- Record: found
- Abstract: found
- Article: found
The Time is Now to Control Typhoid
research-article
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
The death of Prince Albert, married to Queen Victoria of the United Kingdom, in 1861
from typhoid profoundly impacted the Monarchy. The queen mourned for the rest of her
life, some 40 years, highlighting the individual and familial impact of typhoid in
a very public way [1]. The diagnosis was made by the prince’s physician, Sir William
Jenner [2], who managed many typhoid patients and meticulously documented the prince’s
symptoms, including the appearance of rose spots.
As a result of municipal clean water and sewage works, typhoid has essentially disappeared
from the wealthy nations of the world, with almost all cases in Europe and North America
now attributed to travel to endemic regions. However, there are still thought to be
nearly 12 million cases and more than 128 000 deaths each year associated with Salmonella
serotype Typhi [3]. Cases occur largely in resource-poor regions of the world, sub-Saharan
Africa, and South/Southeast Asia, where there is limited access to clean water and
inadequate sanitation [4, 5]. In these communities, the disease continues to have
the same profound impact on families as was experienced by Queen Victoria. Fortunately,
with the availability of antimicrobial therapy, the mortality from typhoid has fallen
from the high levels of the preantibiotic era. Recently, however, extensively drug-resistant
(XDR) S. typhi variants have emerged in India, Bangladesh, the Philippines, Iraq,
and Guatemala, and, importantly, have caused a large outbreak in Pakistan [6, 7],
further threatening the health of these populations.
Since 2008, the World Health Organization (WHO) has advocated vaccine control of typhoid
[8], but uptake has been slow due to lack of a suitable vaccine for children aged
<2 years. Of course, typhoid can be controlled by use of clean water and improved
sanitation and hygiene, which would stop the spread of typhoid and other water- and
foodborne enteric pathogens. However, we cannot wait for safe water and proper sanitation
to be available for every child; too many will suffer from enteric fever if we do
not act. It is time to control typhoid now.
The Typhoid Vaccine Acceleration Consortium (TyVAC) [9], funded by the Bill & Melinda
Gates Foundation, launched in 2017 as a partnership of the Center for Vaccine Development
and Global Health at the University of Maryland School of Medicine, the Oxford Vaccine
Group at the University of Oxford, and PATH, an international nonprofit organization.
TyVAC’s mission is to protect children who suffer the greatest burden by accelerating
the use of typhoid conjugate vaccine (TCV) in Africa and Asia. As a major component,
the consortium is evaluating Typbar-TCV, the leading vaccine candidate, to provide
data to support introduction of the vaccine in those regions suffering a substantial
burden of disease. The studies were designed to be complementary to each other and
to other efforts, including data available from the vaccine manufacturer and partners
[10].
This supplement highlights some of the current and future work of TyVAC and its associates.
The approach is similar to that used to help drive global introductions of other vaccines,
as summarized by Jamka et al [11]. With the March 2018 WHO-revised typhoid position
paper and the current Gavi, the Vaccine Alliance, funding window for TCV introduction,
the supplement provides key data on vaccine efficacy and immunogenicity in sub-Saharan
Africa and Southeast Asia. The supplement includes methods papers for the 4 TyVAC
sites and articles on health economics, modeling, demand forecasting, global incidence,
public engagement and lessons learned, antimicrobial resistance, decision-making,
data management, and accelerating TCV introduction.
The supplement includes a systematic review of data on the global burden of typhoid
[12] and a series of important articles on new burden data from Myanmar, Democratic
Republic of Congo, Bangladesh, and Tanzania [13–16]. As identified in these articles,
and others published recently [17, 18], typhoid is far more widespread than might
be appreciated from the microbiological literature. Surveillance for the disease requires
microbiological culture facilities since the clinical syndrome is largely indistinguishable
from other illnesses that present with fever, making syndromic surveillance unhelpful.
Unfortunately, the regions with the highest rates of typhoid often have the least
developed laboratory facilities, emphasizing the importance of these studies in supporting
vaccine deployment and control of the disease. Lack of country- and regional-level
surveillance data is one of the main challenges for decision-makers.
Vaccine efficacy of 54%–87% was recently demonstrated using a controlled human infection
model of typhoid [19], which strongly supports the likely efficacy of Typbar-TCV,
manufactured by Bharat Biotech. The study was run using human adult volunteers in
Oxford, United Kingdom, who had not lived in an endemic area but received 10 000 bacteria
as the infection challenge after neutralization of gastric acid. It is unclear how
efficacy in the model relates to performance of this TCV in children in an endemic
region where there are currently no field efficacy data. Liu et al [20] discuss the
design and analysis of seroefficacy studies for TCVs.
