- Record: found
- Abstract: found
- Article: found
Stress urinary incontinence is caused predominantly by urethral support failure
Read this article at
Abstract
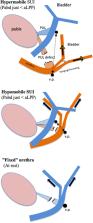
Whales are mammals that can dive to depths of > 1000 m without the high water pressure pushing open their mouth or anus. The same is true for the female urethra. The meatus externus and internus are seals that cannot be pushed open by high water pressures. Recent evidence suggests that the female meatus internus is pushed open when the bladder pressure exceeds the urethral pressure. For a relaxed detrusor, this opening is not possible for at least three reasons: the law of elastic collision, Pascal’s law of hydrostatics and the Hagen-Poiseuille law. The three laws do not support that urethral function failure is the predominant cause of stress urinary incontinence (SUI); however, they do support that urethral support failure is. Influential urogynecologists claim the opposite. TVT surgery, according to the integral theory of SUI (IT), has high failure rates because it does not principally prevent the urethra from hanging on a less mobile bladder neck. In the case of a long urethra, the tape is set too distally, and in hypomobile SUI, the use of a tension-free suburethral tape is unwarranted/ineffective, because the proximal urethra is not elevated above its resting position. A successful operation corrects urethral support failure and not urethral function failure.
Related collections
Most cited references26
- Record: found
- Abstract: not found
- Article: not found
An ambulatory surgical procedure under local anesthesia for treatment of female urinary incontinence
- Record: found
- Abstract: found
- Article: not found
Retropubic versus transobturator midurethral slings for stress incontinence.
- Record: found
- Abstract: found
- Article: not found