103
The efficacy of miltefosine in East Africa was determined during
a trial in Ethiopia in 2006. A regimen of 100 mg/kg per day of miltefosine
for 28 days was found to be equivalent to sodium stibogluconate treatment
(20 mg/kg per day for 40–60 days) in HIV-negative patients
(final cure rate of ∼94% for patients who could be traced during
follow up).
52a
A phase II trial to evaluate
the efficacy of miltefosine in Sudan and Kenya is ongoing.
Miltefosine
is considered to be the first effective oral treatment
regimen for CL, with greater accessibility and lower toxicity compared
to antimonials.
104
Miltefosine at a dose
of 2 mg/kg per day for 28 days is effective against CL in Colombia
caused by L. panamensis (70–90% cure rate),
but has only limited effect against the disease caused by L. braziliensis and L. mexicana
(<60%
cure rate). Treatment extension to six months for CL in Brazil originating
from L. braziliensis infection resulted in a 75%
cure rate compared to the 53% cure rate following treatment with antimony,
with efficacy shown to be greater in adults compared to children.
104
In Table 3 the
WHO regimens for the treatment
of VL and PKDL in various endemic regions are described.
Table 3
WHO Recommended Regimens for Treatment
of VL and PKDL in Different Endemic Regions
105
2.4.6
Ketoconazole
Azoles are oral antifungal
drugs that inhibit fungal ergosterol biosynthesis at the lanosterol
demethylase step resulting in the accumulation of 14 α-methyl
sterols. As Leishmania parasites rely on ergosterol
for their sterol needs and share this biosynthetic pathway with fungi,
azoles have been explored for their therapeutic potential against Leishmania infections.
For CL, the efficacy of compounds
varies depending on species.
106
Ketoconazole
(7) was tested for a month in both adults and children
on CL caused by L. braziliensis (either 600 mg or
100 mg daily, respectively, for 28 days) and resulted in a 76% cure
with mild side effects.
107
Similar
testing in patients afflicted with CL caused by L. mexicana resulted in 89% cure in
another study completed by Navin and colleagues.
108
Another ergosterol biosynthesis inhibitor,
fluconazole (8) (200 mg daily for 6 weeks), was also
previously tested in patients with CL originating from L.
major and resulted in 59% cure and shorter healing time for
patients residing in Saudi Arabia.
109
In
the case of itraconazole (9), minimal response rates
were observed in cases of CL resulting from L. major and in MCL originating from L.
braziliensis.(110) Among the several azole drugs tested (fluconazole,
itraconazole, ketoconazole), only ketoconazole was found to be consistently
efficacious and is now used for treatment of CL infections caused
by L. mexicana (600 mg per day for 28 days).
Figure 1
Current drugs
used for treatment of leishmaniasis.
2.4.7
Treatments with Drug Combinations
There are only a limited number of new chemical entities in the drug
development pipeline to address the limitations of the current VL
treatments. Instead, treatments with combinations of existing drugs
have become the main short to medium term strategy to combat emerging
drug resistance, reduce adverse events, and shorten therapy duration.
The earliest attempts to explore this approach occurred in the early
1990s, with a combination of sodium stibogluconate and paromomycin
tested in Kenya, Bihar state, and Sudan. A study in Bihar evaluating
combinations of various paromomycin and sodium stibogluconate doses
found that a combination of 12 mg/kg of paromomycin and 20 mg/kg of
sodium stibogluconate (both administered daily) for 20 days yielded
an 88% cure rate.
111
Seventeen day
treatment with the combination of sodium stibogluconate (20 mg/kg)
and paromomycin (15 mg/kg) in Sudan affected a 97% initial cure rate
and was found to be superior to sodium stibogluconate alone (20 mg/kg
for 30 days).
112
Similar results were also
observed in a subsequent East Africa multicenter trial, and this combination
regimen is now the preferred treatment in this region.
32,59
Another approach to combination treatment relies on sequential
use of 2 different drugs. During recent trials in India it was established
that a single infusion of 5 mg/kg of AmBisome followed by either 7
days of 50 mg/kg per day of miltefosine or 10 days of 11 mg/kg per
day of paromomycin both yielded 97.5% cure rates 6 months after the
end of treatment. As a part of this trial, a treatment arm with daily
coadministration of miltefosine and paromomycin (50 mg/kg and 11 mg/kg
per day, respectively) for 10 days was also evaluated and yielded
a 98.7% final cure rate.
101
In summary,
combination therapies have been established as safe and effective
treatment options and their implementation into primary treatment
centers in India and East Africa is ongoing.
Combination therapy
with antimonials has been used to enhance efficacy
for CL.
66
Allopurinol supplementation led
to a 2-fold reduction in the required antimony dosage and resulted
in a cure rate of 75–80% in Iranian patients infected with L. major and improved treatment
outcomes for patients treated
with a single agent while infected with L. tropica.(113) To treat L. braziliensis,
pentavalent antimony (15–20 mg/kg daily) has been used in
conjunction with pentoxifylline (400 mg, three times a day) for a
month to cure 90% of patients with MCL and lesions resistant to single
agent therapy.
114
Figure 2
Drugs that have been
repurposed for the treatment of leishmaniasis.
Table 4
Target Product Profile for VL (Adapted
from DNDi)
3
Drug Discovery
for Leishmaniasis
In spite of a large patient population,
leishmaniasis drugs have
led to poor economic returns as endemic areas are typically impoverished.
As a consequence there have been limited funds available to support
the research and development of new antileishmaniasis treatments to
address the liabilities of the current standard of care according
to the target profile shown in Table 4.
In order to bolster the pipeline a significant effort has been
applied in repurposing drugs from different indications. The repurposing
of drugs offers a short and fast path to reach patients and the cost
of development is greatly reduced. The drug repurposing strategy has
been summarized in the literature in several reviews and has been
shown to be very successful. Indeed several current treatments such
as miltefosine, amphotericin B, and pentamidine were previously approved
or primarily designed for other indications.
115,116
In section 3.1, we summarize the main drugs
and compound classes that have been recently considered for repurposing
in leishmaniasis.
As in other areas of infectious diseases most
of the novel chemical
entities are coming from phenotypic drug discovery campaigns rather
than target based efforts. Until recently, the screening of large
libraries using phenotypic readouts was nonexistent in the antileishmanial
field because of the complexity of biology as well as lack of resources.
New technological advancements have allowed the screening of large
libraries using phenotypic readouts and it is anticipated that these
screening efforts will yield new structurally diverse antileishmanial
compounds and will help identify new critical targets. Section 3.2 will describe the
recent advancements from phenotypic
efforts including compounds identified from screening of synthetic
compound libraries as well as natural product extracts followed by
isolation and chemistry modification. Efforts related to the modification
of existing anti-infective scaffolds are also described. Finally,
tremendous efforts have been put in the understanding of the Leishmania biology leading
to identification of numerous
putative targets. Section 3.3 discusses the
proposed essential targets and the compounds used as tools to validate
them.
3.1
Repurposing Efforts for Leishmaniasis
3.1.1
Tamoxifen
Tamoxifen (10) (Figure 2) is an estrogen receptor antagonist
which has been in clinical use for the treatment of breast cancer.
Tamoxifen has in vitro activity against L. braziliensis and L. infantum intracellular
amastigotes with
an EC50 of 1.9 ± 0.2 and 2.4 ± 0.3 μM,
respectively.
Treatment of L. braziliensis-infected
mice with tamoxifen at a dose of 20 mg/kg led to significant reductions
in lesion size and a 99% decrease in parasite burden when compared
with vehicle controls.
Treatment of L. infantum-infected hamsters with
tamoxifen led to significant reductions in liver parasite load and
a 95% to 98% reduction in spleen parasite burden. Furthermore, there
was a 100% survival rate for all animals treated with tamoxifen. In
contrast, all the vehicle-treated animals perished by 11 weeks.
117
In a similar experiment carried out for cutaneous
leishmaniasis, the infected mice were treated with tamoxifen (10), orally, at a dose
of 20 mg/kg/day for 15 days. Results
indicated that untreated infected mice suffered from autoamputation
of the inoculated foot pad. In comparison, the treated mice exhibited
marked improvement of the cutaneous lesions and reduction of overall
parasite load. However, the treated male mice showed scrotal swelling
with evident histopathological changes in the testes that could seriously
compromise fertility of the male mice.
In conclusion, while
tamoxifen (10) is able to cure
leishmaniasis infection in laboratory animals, it also causes significant
side effects to the male reproductive system in the mouse model.
118
3.1.2
PI3 Kinase Inhibitors
A series
of human phosphoinositide-3-kinase (PI3K) and mammalian target of
rapamycin (mTOR) inhibitors were investigated for activity against
the kinetoplastid parasites (Trypanosoma brucei, T. cruzi, and Leishmania sp). The
rationale
behind this study was based on the premise that both parasites and
humans express similar kinase enzymes. Thus, one could exploit the
extensive research on the human targets to repurpose compounds to
kinetoplastid infections. Among the inhibitors examined, NVP-BEZ235
(11), was found to have potent antileishmanial activity
in parasite cultures in submicromolar concentration. However, despite
its activity against L. donovani axenic amastigotes,
no efficacy was observed in in vivo mouse models at tolerated doses.
119
3.1.3
Nitroimidazoles
Nitroimidazoles
are a well-known class of pharmacologically active compounds, most
notably in the field of anaerobic bacterial and parasitic infections.
120
The most profiled antitrypanosomal drug
candidate in this class was megazol (12) (Figure 2), though development was stopped
due to mutagenicity
issues.
121
Continuing exploration of this
class of compounds led to the identification of fexinidazole (13) as an effective
antitrypanosomal agent. Fexinidazole is
currently in clinical trials for stage 2 HAT (see section 6.2.). Fexinidazole is rapidly
oxidized in vivo in
mice, dogs, and humans to the sulfoxide and sulfone metabolite. While
the parent compound is devoid of activity, both metabolites of fexinidazole
are active against intracellular L. donovani amastigotes.
A q.d. regimen for 5 days at 200 mg/kg dose led to a 98.4% suppression
of parasites in a mouse model of visceral leishmaniasis which is equivalent
efficacy to that seen with miltefosine. Overexpression of the leishmanial
nitroreductase homologue in L. donovani led to an
increase in sensitivity to fexinidazole by 19-fold, indicating that
reductive activation, via an NADH dependent bacterial-like nitroreductase,
is responsible for the activity.
122
Based
on the impressive efficacy, fexindazole is currently in phase II clinical
trials for visceral leishmaniasis.
Bicyclic nitroimidazole derivative
(R)-PA-824 (14)
shows potent cidal activity against L. donovani with
an EC50 of 160 nM and 930 nM against promastigotes and
intracellular amastigotes, respectively. In a murine model, (R)-PA-824
exhibits >99% suppression of parasite burden at a dose of 100 mg/kg
b.i.d when administered orally for 5 days. In contrast to fexinidazole,
transgenic parasites overexpressing the leishmania nitroreductase
are not oversensitive to (R)-PA-824 (14) indicating that
this enzyme is not involved in the mechanism of action of this compound
and some other unknown nitroreductase specific to leishmania species
might be involved. Thus, (R)-PA-824 offers the promise of being a
potential candidate for late lead optimization for VL.
123
Indeed, similar compound VL-2098 (15) is already in preclinical development for the
treatment of visceral
leishmaniasis and has the potential to further bolster the pipeline.
3.1.4
Nelfinavir
Reports of visceral
leishmaniasis co-occurring in individuals infected with human immunodeficiency
virus type 1 (HIV-1) are well documented.
124
A series of protease inhibitors (nelfinavir, ritonavir, and saquinavir)
were examined for their activity against various Leishmania species. While it was
observed that these protease inhibitors do
not inhibit the growth of Leishmania infantum promastigotes alone in culture, they
were found to significantly
inhibit the intracellular survival of parasites in phorbol myristate
acetate-differentiated THP-1 macrophages and human primary monocyte-derived
macrophages (MDMs) (65–79% inhibition). Furthermore, these
compounds were found to be equally active against a field isolate
of Leishmania donovani resistant to sodium stibogluconate
(SbV), suggesting that resistance to SbV does not result in cross-resistance
to protease inhibitors. Additionally, the ability of nelfinavir (16) (Figure 2) to
reduce the intracellular
growth of Leishmania parasites is also
observed in MDMs coinfected with HIV-1.
125
Further work into the mechanism of action suggests that nelfinavir
(16) induces oxidative stress in Leishmania amastigotes, leading to caspase-independent
apoptosis, in which
DNA is degraded by endonuclease G. These studies provide a rationale
to test nelfinavir (16) as a potential antileishmanial
agent as well as for possible future use in Leishmania/HIV-1 coinfections.
126
3.1.5
Imipramine
Imipramine (17) is a cationic
amphiphilic drug commonly used for the treatment
of depression in humans. Previous studies have shown that this compound
was able to decrease the mitochondrial transmembrane potential of L. donovani promastigotes
and purified amastigotes
as opposed to miltefosine where only a marginal change in potential
was observed.
127
Moreover it was found
to inhibit trypanothione reductase, an enzyme which is upregulated
in antimony resistant strains.
128
In addition,
as an effective immunomodulator, it was known to upregulate TNF-α,
which plays an important role in cytokine defense.
129
Different groups of hamsters infected with antimony sensitive
and resistant isolates were treated with imipramine at doses of 0.05,
0.5, and 5 mg/kg/day respectively for 4 weeks and while there was
no clearance of splenic and hepatic parasite load at 0.05 mg/kg, 50%
clearance was observed at 0.5 mg/kg and there were no detectable parasites
in animals dosed at 5 mg/kg. More importantly, organ parasite clearance
was similar for all isolates irrespective of their sensitivity toward
antimonials. No further development work has been reported on this
compound.