TCV was licensed and recommended by WHO based on immunogenicity data and a human controlled
infection model in nonendemic adults, but the lack of field data at this time undermines
confidence at the country level of the potential impact. Given limitations on health
budgets, many countries will need more information before deciding to introduce a
vaccine, particularly data are needed on impact, how programs might be structured,
and how the vaccine performs in different transmission settings. As part of the TyVAC
program, we are undertaking individually randomized clinical trials in Malawi and
Nepal and a cluster-randomized trial in Bangladesh. The protocols for these studies
are summarized in this supplement, in addition to an immunogenicity trial protocol
from Burkina Faso [21–24]. In the efficacy trials, more than 85 000 children from
age 9 months to age 15 years were vaccinated during late 2017 through the first half
of 2018. Given that duration of immunity is critically important to country-level
decisions on vaccine introduction, these children will be followed for at least 2
years using enhanced passive microbiological surveillance (blood cultures), with vaccine
efficacy measures available by 2020. The control vaccine in these studies is either
a capsular group A meningococcal vaccine (Nepal and Malawi), as this is the main agent
causing meningococcal disease in these regions, or Japanese encephalitis vaccine in
Bangladesh, since this disease is important in rural areas of that country. Given
the importance of typhoid in the population, control-arm children in Nepal and Bangladesh
will receive TCV at the end of the study. In Malawi, the epidemiology and burden are
less certain; therefore, the decision on whether or not to provide TCV for children
in the control group will be made in concert with Malawian health officials once data
are available. Other typhoid vaccines were not considered for control vaccines because
they are not licensed for the youngest children, do not confer long-term protection,
and, therefore, are less suitable for routine country introduction. Another important
outstanding question is the potential role of TCV in reducing transmission of typhoid
in the field and thus inducing herd protection, as was recently indicated as possible
in studies using the human challenge model [25]. The TyVAC field trials will directly
address this through the cluster-randomized trial in Bangladesh. Taken together, the
data from the TyVAC trials will provide valuable information to inform vaccine deployment
in Africa and Asia, and we anticipate reassurance on field safety will be important
for national immunization technical advisory groups (NITAGs) and health ministers,
when considering introduction of new TCVs. The process of obtaining funding for introductions,
especially through international donors, is slow. The TyVAC trials will provide important
data ahead of possible introductions in most countries [26].
Important components of vaccine field studies that are rarely described in the scientific
literature are logistical elements of study delivery and the role and implementation
of public engagement. Two articles in this supplement deal with these issues and provide
a high-level view that we anticipate will be useful for deployment of clinical studies
in the future [27, 28].
As mentioned above, antimicrobial resistance is a major threat to the health of populations
in which Salmonella infections are prevalent as these bacteria readily pick up resistance
genes. Multidrug resistance (MDR, defined as resistance to the first-line antibiotics
ampicillin, cotrimoxazole, and chloramphenicol) was recognized several decades ago
and became widespread among the agents of enteric fever. However, there has been a
decline in resistance over the past 10 years, especially in South Asia, as antibiotic
pressure was reduced after these drugs became redundant in typhoid treatment [29].
More recent use of fluoroquinolones has driven very widespread acquisition of resistance
to this class of antibiotic; currently severe cases often must be treated with cephalosporins
and milder cases with azithromycin. A recent outbreak of XDR typhoid (defined as MDR
plus resistance to fluoroquinolones and cephalosporins) has been identified in Pakistan
[7], considerably reducing treatment options. In this supplement, we provide insight
into antimicrobial resistance (AMR) from genomic analyses of typhoid strains [30]
and country-specific data on AMR in the enteric fever burden studies. Introduction
of new TCVs will impact AMR infections in the same way as susceptible typhoid, and
our modeling article summarizes predicted vaccine impact [31].
In October 2017, TyVAC provided evidence for WHO’s Strategic Advisory Group of Experts
(SAGE) on Immunization that recommended the use of new TCVs. Also, WHO supplied information
for Gavi, the Vaccine Alliance, to support Gavi’s planning for TCV financing, with
$85 million provided for vaccine deployment as outlined by Jamka et al [11]. An important
component of country decision-making for new vaccines, especially for those graduating
from Gavi support for new vaccine programs in the next 5 years, is the economics of
vaccine introduction. In this supplement, we include a review of typhoid vaccine economic
studies and summarize plans for further work of the TyVAC consortium [32]. For manufacturers
and vaccine financiers (Gavi), an accurate demand forecast is important to ensure
supply meets demand and funds are available to purchase products. Reducing uncertainty
is important for country-level decisions, as highlighted by supply shortages for other
vaccines in recent years, which have caused difficulties for national programs. The
demand-forecasting article describes the model built to estimate TCV demand [33].
Finally, in this supplement, we discuss the importance of communications about typhoid,
which must involve international, national, and local-level stakeholders. This ensures
that SAGE recommendations are translated into appropriate decisions by the NITAG,
with government support, and are clear and understood by local public health immunization
officials and frontline staff so that new programs are introduced rapidly and with
clarity for the benefit of the population [34].
The articles in this supplement show the development of high-quality evidence by TyVAC
to inform decision-making on TCV introduction. Through the data produced and the advocacy
of TyVAC, we are tasked with improving health among some of the most vulnerable populations
in the world through introduction of TCVs where they are most needed to drive substantial
and clinically meaningful reductions in typhoid burden. There should be no more families
to mourn like Queen Victoria did. It is time to control typhoid.
Related collections
Most cited references25

- Record: found
- Abstract: found
- Article: found
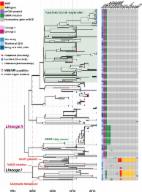
Laboratory and molecular surveillance of paediatric typhoidal Salmonella in Nepal: Antimicrobial resistance and implications for vaccine policy
Carl D. Britto, Zoe A. Dyson, Sebastian Duchêne … (2018)