- Record: found
- Abstract: found
- Article: found
Acupuncture for Paclitaxel-Induced Peripheral Neuropathy: A Review of Clinical and Basic Studies
Abstract
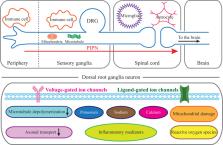
Paclitaxel-induced peripheral neuropathy (PIPN) is a common and intractable side effect of the conventional chemotherapeutic agent paclitaxel. Acupuncture has been reported as an effective alternative therapy in treatment of PIPN in both basic studies and clinical trials. However, there is a lack of comprehensive surveys to summarize the action of acupuncture in management of PIPN. In this review, we briefly demonstrate the basic pathology of PIPN, which includes the activation of ion channels, mitochondrial dysfunction, disruption of axonal transport and also neuro-inflammatory involvement. Meanwhile, we review both the clinical and basic studies as an emphasis to give a general overview of the therapeutic effect of acupuncture against PIPN. Finally, we summarize the current known mechanisms underlying the action of acupuncture against PIPN mainly at peripheral and spinal levels, which include various neurotransmitters, multiple receptors, different types of enzymes and molecules. In conclusion, acupuncture could be considered as a potential alternative therapy in treatment of PIPN, and further clinical and experimental studies are called for in the future.
Most cited references90
- Record: found
- Abstract: found
- Article: not found
Inflammasomes: mechanism of assembly, regulation and signalling.
- Record: found
- Abstract: found
- Article: not found
Prevention and management of chemotherapy-induced peripheral neuropathy in survivors of adult cancers: American Society of Clinical Oncology clinical practice guideline.
- Record: found
- Abstract: found
- Article: not found