3.2
Antileishmanials from Phenotypic
Efforts
Phenotypic drug discovery has proven to be a successful
approach
for identifying new chemotypes and starting points for medicinal chemistry
optimization.
130
Moreover, the poor understanding
of relevant targets in the parasite field has led to poor success
rates when using a target based drug discovery approach, making a
phenotypic strategy particularly attractive in this context.
131
This broad approach offers the potential to
identify agents acting on a previously undescribed target or by acting
on multiple targets in tandem. The prospect of establishing new mechanisms
of action for antileishmanial activity is of growing importance as
drug treatment pressure has resulted in emerging parasite resistance.
132
Advances in chemical proteomics have
made subsequent target elucidation and the evaluation of therapeutic
intervention via this approach a viable alternative to target-based
approaches. However, it is important to discern between inhibitory
activity of interest and general cytotoxicity. Complementary assays
allow for the selection of candidate compounds with an adequate selectivity
index (SI), where the in vitro cytotoxicity in mammalian cells is
significantly less than the antiparasitic activity. However, while
general cytotoxicity can be easily established via such assays, a
particular drawback of phenotypic approaches is the uncertainty related
to mechanism-based toxicity.
In general, the utilization of
phenotypic assays and screens for
the identification of novel lead structures can be of greatest use
when using the appropriate parasite form under the relevant physiological
conditions, allowing for a reasonable probability that efficacious
compounds can be obtained.
Figure 3
Novel scaffolds resulting from phenotypic screens.
3.2.1
Lead Structures Resulting
from Phenotypic
Screens
In the context of Leishmania drug discovery efforts, compound screens using promastigotes,
axenic
amastigotes, or intramacrophage amastigotes have been explored. Each
of these assays offers a unique set of advantages and drawbacks. Promastigotes
have been used extensively for the purpose of screening compounds;
still the relevance of compounds active against them is in question
as they are only prevalent in the insect life-stage. Alternatively,
screening against axenic amastigotes offers the advantage of being
more similar to the disease-relevant parasite stage; however, there
are several cited examples of differences between axenic amastigotes
and intracellular amastigotes as well in terms of protein expression
and in terms of drug susceptibility. There are multiple reports of
high false positive rates from axenic amastigote screens where the
activity of the hits was not confirmed by using an intramacrophage
assay.
133
Ideally, one should employ an
intracellular assay which is the most physiological relevant assay
to find high quality hits. In one such effort, Mckerrow and co-workers
carried out a comparative screen on a 909-member library of bioactive
compounds against Leishmania donovani. The results
revealed 59 hits in the promastigote primary screen and 27 in the
intracellular amastigote assay, with 26 compound hits shared by both
screens. This result clearly indicated the promiscuity of promastigote
stage screens as well as the failure to identify all active compounds.
Interestingly compound 18 (Figure 3) inhibits intracellular but not axenic parasites,
suggesting a host
cell-dependent mechanism of action and would have been missed in a
screening using axenic amastigotes.
134
Cognizant of the technological difficulties associated with the screening
of a large number of compounds with an intracellular macrophage assay,
GNF adopted the strategy of running an axenic amastigote screen on
2.2 million compounds using a 1536 well format. This was followed-up
with a physiologically relevant intracellular assay to confirm the
activity of the hits. As expected, a low hit confirmation was obtained
with intracellular amastigotes, validating the observations about
the poor translatability of the axenic amastigote assay. Despite the
limitations of the assay, we are satisfied with the screen which resulted,
after reconfirmation, in a significant number of novel hits. One such
antileishmanial hit (19) has been pursued by several
groups for human African trypanosomiasis.
135
Despite many reports describing phenotypic assays against
various
leishmanial forms, there are few published reports of follow up to
these initial efforts.
133,134,136
In one such effort, a L. major promastigote screen
was carried out by Sharlow et al. and 31 compounds were picked up
for further characterization and were evaluated for in vitro activity
against intracellular L. donovani and L.
amazonensis parasites. Compounds 20 and 21 exhibited exceptional activity against
intracellular L. donovani in vitro with EC50 values of 21 and
260 nM, respectively. Moreover, the benzothiazole derivative 20 demonstrated low cytotoxicity
against Vero cells indicating
that the compound does not affect the mammalian cells at submicromolar
concentration. Administration of 20 and 21 at a dose of 1 mg/kg intraperitoneally
(i.p.) as a single dose for
5 days resulted in 44% and 42% reduction of liver parasitemia in L. donovani-infected
BALB/c mice. In this study, the control
groups also showed a 27–30% reduction in parasites, indicating
that the vehicle (2-hydroxypropyl)-β-cyclodextrin solution (HPβCD)
had antileishmanial activity on its own.
136a,137
In conclusion, benzothiazole-containing cyanine dyes do have some
activity; however, their potential as drugs remains in question given
the report of their interaction with DNA.
138
In another effort, the repurposing of a narrow range of N-benzoyl-2-hydroxybenzamides
from a Toxoplasma
gondii tachyzoite screen led to two salicyclamide examples
(22) (Figure 3) with reasonable
activity (<0.5 μg/mL) against L. donovani axenic amastigotes.
139
A small
compound library that was screened at a single concentration
using L. donovani axenic amastigotes, revealed a
paullone chemotype. The initial paullone hits from this phenotypic
screen, however, were found to be inactive in an L. donovani intracellular assay.
Cursory structural optimization of the parent
scaffold resulted in two 9-tert-butyl-paullone chalcones
(23) with demonstrated growth inhibition of L.
donovani axenic and also intracellular amastigotes, however,
through the integration of a well-established antileishmanial chalcone
moiety (vide infra), these specific compounds became less structurally
novel.
140
Based on the scarcity of
literature reports so far, one could infer
that to date very little progress has been made in identifying optimization-ready
leads from phenotypic screens. The lack of new leads could be attributed
to technological hurdles in running relevant biological screens or
due to the lack of resources with which to carry out the screening
of larger libraries and the subsequent synthetic follow-up necessary
to achieve a development candidate. However, there are indications
of active medicinal chemistry programs being pursued by various organizations
including us at GNF, the University of Dundee, and DNDi. This brings
hope that more starting points would be delivered from phenotypic
and other approaches in the near future. Based on the public profile,
DNDi is following up on numerous chemotypes in addition to backup
nitroimidazoles.
141
3.2.2
Natural Products
Natural products
derived from plants and animals have been of great interest in the
search for novel antileishmanial compounds. This interest can be attributed
to the potential identification of unique chemical architectures and
pharmacophores, and the often inherent “drug-like” properties
of isolates. Over the last three decades, 69% of all new small molecule
drugs for the treatment of infectious diseases have been derived from,
or inspired by, natural products.
142
While,
natural products represent interesting starting points for further
follow up, the complexity of the molecules often prevents broad optimization
efforts to further improve their properties. The greatest potential
of natural product hits lie in the identification of novel targets
which in turn can spur targeted drug discovery efforts. The extensive
antileishmanial potential of plant and marine based natural products
has been previously reviewed in the literature.
143−145
Figure 4
Antileishmanial
natural products and derivatives.
3.2.2.1
Plant- and Fungal-Derived Natural Products
Natural products from plants and fungi have proven to be a valuable
source of chemical matter for anti-infective programs. Typically,
the natural product of interest is isolated using activity based fractionation.
With large numbers of samples produced from typical plant extract
fractionations, it can be of great benefit to proceed with the use
of axenic parasites, where assays often have quick turnaround times.
In efforts searching for novel treatments for cutaneous leishmaniasis,
3(S)-16,17-didehydrofalcarinol (24)
(Figure 4) was identified by the axenic bioassay-guided
fractionation of the plant Sarcococca hookeriana and Tridax procumbens.
146
Similarly,
axenic L. amazonensis parasite-based assays demonstrated
the antileishmanial potential of the natural product parthenolide,
147
in addition to the two potent sesquiterpene
lactones (+)-8,13-diacetyl-piptocarphol (25) and (+)-8-acetyl-13-O-ethyl-piptocarphol
(26) (Figure 4), isolated from the extract of the traditional
medicine Pseudelephantopus spicatus.
148
As a result of described leishmanicidal potential
of Calophyllum brasiliense crude extracts,
149
and further investigations thereof, the coumarin
natural product (−)-mammea A/BB (27) was determined
to be a potent active component of C. brasiliense, with an EC50 of 0.88 μg/mL against
L.
amazonensis axenic amastigotes.
150
Dosing of (−)-mammea A/BB (27) for 30 days intramuscularly
led to significant reduction of lesion size compared to vehicle with
no observed side effects.
151
Efficacy in L. amazonensis-based in vivo models has also been demonstrated
with (−)-epigallocatechin 3-O-gallate (28), the most abundant flavanol constituent
of green tea,
where dosing in mice (30 mg/kg/d, 5 d/wk. over 52 days, p.o.) resulted
in substantial lesion size reduction.
152
Similarly, oral dosing of γ-fagarine (29) (10
mg/kg, 14 d), from Helietta apiculata, led to a 97%
reduction in parasite burden of L. amazonensis-infected
mice, and treatment of L. amazonensis-infected mice
with the bryophyte constituent 14-hydroxyunularin (30) (Figure 4), resulted in a 93%
reduction
in lesion parasite load (10 mg/kg, 15 days, s.c.).
153
Numerous natural products have also been reported
to successfully
affect in vitro those Leishmania parasites that are
the causative agents of visceral leishmaniasis. Examples include the
protoberberine natural product palmatine, active against L.
infantum,
154
and the quinonemethide
natural products maytenin (31) and pristimerin (32) (Figure 4), with demonstrated
activity
against L. chagasi.
155
Screens employing L. donovani promastigotes are
also prevalent and have identified a wide range of promising antileishmanial
natural products (EC50 < 1 μg/mL) from the plants Plumbago zeylanica,
156
Septoria pistaciarum,
157
Abrus schimperi,
158
Prosopis
glandulosa var. glandulosa,
159
Clerodendrum eriophyllum,
160
and Uvaria grandiflora.
161
Reports utilizing axenic amastigotes validated
the potent natural product preussomerin EG1 (33).
162
A L. donovani intracellular
amastigote assay revealed the potential of the taxoid 10-deacetylbaccatin
III (34) (Figure 4), isolated
from Taxus baccata, with demonstrated potent in vitro
activity (EC50 value of 0.07 μM) and an SI value
of >10, contrary to taxol, which is cytotoxic at nanomolar concentrations.
163
3.2.2.2
Animal-Derived Natural
Products
Among the many animal-derived isolates with observed
antileishmanial
activity, most are derived from marine invertebrates or associated
bacteria. As a result of screening a range of marine organism extracts
against L. amazonensis promastigotes, the promising
natural product cristaxenicin A (36) (Figure 4) was isolated (EC50 = 0.09 μM).
164
Analogous investigation of the bioactive crude
extract of the sponge Plakortis angulospiculatus afforded
small amount of the natural product plakortide P, with good activity
against L. chagasi intracellular amastigotes and
respectable cytotoxic selectivity.
165
There
are also reports of antileishmanial activity from the venom of the
scorpion Tityus discrepans against L. mexicana promastigotes,
166
and crude venom from
the snake Bungarus caeruleus.
167
However, no active components were isolated.
3.2.3
Natural Product Derived Compounds
Systematic exploration
of the structure–activity relationship
of antileishmanial natural products has led to a variety of semisynthetic
efforts, where defined natural pharmacophores effectively provided
a pedestal for synthetic manipulation and were leveraged for potential
compound improvement. A comprehensive approach toward obtaining appropriate
clinical candidates via this method is often hindered, however, by
the structural complexity of isolated natural products and the relatively
small amount that can be isolated in certain cases (vide supra).
Hydrogenation of the antileishmanial coumarin natural product (−)-mammea
A/BB (27) (EC50 = 3.0 μg/mL), obtained
from the extract of C. brasiliense, provided the
more potent synthetic derivative 37 (Figure 4), with an EC50 of 0.37 μg/mL against
L. amazonensis promastigotes.
168
Similarly, synthetic esterification of the phenolic marine natural
product isoaaptamine (EC50 = 0.7 μg/mL), available
from the sponge Aaptos sp. in gram quantities, resulted
in two derivatives (38) with improved EC50 values (0.4 μg/mL and 0.1 μg/mL) against
L.
donovani.
169
Due to potent activity
against intracellular L. donovani amastigotes, 8,8-dialkyldihydroberberine
derivatives (39) (Figure 4) were
further explored in vivo. Unfortunately subpar efficacy was observed
upon i.p. dosing in a murine model for 5 days likely due to poor pharmacokinetic
properties.
170
In many such cases further
optimization is impaired by the resources required for structural
modification of such complex molecular architectures.
3.2.4
Derivatives of Anti-Infective Scaffolds
Due to the
limited understanding of leishmanial biology, it has
been typical to proceed in the rational design of leishmanicidal agents
through the inspiration and modification of structural classes already
known to possess anti-infective activity.
Figure 5
Antileishmanial benzoxazole
and imidazole derivatives.
3.2.4.1
Benzoxazoles
The report of potent
antibacterial activity demonstrated by the natural product A-33853
(40) (Figure 5) prompted the hypothesis
that similar compounds could be evaluated as novel anti-infective
agents. Synthetic analogs of A-33853 (40) were subsequently
found to be remarkably potent against L. donovani axenic amastigotes with compound
41 demonstrating an
EC50 value of 0.31 μM and SI value of 99.
