- Record: found
- Abstract: found
- Article: found
Effect of long-term high-fat diet intake on peripheral insulin sensibility, blood pressure, and renal function in female rats
Read this article at
Abstract
Background
This study determines whether 8-week high-fat diet (HFD) consumption alters insulin sensitivity, kidney function, and blood pressure (BP) in female rats when compared with standard rodent diet (ND) intake in gender- and age-matched rats.
Methods
The present study investigates, in female Wistar HanUnib rats, the effect of long-term high-fat fed group (HFD) compared with standard chow on BP by an indirect tail-cuff method using an electrosphygmomanometer, insulin and glucose function, and kidney function by creatinine and lithium clearances.
Results
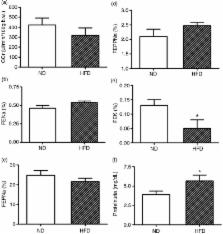
The current study shows glucose tolerance impairment, as demonstrated by increased fasting blood glucose (ND: 78±2.8 vs. HFD: 87±3.8 mg/dL) associated with reduced insulin secretion (ND: 0.58±0.07 vs. HFD: 0.40±0.03 ng/mL) in 8-week female HFD-treated rats. The incremental area under the curve (AUC, ND: 1,4558.0±536.0 vs. HFD: 1,6507.8±661.9), homeostasis model assessment of insulin resistance (HOMA-IR) index, and the first-order rate constant for the disappearance of glucose ( Kitt) were significantly enhanced in 8-week HFD-treated rats compared with age-matched ND group (respectively, P=0.03, P=0.002, and P<0.0001). The current study also shows a significantly higher systolic BP measured in 5 and 8 weeks posttreatment in HFD (5-week HFD-treated: 155.25±10.54 mmHg and 8-week HFD-treated: 165±5.8 mmHg) ( P=0.0001), when compared to BP values in 5-week ND, 137±4.24 mmHg and 8-week ND, 131.75±5.8 mmHg age-matched group. Otherwise, the glomerular filtration rate and renal sodium handling evaluated by FE Na, FEP Na and FEPP Na, were unchanged in both groups.
Related collections
Most cited references35
- Record: found
- Abstract: found
- Article: not found
Diet-induced obesity in C57BL/6J mice causes increased renal lipid accumulation and glomerulosclerosis via a sterol regulatory element-binding protein-1c-dependent pathway.

- Record: found
- Abstract: found
- Article: found
Age, Obesity, and Sex Effects on Insulin Sensitivity and Skeletal Muscle Mitochondrial Function
- Record: found
- Abstract: found
- Article: not found