- Record: found
- Abstract: found
- Article: found
A comparison of the postoperative analgesic efficacy between epidural and intravenous analgesia in major spine surgery: a meta-analysis
Abstract
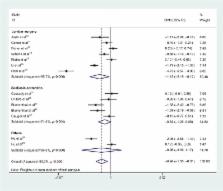
Postoperative analgesia remains a challenge for orthopedic surgeons. The aim of this meta-analysis is to compare the efficacy of epidural analgesia (EA) and intravenous patient-controlled analgesia (IV-PCA) following major spine surgery. We searched electronic databases, including the PubMed, EMBASE, Ovid and Cochrane databases, for randomized controlled trials (RCTs) published before June 2016. The quality of the included trials was assessed using the Cochrane risk-of-bias tool. Random effects models were used to estimate the standardized mean differences (SMDs) and relative risks (RRs), with the corresponding 95% confidence intervals (CI). Subgroup analyses stratified by the type of epidural-infused medication and epidural delivery were also performed. A total of 17 trials matched the inclusion criteria and were chosen for the following meta-analysis. Overall, EA provided significantly superior analgesia, higher patient satisfaction and decreased overall opioid consumption compared with IV-PCA following major spine surgery. Additionally, no differences were found in the side effects associated with these two methods of analgesia. Egger’s and Begg’s tests showed no significant publication bias. We suggest that EA is superior to IV-PCA for pain management after major spine surgery. More large-scale, high-quality trials are needed to verify these findings.
Most cited references34
- Record: found
- Abstract: found
- Article: not found
Efficacy of postoperative epidural analgesia: a meta-analysis.
- Record: found
- Abstract: found
- Article: not found
Effectiveness of acute postoperative pain management: I. Evidence from published data.
- Record: found
- Abstract: found
- Article: not found