171
3.2.4.2
Imidazoles
Imidazole-containing
compounds have received considerable attention in the search for leishmaniasis
chemotherapy due to the success of agents such as ketoconazole, miconazole,
econazole, and clotrimazole in treating fungal infections, thus lending
credence to the possible utility of this broad class of compounds
in other types of infection. Analogs of the imidazole antifungal agent
clotrimazole (42) have demonstrated effective Leishmania inhibition when combined
with metals. Clotrimazole
(42) was incorporated into a pseudo-octahedral ruthenium-clotrimazole
complex, [RuII(η6-p-cymene)Cl2(clotrimazole)] (43), (Figure 5) that was found to exhibit
very good in vitro activity against L. major promastigotes (EC50 = 0.015 μM)
and intracellular amastigotes (EC70 = 0.029 μM) with
an SI value of >500.
172
Analogs
of
the antifungal agents miconazole and econazole have also been explored.
A report that examined the anti-infective nature of analogs of miconazole
and econazole found that a range of synthesized imidazoles tested
against L. donovani intracellular amastigotes provided
good antileishmanial activity, with two examples (44)
exhibiting EC50 values of <0.5 μg/mL. Efficacy
of both of these compounds in vivo demonstrated moderate reduction
of parasitemia (52% and 60%) in a hamster model (50 mg/kg, 10 d, i.p.),
suggesting some potential for this compound class.
173
Figure 6
Antileishmanial chalcone derivatives.
3.2.4.3
Chalcones
Chalcones demonstrate
a wide range of pharmacological anti-infective activity, making this
substructure an attractive pharmacophore from which to explore antiprotozoal
SAR. A small set of chloro-substituted 1-(6-methoxy-2H-chromen-3-yl)-3-phenylpropen-1-ones
were found to have significant
antileishmanial activity. Three such compounds (45) (Figure 6) demonstrated EC50 values
of <1 μM
against the promastigote form of L. major.
174
A synthetic polysubstituted chalcone 46 demonstrated good activity against L. amazonensis
promastigotes (EC50 = 1.1 μM) and intracellular
amastigotes (EC50 = 0.9 μM). The compound was also
found to be active against L. braziliensis (EC50 = 1.4 μM) and L. peruviana (EC50
= 4.0 μM). However, upon dosage in vivo, 46 led to only a 25% reduction in parasite
burden in L. amazonensis-infected mice when treated for 6 weeks intralesionally (5
mg/kg).
Compound 47 was much less active against intracellular L. amazonensis amastigotes
(EC50 = 24.0 μM)
but resulted in a 92% reduction in parasite burden in vivo upon intralesional
dosing for 4 weeks (5 mg/kg). Despite the in vivo reductions in parasite
burden for this group of synthetic chalcones, no significant differences
in lesion diameter were observed relative to untreated controls.
175
Figure 7
Diamidine-containing leishmanicidal derivatives.
3.2.4.4
Diamidines
The effective treatment
of leishmaniasis with the diamidine drug pentamidine has led to the
investigation of a wide range of diamidines for their anti-infective
potential. The diamidine pharmacophore has been researched extensively
and its role in medicinal chemistry has been previously reviewed.
176
The synthesis of pentamidine analogs,
where the amidine moiety is cyclized into a benzimidazole substructure
akin to the known anthelminthic agents mebendazole and albendazole,
yielded hybrid structures with antiparasitic activity (48) (Figure 7).
177
In a reported antiprotozoal SAR study where the diamidine moiety
was incorporated into an imidazoline substructure and a cadaverine
linker was utilized, the resulting derivative 49 displayed
broad antiparasitic activity.
178
Conformationally restricted diamidine derivatives have also shown
to inhibit Leishmania growth. Synthesized diamidine
compounds with an m-terphenyl core displayed encouraging
activity in vitro; however, when these promising compounds were tested
in vivo in L. donovani-infected mice, two led to
adverse effects in uninfected animals, and dosing with a third compound
(50) resulted in only a 23% inhibition of liver parasitemia
(30 mg/kg, 5 d, i.p.). Also disappointingly, two promising compounds
(51) that demonstrated good activity against L. donovani axenic amastigotes, showed
no activity in L. amazonensis-infected macrophages.
179
Figure 8
Dimers containing amino and aminoalcohol linkers.
3.2.4.5
Amino and Aminoalcohol
Linkers
Napthalimide and its derivatives are generally known
to have anticancer
activity in a variety of human and murine cell lines.
180
In an effort to discover antiparasitic compounds
with adequate aqueous solubility, nitrogen- and oxygen-containing
linkers have been utilized to enhance conformationally flat and otherwise
insoluble chromophores. When this strategy was employed to join naphthalimide
groups via nitrogen-containing linkers of various lengths, one compound
(52) (Figure 8) was found to demonstrate
selective activity against L. infantum promastigotes.
181
Similarly, flavones are known to have a wide
ranging activity and known to perturb a variety of enzymes.
182
The synthesis of dimers containing flavonoid
chromophores joined by PEG- and amino PEG-linkers resulted in the
identification of a highly active lead compound (53)
with 0.13–0.21 μM activity (EC50) in wild-type,
sodium stibogluconate-resistant, and pentamidine-resistant L. donovani promastigote
strains, making it an attractive
foundation for the development of a visceral leishmaniasis treatment,
irrespective of parasite drug sensitivity.
183
Figure 9
Nitroheterocycles
and organophosphate antileishmanial agents.
3.2.4.6
Nitroheterocycles
The synthesis
of structural hybrids, utilizing the nitro-furan moiety as found in
the antitrypanosomal agent nifurtimox and the antileishmanial benzamidine
pharmacophore, yielded two highly potent derivatives (54) (Figure 9) with activity
against L. major promastigotes and intracellular amastigotes.
184
Additionally, the synthesis of hybrids of the
nitro-containing antiprotozoal agent megazol and the antileishmanial
combretastatin-type pharmacophore, yielded compound 55 that demonstrated potent activity
against L. donovani axenic amastigotes with an EC50 value of 0.08 μg/mL
and an SI value of 240.
185
3.2.4.7
Phospholipids
The teratogenic
nature of miltefosine and the potential for resistance as a result
of its long half-life (extended presence of subtherapeutic concentrations)
have prompted the desire to find more efficacious and/or less toxic
congeners. As miltefosine was originally developed as an antitumor
agent, there is only limited knowledge of miltefosine’s SAR
with respect to antiparasitic activity. One of the more promising
analogs is compound 56 (Figure 9), which demonstrated a >9 fold improvement in potency
relative
to
miltefosine in the promastigote assay, as well as lower cytotoxicity
and hemolysis improvements when compared to the parent drug.
186
However, while the gains in potency of newer
analogs might seem impressive, very little is known about these compounds
with respect to their teratogenicity or their activity on isolates
which are resistant to miltefosine.
Figure 10
Antiparasitic triphenylmethane and rhodacyanine
compounds.
3.2.4.8
Triphenylmethanes
The known anthelmintic
and antifungal compound gentian violet (57) (Figure 10) has been previously demonstrated
to exhibit antileishmanial
properties.
187
Synthetic efforts incorporating
the triphenylmethane pharmacophore, have yielded a range of compounds
with EC50 values of <1 μM. When examined in vivo,
compound 58 also demonstrated a 1000-fold in vivo reduction
in parasite burden in a murine cutaneous leishmaniasis (L.
amazonensis) model, and analogous application of gentian
violet (57) led to a complete elimination of parasites
(1% gel, b.i.d., 20 days, topical), highlighting the therapeutic potential
of triphenylmethanes and structurally similar electron carriers.
188
3.2.4.9
Rhodacyanines
The antileishmanial
potential of rhodacyanines has been previously described,
189
prompting the further investigation of the
SAR of this class of delocalized lipophilic cation compounds. In a
recent report, synthesized rhodacyanine compounds 59 and 60 demonstrated highly potent
activity in vitro against L. donovani intracellular amastigotes with EC50 values of
0.35 and 0.08 μM, respectively. Despite being less
potent, the efficacy of compound 59 was found to be superior
to 60 in vivo when the compounds were dosed intraperitoneally
at 50 mg/kg in L. donovani-infected mice (31% versus
18%). The efficacy of compound 59 could also be enhanced
with intravenous administration, leading to a 97% (4.1 mg/kg, i.v.)
reduction in liver parasitemia after dosing for 5 days.
190
Figure 11
Antileishmanial β-carboline and quinone
derivatives.
3.2.4.10
β-Carbolines
The natural
product canthin-6-one has been demonstrated as an active leishmanicidal
agent both in vitro and in vivo,
191
rendering
the β-carboline pharmacophore attractive for the investigation
of further antiparasitic SAR. Examination of a range of synthesized
canthin-6-ones and 1-phenyl-β-carbolines revealed that, in general,
leishmanicidal activity was more pronounced for the latter class of
compounds. In particular, compound 61 (Figure 11) displayed significant antileishmanial
activity,
with an EC50 value of 0.25 μM against L.
amazonensis promastigotes.
192
3.2.4.11
Quinones and Iminoquinones
The
quinone moiety and analogous derivatives are pharmacophores that have
been previously shown to exhibit significant activity against Leishmania. The antileishmanial
naphthoquinone compounds
diospyrin, plumbagin, lapachol, and buparvaquone exemplify the potential
of this structural class
193
and have made
the derivatization of quinone-type architectures alluring. In a recent
report, synthesized iminoquinone compound 62 (Figure 11) resulted in 99% and 78% reductions
in the murine
parasite (L. infantum) burden in the liver and spleen,
respectively (10 mg/kg, i.p.), and was found to be relatively nontoxic.
Additional iminoquinone derivatives, however, were found to be ineffective
in reducing parasitemia.
194
In another
report, a small library of 2-phenoxy-1,4-anthraquinones (63) was synthesized via a
parallel approach, with the intent of combining
the naphthoquinone pharmacophore with the substituted phenolic moiety
present in the structure of the known antibacterial and antifungal
agent triclosan. These hybrids (63) were observed to
have reasonable activity against L. donovani axenic
amastigotes; however, the SI values for this group of compounds were
generally poor (<15).
195
Figure 12
Heterocyclic
salts active against Leishmania.
3.2.4.12
Heterocyclic Salts
A small set
of synthesized pyridinium salts (64) (Figure 12), similar in structure to the bioactive
marine
natural products viscosaline and theonelladin C, were found to be
only moderately active against L. amazonensis and L. braziliensis promastigotes; however,
they were remarkably
specific against the intracellular form of the parasite.
196
Similarly, an antileishmanial screen of synthetic
derivatives of the bioactive natural product agelasine D led to the
discovery of two potent imidazolium compounds 65 and 66 with EC50 values of 0.09 and
<0.11 μg/mL,
respectively, against L. infantum intracellular amastigotes.
197
Figure 13
Compounds containing pyrimidine/triazine pharmacophore.
3.2.4.13
Pyrimidines and Triazines
Pyrimidine-
and triazine-type scaffolds have been of great interest in the search
for novel antiprotozoal agents due to the successes of representative
anti-infective compounds like pyrimethamine, cycloguanil, and trimethoprim.
Inspiration from these architectures, and subsequent hybrids thereof,
has yielded a series of promising synthetic antileishmanial derivatives.
The synthesis of quinazolinone-pyrimidine derivatives led to the discovery
of the reasonably potent compound 67 (Figure 13) with an EC50 value of 0.65 μM
against intracellular L. donovani amastigotes.
198
Additional synthetic pyrimidines (68) have been demonstrated to be efficacious in
vivo, with each compound
leading to 78% parasite inhibition when dosed in L. donovani-infected hamsters for
5 days (50 mg/kg, i.p.).
199
Efforts to hybridize the triazine pharmacophore with that
of the ether linkage of pentamidine led to the synthesis of two compounds
(69 and 70) with good activity on intracellular L. donovani amastigotes (EC50 values
of <1
μM). Efficacy of compound 69 in vivo, however,
was only found to be moderate, with a 63% reduction in hamster splenic
parasite (L. donovani) burden when animals were dosed
for 5 days (50 mg/kg, i.p.).
200
Figure 14
Antiparasitic
quinoline compounds.
3.2.4.14
Quinolines
The clinically relevant
antileishmanial therapeutics sitamaquine, primaquine, and imiquimod
highlight the significant potential of quinoline substructures. The
role of quinolines as leishmanicidal chemotherapeutic agents has been
specifically reviewed.
201
Taking advantage
of the privileged quinoline-type core, a substituted quinoxaline 1,4-di-N-oxide (71)
(Figure 14) was found to effectively inhibit the growth of L. amazonensis axenic amastigotes
with an EC50 of 0.7 μM.
202
Similarly, a class of 7-chloro-4-quinolinyl
hydrazones was found to be broadly active against a range of Leishmania promastigotes
with seven compounds (72) demonstrating EC50 values of <0.5 μg/mL.
203
Additionally, the synthesis of 4-substituted
pyrrolo[1,2-a]quinoxalines resulted in two compounds
(73), with EC50 activity against promastigotes
of 0.5 (L. amazonensis) and 0.6 μM (L. infantum).
204
Synthesis
and evaluation of N-quinolin-8-yl-arylsulfonamides,
structurally similar to sitamaquine, yielded three compounds (74) with good activity
against L. amazonensis (EC50 = 2–3 μM) and L. chagasi (EC50 = 0.4–0.6 μM) promastigotes.
Moreover
when a similar compound, 2,5-dichloro-N-(quinolin-5-yl)benzenesulfonamide,
was employed as a ligand in the formation of a copper complex, the
resulting organometallic species 75 was found to be highly
active with an EC50 value of 0.35 μM on L.
braziliensis intracellular amastigotes, and an SI value of
>100.
205
Also, the synthesis of a series
of 2-substituted quinoline derivatives revealed the promising compound 76, which demonstrated
an IC50 of 0.22 μM
against L. donovani intracellular amastigotes and
was also found to inhibit parasitemia in hamsters by 84% when dosed
orally (50 mg/kg, b.i.d.) over 5 days, despite exhibiting very low
bioavailability in mice.
