- Record: found
- Abstract: found
- Article: not found
Treatment with an Anti-CK2 Synthetic Peptide Improves Clinical Response in COVID-19 Patients with Pneumonia. A Randomized and Controlled Clinical Trial

Read this article at
Abstract
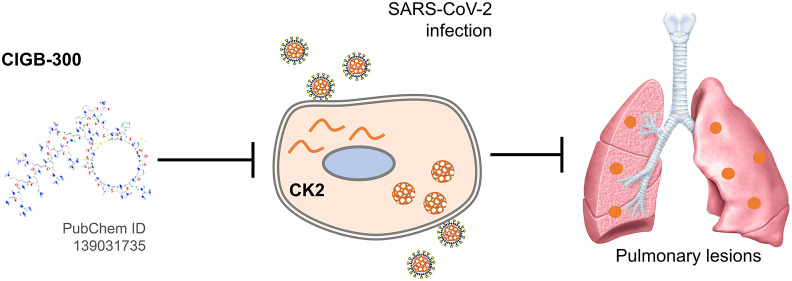
The instrumental role of CK2 in the SARS-CoV-2 infection has pointed out this protein kinase as promising therapeutic target in COVID-19. Anti-SARS-CoV-2 activity has been reported by CK2 inhibitors in vitro; however, no anti-CK2 clinical approach has been investigated in COVID-19. This trial aimed to explore the safety and putative clinical benefit of CIGB-325, an anti-CK2 peptide previously assessed in cancer patients. A monocentric, controlled, and therapeutic exploratory trial of intravenous CIGB-325 in adults hospitalized with COVID-19 was performed. Twenty patients were randomly assigned to receive CIGB-325 (2.5 mg/kg/day during 5-consecutive days) plus standard-of-care (10 patients) or standard-of-care alone (10 patients). Adverse events were classified by the WHO Adverse Reaction Terminology. Parametric and nonparametric statistical analyses were performed according to the type of variable. Considering the small sample size, differences between groups were estimated by Bayesian analysis. CIGB-325 induced transient mild and/or moderate adverse events such as pruritus, flushing, and rash in some patients. Both therapeutic regimens were similar with respect to SARS-CoV-2 clearance in nasopharynx swabs over time. However, CIGB-325 significantly reduced the median number of pulmonary lesions (9.5 to 5.5, p = 0.042) at day 7 and the proportion of patients with such an effect was also higher according to Bayesian analysis (pDif > 0; 0.951). Also, CIGB-325 significantly reduced the CPK ( p = 0.007) and LDH ( p = 0.028) plasma levels at day 7. Our preliminary findings suggest that this anti-CK2 clinical approach could be combined with standard-of-care in COVID-19 in larger studies.
Related collections
Most cited references23
- Record: found
- Abstract: found
- Article: found
Remdesivir for the Treatment of Covid-19 — Final Report
- Record: found
- Abstract: found
- Article: not found
