- Record: found
- Abstract: found
- Article: found
Rare complications of neurofibromatosis 1 diagnosed incidentally in two children
other
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
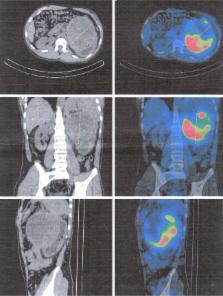
Neurofibromatosis 1 (NF1) is an autosomal-dominant disorder with various clinical expressivity and complications. Arterial hypertension may be present in patients with NF1 and is secondary to vasculopathy or pheochromocytoma. We herein describe two children (17 and 4 years old) diagnosed late with NF1 after severe arterial hypertension had been discovered due to pheochromocytoma and middle aortic syndrome. Routine measurement of arterial pressure is mandatory in children with NF1, in order to diagnose the complications of this disease.
Most cited references17
- Record: found
- Abstract: found
- Article: not found
Guidelines for the diagnosis and management of individuals with neurofibromatosis 1.
Rosalie E Ferner, Susan Huson, Nick Thomas … (2007)
- Record: found
- Abstract: found
- Article: not found
Vascular abnormalities in patients with neurofibromatosis syndrome type I: clinical spectrum, management, and results.
Peter Gloviczki, Gustavo S Oderich, Veronica Miller … (2007)
- Record: found
- Abstract: found
- Article: not found
von Recklinghausen's disease and pheochromocytomas.
M M Walther, Ronald J. Herring, E Enquist … (1999)