3.3
Targeted
Approaches toward Novel Leishmaniasis
Therapies
Species within the genus Leishmania have been the focus of target based drug discovery
by numerous groups.
A large number of targets have been proposed; however, there have
been relatively few medicinal chemistry campaigns. This subsection
attempts to capture relevant efforts that have been reported in the
literature over the last five years. Recent reviews describing Leishmania targets
have also been published (Table 5).
143a,156,206
Table 5
List of Targets Identified (Not Described
in Review) for Leishmania Species
pathway/target
Leishmania species
refs
DNA binders
L. amazonensis, L. mexicana
(207)
protein synthesis
L. donovani, L. major
(208)
sterol 24-methyltransferase
L. amazonensis, L. donovani
(209)
CYP P450 enzyme 14-α-demethylase
L. tropica, L. amazonensis, L. braziliensis
(116)
farnesyl pyrophosphate
L. major
(210)
glyoxalase
pathway
L. donovani
(211)
Glycosylphosphatidylinositol
(GPI) pathway
L. mexicana
(212)
Leishmania β-1,2-mannosyltransferase
L. mexicana
(213)
oligopeptidase-B
L. donovani
(214)
pyruvate
kinase
L. mexicana
(215)
Leishmania
MAP kinase homologue
(LMPK)
L. mexicana
(216)
N-myristoyl
transferase
L. donovani
(217)
nitroreductase
L. donovani
(218)
nucleoside
hydrolase
L. donovani
(219)
adenosine
kinase
L. donovani
(220)
nucleoside
diphosphate kinase b
L. major
(221)
protein
disulfide isomerase
L. major
(222)
S-adenosylhomocysteine
hydrolase
L. donovani
(223)
methionyl-tRNA
synthetase
L. major
(224)
tyrosyl-tRNA
synthetase
L. major
(224a)
uridine-5′-monophosphate
synthase
L. donovani
(225)
deoxyuridine
triphosphate
nucleotidohydrolase
L. major
(226)
dihydroorotate
dehydrogenase
L. major
(227)
aldolase
L. mexicana
(228)
glucose-6-phosphate
isomerase
L. mexicana
(229)
glycerol-3-phosphate
dehydrogenase
L. mexicana
(230)
phosphomannomutase
L. mexicana
(231)
nicotinamidase
L. infantum
(232)
triosephosphate
isomerase
L. donovani
(233)
thiol-dependent
reductase
L. major
(234)
cysteine
synthase
L. major
(234)
deoxyhypusine
synthase
L. donovani
(206b)
sphingolipid
biosynthetic
pathway
L. amazonensis
(235)
metacaspase
L. donovani
(236)
cytochrome-c-oxidase
L. donovani
(237)
Figure 15
Structures of imatinib
(77) and berberine chloride
(78).
Table 6
Kinase
Inhibition and Antileishmanial
Activity of 79 and 80
3.3.1
Kinases
The
relevance of kinases
in drug discovery is well documented, particularly in the field of
oncology. Aberrant activation of kinases has been linked to proliferation
of certain cancer cells. For example, activation of Abelson tyrosine
kinase (Abl) has been linked to chronic myeloid leukemia. Small molecules
such as imatinib (77) (Figure 15) are known to inhibit Abl thus leading to cancer
cell death by apoptosis.
Inspired by the successes in oncology, a number of efforts have been
carried out in the field of parasitic diseases targeting kinases.
238
Based on homology studies, the kinome of L. major contains 179 genes encoding putative
homologues
of eukaryotic protein kinases (ePKs) and 17 encoding atypical protein
kinases.
239
While druggability of the kinase
target is not in question, questions persist regarding achieving a
selective kinase inhibitor which targets only the leishmania species
and not the host. This is not an impossible task as there are recent
examples from the antimalarial field where selective compounds have
been achieved.
240
Berberine chloride
(78), a quaternary isoquinoline alkaloid, is known to
have antileishmanial activity both in vitro as well as in vivo in
hamster models.
241
Recently, it was unraveled
by Western blot phosphorylation studies that berberine chloride (78) was responsible
for time dependent activation of p38 MAPK
along with deactivation of ERK1/2.
242
While
berberine chloride has proven to be a valuable tool compound in understanding
the mechanism of action its development as a drug is hampered by its
poor physicochemical properties. However, validation of the MAPK pathway
opens up the possibility of a target based approach in the future.
Cyclin dependent kinases or CDKs represent another interesting
subclass of kinases as potential drug targets because of their ability
to affect the cell cycle. Analysis of the genome from L. major has revealed the existence
of 11 CDKs. Moreover, 11 putative cyclins
(CYC2-11 and CYCA) have also been identified. Interestingly, among
the kinetoplastids, only Leishmania possesses cyclin
CYCA, a cdc-2 related serine/threonine protein kinase, which is essential
for transition through the G2-M phase of the Leishmania cell cycle. A CRK3:CYC6 protein
kinase assay was developed and two
groups followed up on this target leading to the identification of
potent enzymatically active compounds 79 and 80 (Table 6). However, there was a poor
correlation
between the observed enzymatic activity and cellular potency.
238c,243
Table 7
Activity of 2,4-Di-aminoquinazolines
on Folate Pathway Enzymes
a
L. major promastigote
assay.
b
L. donovani amastigote
assay.
Table 8
Inhibition
Constants on Leishmania
pteridine Reductase Inhibitors
3.3.2
Folate Biosynthesis
The folate
biosynthesis pathway has been a successful target for cancer and malarial
chemotherapy. Folates are essential cofactors in a variety of metabolic
pathways such as DNA and RNA synthesis and amino acid metabolism.
Two enzymes which are of particular interest in this pathway are thymidylate
synthetase (TS) and dihydrofolate reductase (DHFR). In trypanosomatids
these enzymes exist as single polypeptides (DHFR-TS), with the DHFR
domain on the amino terminus and the TS domain on the carboxy terminus.
It was discovered that most of the known DHFR inhibitors are inactive
against Leishmania. This can be explained by the
amplification of the PTR1 gene in some mutants. PTR1 can reduce both
pterins and folates and is much less susceptible to inhibition by
antifolates.
244
In order to overcome this
bypass mechanism, it was envisaged to design compounds which inhibit
both DHFR-TS and PTR1 enzymes. Hardy and co-workers were able to identify
compounds which were effectively able to inhibit both enzymes. However,
there was little correlation between potencies on PTR1 or DHFR-TS
and activity in the whole cell assay.
245
Compounds 82 and 83 are more potent in
the promastigote assay, while exhibiting mediocre potency on the targets
of interest (Table 7). This suggests that there
may be other targets for this class of compounds. In contrast, compound 81 exhibits
whole cell potency which is in agreement with
the enzymatic assays. Recently, Gilbert and co-workers were able to
design and optimize 2,4-diaminoquinazolines, such as 84, as inhibitors of dihydrofolate
reductase. While the synthesized
compounds exhibited potent activity against L. major DHFR, there was only relatively
weak inhibition of L. donovani axenic amastigotes despite activity on T. cruzi and
T. brucei. Lack of cellular activity on L. donovani can possibly be explained by the
low pH of the
medium which prevented diffusion of basic compounds into the parasites.
246
The activity of 84 on the PTR1
enzyme was not examined in the study (Table 7).
In order to overcome PTR1 resistance, a series of inhibitors
of PTR1 (quinazolines 85 and 86) were synthesized
and tested in combination with pyrimethamine (a known DHFR inhibitor)
(Table 8). Both 85 and 86 were only weakly active on L. mexicana as well
as other L. major strains when tested alone but showed
a profound parasite reduction when tested in combination with pyrimethamine.
247
Leishmania protozoans are autotrophic
for folates and unconjugated pteridines and rely on their host and
insect vectors to provide them. Unlike other organisms there are no
choke point enzymes and multiple bypass mechanisms exist. A suitable
molecule has to target DHFR-TS and PTR1 enzymes simultaneously while
maintaining selectivity against mammalian targets. Despite numerous
efforts, such an inhibitor with good efficacy in vivo remains elusive.
Figure 16
Representative
inhibitors of trypanothione, cyclophilin, and purine
salvage pathways.
3.3.3
Trypanothione
Pathway
The trypanothione
pathway is downstream to the polyamine pathway which synthesizes spermidine,
a key molecule for the synthesis of trypanothione. Trypanothione (bis(glutathionyl)
spermidine) is an essential molecule for modulating oxidative stress
in parasites. Trypanothione synthesis is catalyzed by two key enzymes,
namely trypanothione synthetase (TS) and trypanothione reductase (TR).
TS is responsible for the synthesis of trypanothione from spermidine
and two molecules of glutathione.
248
Trypanothione
is then maintained in its reduced state by the enzyme trypanothione
reductase using NADPH as the cofactor. Trypanothione in reduced form
then reduces tryparedoxin (TX) which is then followed by reduction
of tryparedoxin recycling enzyme tryparedoxin peroxidase (TP). It
has been shown that TR, TS, and TP are essential targets for the survival
as well as infectivity of parasites.
249
However, trypanothione reductase has structural similarity with
its human homologue glutathione reductase, which could make it difficult
to design selective analogues against this enzyme.
206b,250
The efforts on trypanothione pathway enzymes have been the
focus of several past reviews.
250,251
Recently pyrrole compound 87 (Figure 16) was identified to be
a competitive inhibitor of trypanothione reductase with a K
i of 4.6 μM. The compound also showed
activity on L. donovani intracellular amastigotes
with an EC50 of 13 μM. However, the compound was
equally cytotoxic on KB cells. The X-ray structure of the compound
with the trypanothione complex shows that compound 87 binds to the trypanothione binding
site, thereby impeding substrate
entry which explains the competitive nature of its inhibition.
251a
In a separate effort, a combinatorial
library of quinone–polyamine
conjugates was designed based on phenotypic T. brucei hits and conjugated with polyamine
derivatives to optimize their
antitrypanosomatid profile. The best compound from this series (compound 88) was found
to have trypanothione reductase activity along
with the ability to reduce cytoplasmic ATP and mitochondrial potential.
In addition to T. brucei activity, the compound showed
activity on L. donovani amastigotes as well as promastigotes
in the 2–3 μM range with a SI index of 2–3 for
cytotoxicity on L6 cells.
252
Mesoionic
heterocycles have been linked to a variety of biological
activities as a result of their ionic character and high dipole moment.
Previous studies have identified this class of compounds having antitrypanocidal
activity. Based on this result, mesoionic 1,3,4-thiadiazolium-2-aminide
derivatives were studied for trypanothione reductase activity. Among
them, the nitro-containing compound 89 exhibited a noncompetitive
inhibition profile with an IC50 of 1.63 μM. Molecular
docking studies have indicated that these mesoionic compounds effectively
fit into the substrate binding site together with the substrate molecule.
253
Compound 89 was also active on L. amazonensis promastigotes with an EC50 = 1.5
μM.
254
The compound was used in an L. infantum murine model where it exhibited high efficacy
upon intraperitoneal dosing at 20 mg/kg/day for 4 weeks. No parasites
were detected in the liver or the spleen. In an L. amazonensis mouse model, intralesional
topical treatment of 20 mg/kg/day led
to superior therapeutic efficacy than treatment with meglumine antimoniate.
253
It has been shown that the enzymes in
the trypanothione pathway:
trypanothione synthetase (TS), and trypanothione reductase (TR) and
tryparedoxin peroxidase (TP) are absent in human hosts and are essential
to parasites. While trypanothione reductase has structural similarity
with its human homologue glutathione reductase, which could potentially
impede the path to design selective analogues, the other two enzymes
TS and TP hold the promise of delivering selective inhibitors against
them.
3.3.4
Cyclophilins
Cyclophilins are groups
of proteins which bind to cyclosporine (90) (Figure 16). Proteins in this family share
approximately
109 amino acids which are referred to as the cyclophilin-like domain.
This domain is responsible for peptidylprolyl isomerase (PPIase) which
influences a number of biological processes such as protein folding,
assembly of multiprotein complexes, and signal transduction. Cyclosporine
(90) is known to have antileishmanial activity on intracellular L. tropica- and L.
major-infected mouse
macrophages. However, the repurposing of cyclosporine (90) is not feasible because
of its immunosuppressive effect. Späth
and co-workers have proven that cyclosporine acts on Leishmania cyclophilins and the
structural differences between human and parasite
orthologs, potentially enable the design of compounds to selectively
act against the parasite.
255
3.3.5
Purine Salvage Pathway
Leishmania species
have to utilize purine from the mammalian
host to synthesize purine nucleotides. While the protozoan transporters
are different from their mammalian counterparts in terms of substrate
specificity, there are numerous uptake mechanisms which make targeting
of these transporters difficult as the nontargeted transporters provide
escape mechanism.
256
The most important
enzyme in this pathway is phosphoribosyl transferase (PRT). There
are three known homologues of PRT namely, adenine phosphoribosyl transferase,
hypoxanthine-guanine phosphoribosyl transferase (HGPRT), and xanthine
phosphoribosyl transferase (XPRT).
206b,257
HGPRT converts
hypoxanthine to inosine monophosphate and guanine to guanine monophosphate.
One of the known inhibitor of HGPRT is allopurinol (91) (Figure 16), which is phosphorylated
by
HGPRT and incorporated into nucleic acids leading to death of the
parasite. Allopurinol (91) has been shown to be efficacious
against both cutaneous and visceral leishmaniasis.
258
Moreover, it was found to be synergistic with other antileishmanial
drugs.
113a,259
However, it was found that PRTs are not
essential for parasitic survival raising doubts about the validity
of this target.
260
Nevertheless given the
orthogonal mechanism, a pan-purine transport inhibitor might be able
to provide the necessary parasite growth inhibition. This approach
has not been reported in the literature.
Figure 17
Representative examples
of topoisomerase inhibitors.
Table 9
L. infantum Activity
on Topoisomerase Inhibitors
L. infantum EC50 (μM)
compound
promastigote
intracellular
amastigote
splenocyte
culture EC50 (μM)
SI
92
1.12
0.03
0.62
20.7
93
10.86
0.16
4.96
31
94
1.73
0.001
0.21
175
95
>200
>100
>200
ND
96
12.20
0.05
0.54
9.8
6
25.15
8.7
504.1
57.9
Table 10
Topoisomerase
and Antiparasitic Activity
on Fatty Acid Derivatives
compound
Leishmania EC50 (μM)
LdTopIB IC50 (μM)
hTopIB IC50 (μM)
macrophage
CC50 (μM)
2-HDA (97)
17.8a
28.7
>100
>100
2-ODA (98)
11.0a
5.3
51.9
>100
99
260b
31
>100
>100
100
240b
22
>100
90
101
19.8a
activity at 50 μM
102
165a
62
604
a
L. donovani promastigote
assay.
b
L. infantum amastigote
assay.
Table 11
Topoisomerase
and Antiparasitic Activity
on Thiadiazole Derivatives
compound
R
L.
major Top I (%)
L.
major Top II (%)
intra am
EC50 (μM)
112
Ph
73
59
4.2
5-Cl-2-thiophene
62
57
2.7
113
Ph
64
76
3.7
2-Cl-Ph
39
55
8
3-Cl-Ph
49
51
6.8
5-Cl-2-thiophene
37
83
2.8
5-Br-2-thiophene
8
58
6.2
3.3.6
Topoisomerase
DNA topoisomerases
are enzymes that play an important role in numerous biological processes
such as DNA replication, transcription, recombination, and repair.
While topoisomerases are ubiquitous in all organisms, studies have
shown that kinetoplastid topoisomerases have some distinguishing features
that differentiate the parasite enzyme from its prokaryotic and eukaryotic
counterparts.
261
Broadly, they are classified
as type I and type II topoisomerases and cleave single stranded and
double stranded DNA, respectively. Both type I and type II topoisomerase
have been characterized from L. donovani. The type
I topoisomerase enzyme was found to be independent of ATP and is present
in both the kinetoplast and nucleus. In contrast, type II topoisomerase
was found to exhibit both ATP dependent and independent activity.
DNA topoisomerase inhibitors have been extensively covered in the
literature.
261a,261b,262
Based on the success of camptothecin (92) (Figure 17), a known topoisomerase inhibitor
in the field
of oncology, camptothecin analogues used in therapy were evaluated
for antileishmanial activity. Three compounds, namely topotecan (Hycantim, 93), gimatecan
(ST1481, 94), and the pro-drug
irinotecan (Camptosar, 95) as well as its active metabolite
SN-38 (96) were evaluated against L. infantum. Gimatecan (94) and camptothecin (92)
were
most potent on L. infantum promastigotes with activity
in the micromolar range (Table 9). Moreover,
all these compounds except for irinotecan (95) inhibited L. infantum splenocyte-infecting
amastigotes in the nanomolar
potency range. The inhibitory potency of campothecin derivatives on
recombinant L. infantum topoisomerase IB demonstrated
that all the compounds affected topoisomerase activity, with gimatecan
(94) being the most potent compound preventing the relaxation
of supercoiled DNA at submicromolar concentration.
263
2-Alkynoic fatty acids have been described to have
broad range
of biological activity including antileishmanial, antimycobacterial,
antifungal, and anticancer properties. In particular, 2-hexadecynoic
acid (2-HDA, 97) and 2-octadecynoic acid (2-ODA, 98) (Figure 17) demonstrated activity
against L. donovani (Table 10). These fatty acids are inhibitors of the L. donovani
DNA topoisomerase IB enzyme (LdTopIB) and the potency against LdTopIB
is dependent on chain length.
264
Also (5Z,9Z)-(±)-2-methoxy-5,9-eicosadienoic
acid (99) and its acetylenic analog (±)-2-methoxy-5,9-eicosadiynoic
acid (100) were shown to be active against the L. donovani DNA topoisomerase IB enzyme
(LdTopIB). The potency
for LdTopIB inhibition correlated with the degree of unsaturation.
Unsaturated fatty acids 101 and 102 were
isolated from marine sponge Polymastia penicillus and Dragmaxia
undata respectively and displayed antiprotozoal activity
against L. donovani through inhibition of Leishmania DNA topoisomerase IB enzyme (LdTopIB)
as well.
All the reported compounds appear to have selectivity over human topoisomerase
IB enzyme (hTopIB).
264a
These findings
supported the previous hypothesis that monounsaturated iso-methyl-branched
fatty acids impart selectivity over human DNA topoisomerase I.
265
Two lignan glycosides namely, lyoniside
(103) and
saracoside (104) (Figure 17) were
evaluated for activity against L. donovani promastigotes
as well as intracellular amastigotes. Both compounds inhibited promastigotes
in a sodium antimony gluconate sensitive AG83 strain as well as an
antimony resistant GE1 strain in the 2–4 μM range. Moreover,
both compounds were more potent on intracellular amastigotes with
submicromolar activity against sensitive and resistant strains. These
noncompetitive topoisomerase inhibitors stabilize the DNA-LdTopIB
cleavage complexes inside Leishmania cells and induce
apoptosis. Both lyoniside (103) and saracoside (104) demonstrated impressive antileishmanial
efficacies in
a BALB/c mice model of leishmaniasis when dosed intraperitoneally
at 2.5 and 5 mg/kg with almost complete clearance of the liver and
splenic parasite burden at the higher dose.
266
16α-Hydroxycleroda-3,13(14)Z-dien-15,16-olide (105) (Figure 17) was isolated from
Polyalthia
longifolia and showed in vitro activity on intracellular
transgenic GFP tagged expressed L. donovani amastigotes
of 5.8 μg/mL which was equipotent to miltefosine (5.0 μg/mL).
The in vivo efficacy was assessed using a dosing regimen of 25, 50,
100, and 250 mg/kg for 5 days against established L. donovani infection in hamsters.
Dose dependent efficacy was observed, and
at 250 mg/kg, a 91% reduction of parasite burden was observed in spleen,
87.5% in liver, and 89.1% in bone marrow. No overt signs of toxicity
were observed in animals after 6 months of treatment. The topoisomerase
activity was established when the compound was added together with
DNA and enzyme leading to an observed inhibition of relaxation activity
at various concentrations.
267
A series
of triterpene analogues were synthesized from betulin
(106, R = H) and dihydrobetulin (107, R
= H) (Figure 17), isolated from the cork layer
of Betula spp. Three analogs (disuccinyl betulin 106,
R = succinate; diglutaryl dihydrobetulin 107, R = glutarate;
disuccinyl dihydrobetulin 107, R = succinate) inhibited
relaxation activity of the enzyme type IB topoisomerase (IC50 = 12–23 μM) and were
also able to reduce the intracellular
parasite burden in macrophages infected with wild-type L.
donovani and with sodium antimony gluconate resistant parasite
(GE1) parasites with EC50 values in the range of 6–10
μM. Further mechanistic work indicated that these compounds
interact with the enzyme in a reversible manner. The stoichiometry
of these compounds binding to LdTOP1LS is 1:1 (mol/mol) with a dissociation
constant on the order of ∼10–6 M. In contrast
to campothecin (92), these compounds do not stabilize
the cleavage complex; rather, they destroy the covalent complex formation.
These results suggest that betulin derivatives could be exploited
for antimony resistant leishmaniasis.
268
Two known topoisomerase indenenoisoquinoline alkaloids, namely
AM13-55 (108) and indotecan (109) (Figure 17), were investigated for antileishmanial
activity.
Both these compounds were found to be potent in L. infantum cultured in splenocytes
with an EC50 of 100 nM and with
SI index >48 over uninfected splenocytes. The efficacy for these
compounds
was evaluated in a murine BALB/c model of infected splenocytes with L. infantum. Mice
were treated intraperitoneally with 0.5
mL solutions of indotecan (109) or AM13-55 (108) in DMSO-saline at a dose of 2.5 mg/kg
every 2 days for 15 days.
Mice treated with indotecan (109) exhibited drastic reduction
in parasite load both in the liver and the spleen. Surprisingly, the
same dose of AM-1355 (108) led to a greater than 90%
reduction in parasites only in spleen and with no change in parasite
burden in the liver. Lack of reduction of parasites in the liver could
be attributed to metabolism of the parent compound to inactive metabolite(s).
The inhibitory potency of both alkaloids on L. infantum recombinant TopIB was assessed
with results showing that indotecan
(109) was the most potent compound on topoisomerase IB.
269
A series of bislawsone analogues were
assessed for their activity
on L. donovani promastigotes as well as on leishmanial
DNA topoisomerase I. The best analogs (110 and 111) (Figure 17) showed a promastigote
activity of 2 μM indicating that these compounds are active
at the cellular level. In the topoisomerase I enzymatic assay; the
range of activity varied from 51 to 70 μM in a simultaneous
assay and 15–16 μM in a preincubation assay indicating
that topoisomerase I is one of the targets for these compounds. Given
the weak activity, however, additional targets cannot be ruled out.
200
A series of nitroheteroaryl-1,3,4-thiadiazoles
were investigated.
The results showed that the nitroimidazole and nitrofuran analogs
are active against intracellular amastigotes in the single digit micromolar
range with low toxicity against the host cells. An assay against Leishmania topoisomerases
proved that compounds from series 112 and 113 (Figure 17) acted against both topoisomerase
I and II with inhibition in the
range of 8–83% at EC50 doses of compounds against Leishmania (Table 11). These series
of compounds were also found to be active against both L.
infantum and L. tropica.
270
In an interesting study involving known topoisomerase
I inhibitor
3,3′-diindolyl methane (DIM, 114) (Figure 17), resistant parasite strains of L. donovani
were generated by gradually increasing the concentration of the
drug leading to random mutations in the large and small subunits of
heterodimeric DNA topoisomerase I (LdTOP1LS). It was discovered that
the mutation of the large subunit of LdTOP1LS at F270L is responsible
for resistance to DIM. A series of DIM analogues was generated (115-117) which were
not only active on resistant L. donovani parasites but were also active against the
wild
type parasite.
256
Figure 18
Examples of protease
and phosphodiesterase inhibitors.
3.3.7
Proteases
There are a total of
154 proteases in the Leishmania genome. These proteases
are in the cysteine, serine, aspartate, and metalloprotease family.
Out of these proteases, cysteine proteases and metalloprotease have
proven to be important in the pathogenesis of leishmaniasis.
271
3.3.8
Cysteine Protease
The cysteine
proteases in Leishmania exist in the gene families
CPA, CPB, and CPC. It has been established that at least two of the
families need to be targeted to absolutely block the parasite invasion
and replication in host cells.
272
In an
effort to find new starting points for cysteine protease inhibitors, L. mexicana cysteine
protease CPB2.8, which shows significant
differences with bovine cathepsin B, was selected as a target. High
throughput screening of a compound library against this enzyme and
bovine cathepsin B (BtCatB) identified four novel inhibitor classes
broadly classified into 3 groups depending on the warhead-types, namely
thiosemicarbazones (118, 119), nitriles (120), and semicarbazones
(121) (Figure 18). The thiosemicarbazone
118 showed an IC50 on CPB2.8ΔCTE (which is the recombinant
form of the amastigote specific isoform CPB2.8 expressed without the
C-terminal extension) in the nanomolar range with complete selectivity
over bovine Cat B (IC50 >30 μM). In contrast,
the
thiosemicarbazone (119) was equipotent on both CPB2.8ΔCTE and
on BtCatB in the nanomolar range. The nitrile 120 was approximately
ten times less potent on CPB2.8ΔCTE (K
i = 570 nM) and had some degree of selectivity over bovine
protease BtCatB (IC50 = 13.8 μM). The most promising
hit was 121 with a K
i of
5 nM and an IC50 >30 μM for BtCatB. These chemotypes
prove that reasonable starting points can be discovered for further
optimization of cysteine protease inhibitors.
273
In a separate effort by Augustyns and co-workers, a set
of α-ketoheterocycles was designed and synthesized as cysteine
protease inhibitors of L. mexicana. However, there
was no correlation between the enzymatic activity and cellular activity,
thus bringing into question the validity of the target.
274
A series of semisynthetic morelloflavone
(122) (Figure 18) analogs were
evaluated. All compounds exhibited inhibition of L. amazonensis promastigotes as well
as amastigote activity in nanomolar range
with low cytotoxicity. In addition, compounds 123–125 were active against recombinant-CPB2.8
of L. mexicana and r-CPB3 of L amazonensis with IC50 values of 0.7–1.5 μM, respectively.
These results provide new starting points for lead optimization.
275
Tellurium compounds as chemotherapeutic
agents are being investigated
for variety of indications. Organic telluranes are also known to be
inhibitors of cysteine proteases.
276
Based
on the earlier reports of organotellurane compounds being active on
promastigote and amastigote forms of L. amazonensis,
277
tellurium compound RF07 (126) (Figure 18) was evaluated against L. chagasi, a causative
agent of visceral leishmaniasis
in Latin America. In vitro assays indicated that the compound was
active on intracellular amastigotes with an EC50 of 530
nM and a 10-fold cytotoxic window when compared to noninfected macrophages.
Intraperitoneal injection of RF07 (126) in L.
chagasi-infected hamsters exhibited a 99.6% reduction of
parasite burden when compared to control animals which received an
antimonial drug Glucantime or PBS. The effect of RF07 (126) on cathepsin B activity
on L. chagasi amastigotes
was evaluated spectrofluorometrically using fluorogenic substrates
and the IC50 values were 10-fold higher suggesting the
potential involvement of other targets in cells and in vivo.
278
The palladacycle’s trypanocidal activity
as well as their ability to affect cathepsin B activity has been previously
demonstrated.
279
Inspired by this, palladacycle
compound DPPE 1.2 (127) was evaluated for activity against L. amazonensis, which is
prevalent in in the Amazon region
of Brazil and is responsible for cutaneous leishmaniasis. The compound
was found to be active against axenic L. amazonensis promastigotes with an EC50 of
2.13 nM. It was also found
to be active on intracellular parasites with an EC50 of
128 nM, and the compound was 10-fold less toxic in macrophages (CC50 = 1,267 nM).
In an efficacy study, L. amazonensis-infected BALB/c mice were injected subcutaneously
with DPPE 1.2
(127) at 4.8 mg/kg every other day. The treated animals
showed a significant decrease in foot lesion size and a 97% reduction
of parasite burden when compared to controls that were treated with
PBS. DPPE 1.2 (127) inhibited the cysteine protease activity
of L. amazonensis amastigotes and more significantly
the cathepsin B activity which was determined by zymography after
electrophoresis.
280
3.3.9
Aspartic Protease
The role of aspartic
proteases in Leishmania was discovered when HIV aspartyl
peptidase inhibitors were profiled for L. amazonensis proliferation. The HIV protease
inhibitors affected parasite growth
in a dose-dependent fashion with nelfinavir (16) (Figure 2) and lopinavir (128) (Figure
18) exhibiting an EC50 of 15.1 μM
and 16.5 μM on promastigotes. The protease activity of these
compounds was established by measuring proteolytic hydrolysis of the
peptide substrate in a dose dependent fashion in L. amazonensis. Lopinavir (128) was
able to reduce the proteolytic
hydrolysis of the substrate by approximately 90% at 1 μM, and
demonstrated full activity at 10 μM. On the other hand, nelfinavir
(16) exhibited weak activity with inhibition of 98% at
10 μM and no observable activity at 1 μM.
281
In a separate effort, an ortholog of
the yeast Ddi1 protein was identified as the only member of the aspartic
protease family in Leishmania parasites and was explored
as a potential drug target. An enzymatic assay was developed by incorporating
genes encoding Ddi1 orthologs from L. major and humans.
Nelfinavir (16) was active on human as well as L. major with an IC50 value of 3.4
and 0.44 μM,
respectively. These values correlate well with observed cellular activity.
282
3.3.10
Serine Protease and
Metalloprotease
In the serine protease family, oligopeptidase
and oligopeptidase
B play an important role in the interaction of pathogens with their
host and are considered to be important targets. A number of medicinal
chemistry efforts have been undertaken in the past which have been
described previously.
271a
Leishmania metalloprotease GP63 is located on the surface of promastigotes
and is thought to be a key player in evasion and survival from lysis
prior to internalization by macrophages. However, there are no medicinal
chemistry efforts reported for this target.
271a
Table 12
Antileishmanial Activity of Phosphodiesterase
Inhibitors
compound
L.
major pro EC50 (μM)
L.
infantum am EC50 (μM)
129
45
130
58
131
44
10.2
132
1000
3.3.11
Phosphodiesterase
Phosphodiesterases
(PDEs) control the cellular concentration of the second messenger’s
cAMP and cGMP that are key regulators of many important biological
processes.
283
The human genome contains
twenty-one PDE genes that are categorized into 11 families. In comparison,
the genome of the protozoal parasite L. major contains
five PDE genes encoding LmjPDEA, LmjPDEB1, LmjPDEB2, LmjPDEC, and
LmjPDED. Two of these, LmjPDEB1 and LmjPDEB2, are adjacently situated
on chromosome 15 and share extensive similarity in their overall architecture.
284
Early studies showed that three human PDE inhibitors
(dipyridamole (129), etazolate (130), and
trequinsin (131)) (Figure 18)
inhibit the proliferation of L. major promastigotes
and L. infantum amastigotes with EC50 values
in the micromolar range (Table 12).
284
Recently, the cocrystallization of the catalytic
domain of LmjPDEB1 in complex with 3-isobutyl-1-methylxanthine (IBMX, 132) was reported.
IBMX (132) is a nonspecific
PDE inhibitor with an enzymatic activity of 580 nM against that catalytic
domain of LmjPDEB1. A comparison between the structures of LmjPDEB1
and human PDEs has identified a novel pocket in the LmjPDEB1 structure,
which may thus be useful for the design of parasite selective inhibitors
for the treatment of leishmaniasis.
285
Figure 19
Examples
of tubulin inhibitors.
3.3.12
Tubulin
Tubulin, which is highly
conserved across all species, is a superfamily of globular proteins
with six distinct families, the alpha-, beta-, gamma-, delta-, epsilon-,
and a sixth family zeta-tubulin, which is specific to kinetoplastid
protozoa. Tubulins have been associated with a variety of cellular
functions such as maintenance of cell shape among others. Tubulin
has proven to be an attractive target in the field of oncology and
there are several successful drugs in the clinic.
286
The comparison of tubulin sequences from mammalian cells
and yeast cells reveals a homology of 70–90%. However, specific
antitubulins are known and it is suggested that differences in amino
acid sequence lead to different conformations of tubulins making the
targeting of parasitic tubulin possible.
287
Interest in antitubulins for antiparasitic therapy was piqued
when Chan and co-workers demonstrated that radioactive herbicide trifluralin
(133) (Figure 19) binds selectively
to tubulin extracts from Leishmania species.
288
Based on this finding, another dinitro compound
(134) was found to selectively bind to L. tarentolae tubulin (IC50 = 7.4 μM). Furthermore,
this compound
was found to have activity against L. donovani axenic
amastigotes (EC50 = 2.3 μM) with no cytotoxicity
on Vero cells. Given the liabilities of the nitro group, the compound
was further optimized to 135 which showed an IC50 of 6.6 μM against L. tarentolae
tubulin and
cellular activity against L. donovani axenic amastigotes
with an EC50 of 4.4 μM.
289
In addition, a screen was carried out on 10 000 compounds
using L. tarentolae tubulin which led to the identification
of new chemotypes for future optimization campaigns. Inspired by the
success of sulfonamides, a benzopyrazole sulfonamide (136) was designed and synthesized.
287a
Compound 136 had an EC50 of 37–48 μM against
promastigotes of different Leishmania subspecies.
This cellular activity was in the same range as miltefosine (EC50 = 17 μM). Furthermore,
compound 136 when
dosed via i.p. route was able to reduce the parasite load in the liver
and spleen by 96–97% in an acute L. infantum mouse model.
290
Rodrigues and co-workers
have designed and synthesized a hybrid of dintroaniline and alkyl
phosphocholine to attempt to combine the tubulin binding mechanism
with that of miltefosine. Compound 137 has an EC50 of 2.6 and 1.2 μM against L. amazonensis
promastigotes and intracellular amastigotes, respectively. Fluorescence
microscopy with alpha tubulin antibody in conjunction with scanning
electron microscopy show changes in the cytoskeleton and alterations
in the shape of the plasma membrane proving that the hybrid molecule
is still acting on tubulin.
291
Stilbene
based compounds are widely found in nature and are known
for their pharmacological properties.
292
There are previous reports where stilbenes have been reported for
their antileishmanial activity.
293
A series
of stilbene derivatives were also evaluated for their antileishmanial
activity. Based on the SAR, it was observed that trans-stilbenes were more potent
than cis isomers. trans-3,4′,5-Trimethoxy-3′-amino-stilbene (TTAS, 138) was the most
active stilbene, showing a LD50 value of
2.6 μg/mL in L. infantum. It was observed that
TTAS (138) had low toxicity when tested on normal hemopoietic
cells. TTAS has the ability to block Leishmania parasites
in G(2)-M phase of cell cycle which is in line with the affinity chromatography
results that identified tubulin as the putative target.
294
4
Introduction
to Human African Trypanosomiasis
(HAT) and Clinical Description
Also known as African sleeping
sickness, HAT is caused by the protozoan
parasite, Trypanosoma brucei. Two forms of the disease
exist in humans, the more common caused by the subspecies Trypanosoma brucei gambiense,
and the less common form caused
by Trypanosoma brucei rhodesiense. Both forms are
transmitted to humans by the painful bite of blood-feeding tsetse
flies. Infectious metacyclic trypomastigotes present in the salivary
fluid of flies establish a primary lesion in the skin known as a trypanosomal
chancre that appears 5–15 days after the initial bite. The
parasites proliferate and spread to the blood where they disseminate
throughout the body. During the early “hemolymphatic stage,”
patients experience nonspecific symptoms of intermittent fevers, malaise,
arthralgias, and headaches. The acute disease has protean manifestations
including gastrointestinal complaints, cardiac features, ophthalmological
complications, endocrine dysfunction, to name a few. In the form of
HAT caused by T. brucei gambiense, the early stage
evolves over a time frame of months or even years.
295
In one of the early clinical descriptions of HAT, Thomas
Winterbottom in 1803 referred to the swollen lymph nodes along the
posterior neck as an important characteristic and mentioned that this
finding, now known as Winterbottom’s sign, was used by Arab
slave traders to exclude potential slaves.
296
In the other form of HAT caused by T. brucei rhodesiense, the early stage runs a more
rapid course of weeks before evolving
into late-stage disease. As a zoonotic infection, the rhodesiense form of HAT may
be less well adapted to the human host compared
to the anthroponotic gambiense form. In both forms
of HAT, late-stage disease is defined by the entry of trypanosomes
into the central nervous system. A patient is judged to have late-stage
HAT when trypanosomes (or elevated white blood counts) are detected
in cerebral spinal fluid upon doing a spinal tap. In late-stage disease,
parasites are also present within parenchymal brain tissue giving
rise to the encephalitic picture for which the disease is so feared.
Symptoms include psychiatric, motor, and sensory disturbances along
with abnormal reflexes. Approximately three-quarters of patients have
profound sleep disturbance, including nocturnal insomnia and daytime
somnolence,
297
giving rise to the disease
name, sleeping sickness. Without treatment, patients inevitably progress
to coma and death.
5
Background of HAT
5.1
History and Epidemiology of HAT
Other
species of trypanosomes such as T. congolense, T.vivax, and T. brucei brucei infect
animals and have greatly
limited man’s ability to bring domesticated animals into many
regions of Africa. The disease affecting cattle, nagana, has been
recognized since antiquity. Interestingly, humans are resistant to
these species due to trypanosome lytic factors circulating in their
blood,
298
which points to the long evolution
of humans in the presence of these parasites in Africa. It is thought
that HAT is a relatively recent event in human development.
296
In fact, the infectivity of T. brucei
rhodesiense to humans is due to a serum-resistance associated
gene that arose as a single event and spread through East Africa by
genetic exchange.
296,299
Tsetse flies were recognized
to cause nagana 50 years before the Scottish microbiologist, David
Bruce, first reported Trypanosoma brucei in the blood
of cattle in 1895.
296
The first microscopic
detection of trypanosomes in human blood was made on a steamboat captain
in The Gambia in 1901 by British surgeon R. M. Forde.
296
This was named, Trypanosoma gambiense. The second trypanosome species causing infection
in humans, T. rhodesiense, was identified in 1910.
Transmission
of HAT is limited to the range of tsetse flies, thus
the disease is confined to the African continent. In the 20th century,
three major sleeping sickness epidemics have afflicted the Africa.
The first epidemic at the turn of the 20th century, killed about 300 000–500 000
people in the Congo basin, Uganda, and Kenya and led to the introduction
of arsenical compounds as the first treatments for HAT. Subsequent
work by the German chemical/pharmaceutical company, Bayer, led to
the discovery of suramin in 1916, the first truly effective treatment
for HAT, and one that is still in use. The second major epidemic occurred
between about 1920 and 1940. In response to these epidemics, control
measures were introduced including tsetse fly control using traps
and brush clearing, host reservoir control, and game destruction.
296
Colonial powers introduced mobile teams to
carry out these control measures with positive impacts on prevalence
of HAT. The third major HAT epidemic occurred following the departure
of colonial powers (1960–70s) with the associated political
instability and interruption of control programs (exacerbated by the
banning DDT in the 1970s). The most heavily impacted countries were
Angola, Congo, Sudan, and Uganda with more than 300 000 cases
per year occurring in the late 1990s. The WHO along with partner agencies
and governments stepped in with aggressive case detection, treatment,
and vector control to bring rates down to 50 000–70 000
by 2006. Reported cases dropped below 10 000 for the first
time in 2009, although the factor gap between reported cases and actual
cases is probably at least three.
300
Areas
with political and social instability, particularly in the Democratic
Republic of the Congo and the Central African Republic continue to
see high rates of HAT that help sustain the risk of future epidemics
to the continent.
301
Thirty-six countries
are currently listed as endemic for HAT.
300
5.2
Biology of HAT
African trypanosomes
have fascinated biologists since their discovery. The complex life-cycle
of T. brucei between the vertebrate and invertebrate
hosts provides reservoirs and means of transmission to ensure efficient
propagation in nature. Parasites undergo dramatic morphological and
biochemical adaptions when cycling between these vastly different
hosts. In humans, during the early stage, the trypanosomes spend most
of their time in the nutrient-rich environment of the bloodstream
where normal glucose levels run about 100 mg/dL. For ATP production,
bloodstream trypanosomes are entirely dependent on the conversion
of the blood sugar glucose. Oxidative metabolism involving mitochondrial
Krebs cycle enzymes and oxidative phosphorylation are essentially
shut down.
302
On top of this, the glycolytic
pathway in trypanosomatids is organized in a unique manner: the majority
of the glycolytic enzymes are sequestered inside peroxisome-like organelles
known as glycosomes, presumably concentrating the enzymes and their
substrates for efficiency. While living in the bloodstream, trypanosomes
are continually under attack by the body’s immune system, particularly
antibodies directed at surface antigens. As a countermeasure, as much
as 10% of T. brucei’s genome encodes variant
surface glycoproteins (VSGs) that coat the outer membrane by attachment
to glycosylphosphatidylinositol anchors. Only one VSG is expressed
at a time with stochastic switching to provide antigenic variation
that allows for evasion of the immune system. Due to myriad VSGs,
attempts at making effective vaccines for HAT have been unsuccessful.
The T. brucei genome of ∼9000 genes has been
fully sequenced and has accelerated our understanding of the biology
of this sophisticated parasite. Areas of unique biology point to attractive
targets for drug discovery, such as the machinery involved in extraordinary
process of RNA editing that takes place in the sole mitochondrion
known as the kinetoplast.
303
Further discussion
of target-based drug discovery follows later.
6
Drug Discovery for HAT
6.1
Current Treatments
The drugs currently
recommended for treating HAT are listed in Table 13 and Figure 20. Approximately 98%
of
cases of HAT are due to T. brucei gambiense which
predominates in central and western African countries.
304
For early stage gambiense HAT,
pentamidine (3) is considered first line treatment. This
diamidine drug was developed in the 1930s by English chemist A. J.
Ewins of the pharmaceutical company May and Baker.
296
It is administered by intramuscular injections once daily
for 7 days, although it can also be given intravenously. The drug
is usually effective and relatively inexpensive, but it is associated
with pain at the injection site, hypo- or hyperglycemia, prolonged
QT interval on electrocardiogram, leukopenia, nephrotoxicity, hypotension,
and gastrointestinal symptoms. Binding to tissue proteins contributes
to a large volume of distribution and long terminal half-life. It
does not cross the blood-brain barrier, hence its use is limited to
patients with early stage HAT. The drug is thought to have a fairly
nonspecific mechanism of killing trypanosomes by binding DNA and disrupting
mitochondrial functions. It is able to mediate selective toxicity
on trypanosomes over mammalian cells by virtue of being concentrated
to millimolar levels inside trypanosomes by P2 and other surface transporters.
305
Resistance to pentamidine has been generated
in laboratory strains but is not reported to be a widespread problem
in the field.
306
Table 13
Drugs
for Treating Human African
Trypanosomiasis
Disease
Stage
Drug
Year introduced
Route of
administration
Liabilities
Gambiense HAT
Early
Pentamidine
1941
IM or IV
No oral
formulation
Eflornithine
1981
IV
Expensive, every 6 h dosing
Melarsoprol
1949
IV
Arsenical (toxic encephalopathy)
Late
NECTa
2009
IV + PO
Expensive, IV for eflornithine
part
Rhodesiense
HAT
Early
Suramin
1922
IV
No oral formulation
Late
Melarsoprol
1949
IV
Arsenical (toxic encephalopathy)
a
NECT: nifurtimox/eflornithine combination
therapy.
Suramin (139) is perhaps the oldest antimicrobial
drug in continuous use since its introduction (i.e., 1922). It is
the first-line treatment for rhodesiense HAT and
given by slow intravenous infusion every 3–7 days for a 4-week
period, typically.
307
It is highly protein
bound and has very long terminal half-life of 41–78 days; it
does not cross the blood-brain barrier. It is effective therapy, but
is associated with urticarial rash in about 90% of patients that usually
resolves without discontinuation of the drug. Other common side effects
include pyrexia, nausea, and reversible nephrotoxicity. The mechanism
of action for suramin on trypanosomes is unknown. Resistance in the
field has been rarely reported.
307
Melarsoprol (140) is an arsenical drug used for late-stage
HAT. As discussed above, arsenicals were the first drugs introduced
for treating sleeping sickness starting with a drug called atoxyl,
an ironic name since clinical studies showed it caused blindness due
to optic nerve atrophy.
296
Melarsoprol
was the first and still the only effective drug for late-stage HAT
due to T. brucei rhodesiense. It has largely been
replaced by eflornithine-based treatment for management of late stage
HAT due to T. brucei gambiense. However, due to challenges
with distributing and administering eflornithine, melarsoprol was
still being used to treat 88% of persons with second stage T. brucei gambiense as
recently as 2003.
308
Melarsoprol is perhaps one of the most dangerous drugs
used for treating an infectious disease with reactive encephalopathy
occurring in ∼10% of patients and fatalities occurring in ∼5%
of these cases. However, since late-stage HAT is uniformly fatal,
medical providers have been forced for decades to accept melarsoprol
as the best therapeutic option. On top of this, melarsoprol is associated
with agranulocytosis, skin rashes, peripheral neuropathy, cardiac
arrhythmias, and multifocal inflammatory disorder.
308
Melarsoprol is administered by intravenous injection in
a 10 day regimen.
309
Like pentamidine,
it is concentrated in trypanosome cells via uptake by P2 transporters;
it then disrupts the redox environment within the cell by disrupting
the protein, trypanothione.
310
Treatment
failures occur with increasing frequency in many regions although
the direct responsibility of drug-resistant parasites has not been
firmly established.
307
Eflornithine
(141), introduced in 1981, was an important
breakthrough for HAT as it provided a safer alternative to melarsoprol
for late-stage disease caused by T. brucei gambiense. Eflornithine (difloromethylornithine,
DFMO) was repurposed from
investigations as an anticancer agent. It blocks the enzyme, ornithine
decarboxylase (ODC), which is integral to polyamine biosynthesis.
It acts on the mammalian enzyme as well as the trypanosomal ODC, but
owing to the rapid turnover of the mammalian ODC, the drug exerts
much less toxicity on host cells compared to bloodstream trypanosomes.
It is less effective on T. brucei rhodesiense so
its use is restricted to cases of late stage gambiense HAT. Eflornithine by itself
is given at a dose of 100 mg/kg intravenously
every 6 h for 14 days. For a typical-sized individual, this demanding
regime translates to nearly a half-kilogram of drug administered while
the patient is confined to a hospital. Through support from WHO, eflornithine
kits for two weighing 40 kg and costing US$1420 were made available
for distribution in disease endemic countries.
300
The frequent administration schedule of eflornithine is
necessary due to its short plasma half-life of 3 h. It is associated
with side effects of fever, headache, alopecia, hypertension, rash,
peripheral neuropathy, tremor, and diarrhea.
307
Resistance, due to mutations in a putative amino acid transporter,
has been shown in vitro.
311
An important
recent advancement in HAT chemotherapy was the introduction
of nifurtimox eflornithine combination therapy (NECT), which is currently
the first line of treatment for HAT.
312
Nifurtimox (142) was repurposed as a drug for treating
American trypanosomiasis (Chagas disease) caused by Trypanosoma
cruzi. For HAT, nifurtimox is orally administered three times
a day for 10 days in combination with intravenous eflornithine. The
advantage is that eflornithine is given every 12 h for 7 days at 200
mg/kg rather than every 6 h for 14 days that is used in monotherapy.
Although the burden of intravenous therapy is still a factor, it is
considerably reduced by the longer dosing frequency and shorter total
duration. Compared to eflornithine alone, NECT was associated with
a higher incidence of tremors, anorexia, and nausea.
312a
NECT was added to the WHO Essential Medicines
List in 2009. Kits for four full treatment courses weigh 36 kg and
cost US$1440, and are being widely adopted in disease endemic countries.
300
Despite this positive advancement, the need
for intravenous treatment coupled with the high costs of distribution,
makes NECT a far cry from optimal chemotherapy for treating late stage
HAT. A target product profile (TPP) for a better drug for HAT has
been proposed by the Drugs for Neglected Diseases initiative.
141
The ideal drug would be effective against both
early- and late-stage disease, orally administered over a relatively
short course (i.e., 7 days), safe for all persons including children
and pregnant women, and cost less than 30 euros per course. By being
effective in both early and late-stage disease, the drug would obviate
the need to perform lumbar punctures for staging purposes, a major
advantage. Due to the large gap between the profiles of currently
used HAT drugs and the ideal HAT drug, there is much work to be done
in the field of drug discovery. Recent discoveries and advancements
to be discussed below give us optimism that these goals are achievable
in the coming decade.
Figure 20
Established drugs to treat HAT.
6.2
Drug Candidates in Clinical Trials for HAT:
Fexinidazole and Oxaborole SCYX-7158
Fexinidazole (13) was identified in a phenotypic screen of >700 nitroheterocyclic
compounds against T. brucei cultures.
313
It was originally synthesized by Hoechst in
the 1970s and shown to have antitrypanosomal activity.
307
The compound is active against T. b.
rhodesiense and T. b. gambiense and cures
both the acute and chronic mouse models of HAT infection.
314
Fexinidazole is metabolized by P450 enzymes
to sulfoxide and sulfone derivatives that have similar antitrypanosomal
activity as the parent compound (range: 0.4–0.8 μg/mL).
Oral bioavailability in mice was 41%, and the parent compound and
metabolites achieved brain concentrations above IC50 values.
313
Fexinidazole was mutagenic in the Ames test
due to bacterial specific metabolism, but not genotoxic on mammalian
cells. Four week repeat-dose toxicokinetic studies in rats and dogs
demonstrated a no observed adverse event at 200 mg/kg/day in both
species. The drug entered phase I human studies in 2009
315
and progressed to phase II/III safety and efficacy
studies in October 2012 where it is being compared to NECT. The API
is produced by Sanofi. The phase II/III studies are taking place in
the Democratic Republic of the Congo and Central African Republic
under direction by the Drugs for Neglected Diseases Initiative in
collaboration with the Swiss TPH.
SCYX-7158 (143) (Figure 21) is the second compound for HAT
that has recently entered human clinical trials. It was derived from
screening a library of boron-based compounds from Anacor Pharmaceuticals
against T. brucei cultures.
316
A lead-optimization program conducted at Scynexis led to the benzoxaborole
compound, SCYX-7158, with an IC50 of 0.29 μg/mL against T. brucei 427 strain. It cures
both the acute and chronic
mouse models of HAT infection.
317
Oral
bioavailability in mice was 55%; it is CNS permeable and highly metabolically
stable in rodents. SCYX-7158 was negative in Ames and hERG channel
assays. It was well tolerated in mice at doses up to 100 mg/kg twice
per day.
317
DNDi is directing the first-in
human studies in France which started in March, 2012, to assess the
safety, tolerability, and pharmacokinetics in healthy volunteers of
sub-Saharan origin.
Figure 21
Structure of SCYX-7158.
6.3
Amidines and Diamidines
Tidwell and
co-workers have extensively developed bisamidines patterned after
pentamidine (3) for treatment of HAT. One compound entered
into clinical trials but the trial was halted due to the occurrence
of nephrotoxicity. These compounds have been reviewed previously.
305
It has been previously reported that these
dicationic compounds are selectively cytotoxic to T. brucei over mammalian cells due
to the differences in the active transport
mechanism, which aids in the accumulation of drug into parasites at
levels ∼1000-fold higher than in mammalian cells.
305
More recently, Alp et al. reported a
series of amidinobisbenzimidazoles including compound 144 (Figure 22).
318
The best compound in the series (compound 144) blocked
the growth of T. b. rhodesiense in vitro with an
IC50 of 0.036 μg/mL and displayed cytotoxicity on
mammalian cells at 29.4 μg/mL. No pharmacokinetic or efficacy
studies were reported.
Dicationic flexible triaryl guanidines
and imidamides were evaluated
as antiprotozoal agents by Arafa et al.
319
The most potent compound in the series 145 had an in
vitro IC50 of 151 nM against T. b. rhodesiense with cytotoxicity of 11.6 μM. Although
molecular modeling
and DNA binding studies were reported, the detailed mode of action
and animal data were not available.
Huang et al. reported the
SAR of alkanediamide linked bisbenzamidines
as antitrypanosomal agents.
320
Compound 146 (Figure 22) in this series had
an IC50 of 0.003 μM against T. b. brucei and an IC50 of 0.002 μM against T. b. rhodesiense.
Compound 146 was found to be less cytotoxic to the
A549 human lung carcinoma cell line with cytotoxicity of 1193 μM.
Although the mechanism of action of bisbenzamidines is credited due
to the binding to DNA, the antitrypanosomal activity of the bisbenzamidines
reported did not directly correlate with the corresponding binding
affinity to DNA. No animal data were provided.
Dicationic substituted
bis(phenoxymethyl)arene analogues of pentamidine
were evaluated for antiprotozoal activities by Bakunova et al.
321
The most active compound against T.
brucei rhodesiense was 1,3-bis(4-amidinophenoxymethyl)benzene 147 (Figure 22) with
an IC50 of 2.1 nM. Compound 148, the N-isopropyl
derivative of 147, was identified to be active in the
acute mouse model of HAT following i.p. dosing (4 × 5 mg/kg),
but none of the compounds exhibited significant oral activity.
Patrick et al. reported the SAR on cationic benzyl phenyl ether
derivatives for activities in vitro and in vivo against T.
b. rhodesiense (STIB900).
322
Several
of the dicationic benzyl phenyl ether derivatives displayed good in
vitro and in vivo activity against T. b. rhodesiense. In particular, methamidoxime
derivative 149 achieved
4 out of 4 cures by oral administration (4 × 25 mg/kg) in a murine
model.
The SAR on pentamidine derivatives bearing the benzofuran
residue
was reported by Bakunov et al.
323
The authors
reported that the potency of these compounds against T. b.
rhodesiense depended upon the nature of the cationic motif,
the orientation of the benzofuran residue and the length of the carbon
linker. The most active compound in this series 150 (Figure 22) had an in vitro IC50
of 0.025 μM
against T. b. rhodesiense with cytotoxicity of 8.6
μM against L6 cells. The target of these compounds and in vivo
data were not reported.
Patrick et al. reported the antiprotozoal
activity of dicationic m-terphenyl and 1,3-dipyridylbenzene
derivatives.
324
Herein several diamidine
derivatives displayed
good in vitro activity against T. b. rhodesiense and
proved to be curative in mouse model of early stage HAT. In particular,
compounds 151, 152, and 153 (Figure 22) achieved 4/4 cure rate in mice
infected with T. b. rhodesiense (STIB900) with four
daily 5 mg/kg i.p. doses and also by a single i.p. dose of 10 mg/kg.
Furthermore, prodrugs 154 and 155 attained
a cure rate of 3/4 with four daily oral doses of 25 mg/kg. Mechanism
of action and pharmacokinetic studies were not reported.
Structure
activity and cytotoxicity analysis of pentamidine derivatives
as antiprotozoal agents was reported by Bakunova et al.
321
Herein they have identified several derivatives
of pentamidine with potent in vitro activity and decreased cytotoxicity
to mammalian cells by varying the aliphatic chain lengths, replacing
the oxygen atom in the aliphatic linker with sulfur and sulfone moieties
and through N-substitutions. Compounds 156 and 157 produced good in vivo activity
in an acute
mouse model of trypanosomiasis by attaining a cure rate of 4/4 with
four daily i.p. doses of 5 mg/kg. Mode of action and the pharmacokinetic
studies were not reported.
Nieto et al. reported the synthesis
and evaluation of N-alkoxy analogues of 4,4′-bis(imidazolinylamino)diphenylamine 158
to improve the blood-brain barrier penetration of the
parent compound.
325
Compound 159, the N-hydroxy analogue of 158, displayed
3 times increase in blood-brain barrier permeability compared to lucifer
yellow as determined by in vitro transport assays through the hCMEC/D3
human brain endothelial cell line. While the parent compound 158 showed a 4/4 cure
rate (i.p. dose of 4 × 20 mg/kg)
in the STIB900 mouse model that mimics the stage-I of the disease,
the N-hydroxy derivative 159 was only
moderately active through i.p. administration.
Figure 22
Amidine and diamidine
compounds active against strains of T. brucei.
6.4
Natural
Product Derived Compounds
2-Arylpaullones as antitrypanosomal
agents was reported by Ryczak
et al.
326
The initial set of 2-arylpaullones
tested possessed good activity against T. b. rhodesiense bloodstream parasites, but
they were also cytotoxic against human
THP-1 macrophages. Further SAR studies on the 2-arylpaullones led
to compounds with good potency against T. b. rhodesiense and selectivity over THP-1
macrophages. The most active compound
in this series 160 (Figure 23)
displayed an activity of 0.51 μM against T. b. rhodesiense with a selectivity index
of 157 fold over human THP-1 cells. Animal
studies were not carried out, and the mode of action of these compounds
is unknown.
Inhibition of T. brucei by curcuminoid
analogs was reported by Changtam et al.
327
The naturally occurring curcuminoids exhibited low potency against T. brucei. To enhance
the activity the authors made several
structural modifications to these curcuminoids to get 43 different
analogs. Thirteen compounds from this library displayed submicromolar
activity, notably compound 161 with an IC50 of 0.053 μM against T. b. brucei. Compound
161 was equally potent against T. b. brucei strains resistant to diamidines and melaminophenyl
arsenical drugs.
In addition the compound exhibited a selectivity index of 453-fold
over the human embryonic kidney (HEK) cell line.
6.5
Lead Structures Resulting from Phenotypic
Screens
A high throughput screen was carried out at the Genomics
Institute of the Novartis Research Foundation designed to identify
new small molecules with antiparasitic activity toward T.
brucei within a library of 700 000 compounds.
328
Substituted 2-phenyl-imidazopyrines from this
screen were studied in detail. Several compounds in this series including
compound 162 (Figure 23) blocked T. b. brucei growth with an IC50 in the 2–4
nM range. Compound 162 showed good penetration into the
brain which may translate into a drug candidate for stage-II infection.
This compound displayed excellent oral pharmacokinetics in mice and
cured mice of stage-I T. brucei infection when dosed
twice a day at 5 mg/kg orally for 5 days.
328
A similar lead was found independently by Ferrins et al. by a high
throughput phenotypic screen of 87 00 compounds for growth
arrest of T. brucei.
329
The target for these compounds is not yet known.
Hwang et
al. reported the optimization of chloronitrobenzamides found in a
phenotypic screen against T. brucei.(330) Compound 163 blocked T.
brucei growth in vitro with an IC50 in the 2–10
nM range and did not inhibit mammalian cell growth at micromolar concentrations.
This compound showed excellent stability to liver microsomes in vitro.
No in vivo data of antiparasite efficacy was reported, and the mechanism
of action of these compounds is not known.
6.6
Target
Based Approaches for HAT
RNA
interference knockdown studies suggested that T. brucei
N-myristoyltransferase is a valid drug target as
a decrease in this enzyme lead to parasite growth arrest in vitro
and a negation of infectivity of parasites in mice.
331
Brand et al. reported the optimization of an N-myristoyltransferase inhibitor discovered
via high throughput screening.
332
Compound 164 with an in vitro
IC50 of 2 nM against T. brucei was identified.
The compound cured rodents of stage-I infection with T. b.
rhodesiense and T. b. brucei after oral
dosing. Overexpression of N-myristoyltransferase
in parasites leads to a shift of IC50 to higher concentration
thus providing strong evidence that this enzyme is the target of these
compounds. Also, compound 164 blocked incorporation of
radiolabeled myristic acid into parasite proteins. Unfortunately,
these compounds do not enter the brain and thus cannot be developed
as stage-II drug candidates.
Gelb, Hamilton, Buckner, Van Voorhis,
and their co-workers reported extensive work on T. brucei farnesyltransferase inhibitors
as antiparasite agents.
333
This enzyme attaches 15-carbon farnesyl groups
to the C-terminus of a specific set of parasite proteins (human cells
contain a similar enzyme). Farnesyltransferase inhibitors have been
extensively developed by pharma as anticancer drug candidates, and
thus a wealth of farnesyltransferase inhibitors are available for
repurposing to treat HAT. Unfortunately, after extensive studies,
inhibitors that are potent on the parasite enzyme could not be modified
to improve pharmacokinetic properties. Furthermore, farnesyltransferase
inhibitors with good pharmacokinetic properties in humans and that
entered anticancer clinical trials were not potent on the T. brucei ortholog. The
reasons for this interspecies inhibitor
specificity is not apparent since almost all of the residues in the
parasite enzyme seem to be conserved with those in the active site
of human farnesyltransferase, for which a crystal structure is available.
Trypanothione reductase has been extensively studied as a drug
target for HAT. Recent work in this area by Martyn et al. involved
a high throughput screen against a library of 134,500 compounds.
334
One compound from this work is 165 with an IC50 of 0.68 μM against T. brucei and a
59-fold selectivity for trypanothione reductase over human
glutathione reductase. No in vivo studies for these compounds were
reported.
Cavalli et al. reported the antitrypanosomal activity
of quinazoline
derivatives that target trypanothione reductase, a flavoenzyme essential
for the parasite survival.
335
The authors
reported several low micromolar quinazoline based inhibitors for T. b. rhodesiense
which also inhibited the enzyme in vitro.
The best compound in the series 166 had a potency of
0.12 μM against bloodstream T. brucei rhodesiense and a 23-fold selectivity over mammalian
L6 cells.
Using virtual
screening, Mpamhanga et al. identified two scaffolds
for the inhibition of the T. brucei pteridine reductase
1 (TbPTR1), an enzyme essential for parasite survival.
336
On the basis of the crystal structure of one
of these compounds bound to the enzyme, further analogs were designed
to increase the potency, selectivity and favorable physicochemical
properties. To fill the hydrophobic pocket near the binding site,
a phenyl group was added to the parent structure to get compound 167. This compound
displays an apparent K
I
value of K
i
app 0.007 μM
on the pteridine reductase 1 and was 100-fold more active than the
parent compound and displayed good selectivity over human versus parasite
enzyme. However, this compound displayed poor inhibition of T. brucei cell growth
in culture with IC50 of 10 μM and no animal data
was reported.
Mallari et al. reported purine-derived nitriles
as antitrypanosomal
agents by targeting the trypanosomal cathepsin B.
337
Through a structure guided lead development, inhibitors
of this enzyme with good selectivity for the parasite enzyme over
human cathepsins B and L was reported. The most potent compound in
the series compound 168 had an in vitro IC50 of 0.46 μM against T. brucei cathepsin
B
and 0.03 μM against rhodesain, a trypanosomal cathepsin L-type
protease. Further it also possesses selective trypanocidal activity
with an IC50 of 0.56 μM against T. brucei. No animal data was reported.
Ochiana et al. reported the
repurposing of a human Aurora kinase
inhibitor scaffold for specifically targeting trypanosomal Aurora
kinase 1.
338
An SAR investigation was done
on an established human Aurora kinase inhibitor 169 by
focusing on decreasing the activity against the acute myelogenous
leukemia cell line (MOLT-4) and maintaining the activity against T. brucei rhodesiense.
The study yielded compounds with
selectivity indices ranging from 2- to 23-fold. Compound 170 was the most selective
with a potency of 0.61 μM against T. brucei rhodesiense and a selectivity ratio of
23 against
MOLT-4. No animal studies were reported.
Hirth et al. reported
the antitrypanosomal activity of the base
modified adenosine derivatives that target S-adenosylmethionine decarboxylase
(AdoMetDC), an enzyme that is essential in the synthesis of polyamines
critical for trypanosomes survival.
339
The
8-methyl adenosyl derivative 171 was the most active
compound in this series with an IC50 of 0.001 μM
against T. brucei rhodesiense and 0.027 μM
against T. brucei brucei. This compound was observed
to possess good blood brain barrier penetration based on an intraperitoneal
administration study on mice.
Peptidic Michael acceptor-based
inhibitors of trypanosomal cysteine
proteases, called rhodesain, exhibiting antitrypanosomal activity
were reported by Breuning et al.
340
A library
of 45 fumaric acid-based peptidic analogs containing Asn, Gln, or
Phe residues were synthesized and tested against rhodesain from T. b. rhodesiense.
In general it was observed that the E
isomers were more potent than the corresponding Z isomers, and most
of the compounds in this series were nontoxic to mammalian macrophages.
The most active compound in this series against T. brucei
brucei was 172 with IC50 of 0.25
μM against T. b. brucei and a K
I
of 7.6 μM against rhodesain.
No animal studies were reported.
Figure 23
Miscellaneous anti-HAT compounds.
7
Concluding
Remarks
In summary, there has been significant progress in
the treatment
of both leishmaniasis and HAT during the past decade. Newly introduced
VL treatments, which include paromomycin, miltefosine, geographic
extensions of liposomal amphotericin B, and various drug combinations,
have substantially improved options for patients affected by VL. This
has been especially critical for treating VL cases in the state of
Bihar, India, where resistance toward pentavalent antimonials is widely
spread. Similarly, the treatment of stage II HAT patients dramatically
improved in recent years as the result of the introduction of nifurtimox-eflornithine
combination therapy (NECT). There is insufficient data to firmly establish
the clinical efficacy of various regimens used for treatment of CL.
Many of these infections are self-healing and the decision to initiate
treatment is typically determined by the nature of lesions and risk
of developing MCL.
However, in spite of this recent progress,
new drugs for both leishmaniasis
and HAT are still urgently needed. Treatment options for patients
with VL in East Africa, HIV-VL coinfections, and those with PKDL diagnosis
are still inadequate, and new drugs that are inexpensive, orally bioavailable,
short acting, and do not require hospitalization, would dramatically
improve the treatment of VL patients in endemic areas. For HAT, the
current treatment options are even more limited, thus making the situation
dire. The current target profile necessitates for drug candidates
to be effective against both stage I and stage II disease. This makes
the task scientifically challenging as only a small percentage of
chemical leads have the potential to penetrate the BBB. Currently,
the number of infected individuals is uncertain and probably lower
than during other times because of public health campaigns. However,
even with the low numbers, HAT disease figures in the top 10 of diseases
responsible for loss of life and productivity in the African continent.
341
The drug pipelines for both diseases
are very thin: very few compounds
are in development and drug discovery efforts are limited. There are
only two compounds in clinical trials for HAT (nifurtimox, SCYX-7158)
and one for VL (nifurtimox) making the need for enriching the pipeline
with novel chemical entities of critical importance.
Related collections
Most cited references265

- Record: found
- Abstract: found
- Article: found
Long Term Outcomes Following Hospital Admission for Sepsis Using Relative Survival Analysis: A Prospective Cohort Study of 1,092 Patients with 5 Year Follow Up
Joshua Davis, Vincent He, Nicholas Anstey … (2014)
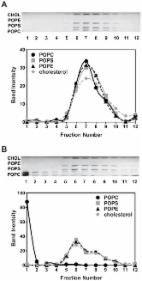
- Record: found
- Abstract: found
- Article: found
Preparation of Artificial Plasma Membrane Mimicking Vesicles with Lipid Asymmetry
Qingqing Lin, Erwin London (2014)

- Record: found
- Abstract: found
- Article: found
Outcomes in Patients with Acute and Stable Coronary Syndromes; Insights from the Prospective NOBORI-2 Study
Farzin Fath-Ordoubadi, Erik Spaepen, Magdi El-Omar … (2014)
