- Record: found
- Abstract: found
- Article: found
Locoregional extension patterns of nasopharyngeal carcinoma and suggestions for clinical target volume delineation
Read this article at
Abstract
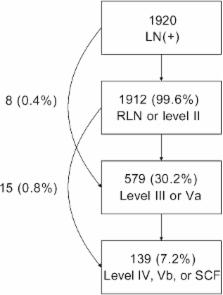
Clinical target volume (CTV) delineation is crucial for tumor control and normal tissue protection. This study aimed to define the locoregional extension patterns of nasopharyngeal carcinoma (NPC) and to improve CTV delineation. Magnetic resonance imaging scans of 2366 newly diagnosed NPC patients were reviewed. According to incidence rates of tumor invasion, the anatomic sites surrounding the nasopharynx were classified into high-risk (>30%), medium-risk (5%–30%), and low-risk (<5%) groups. The lymph node (LN) level was determined according to the Radiation Therapy Oncology Group guidelines, which were further categorized into the upper neck (retropharyngeal region and level II), middle neck (levels III and Va), and lower neck (levels IV and Vb and the supraclavicular fossa). The high-risk anatomic sites were adjacent to the nasopharynx, whereas those at medium- or low-risk were separated from the nasopharynx. If the high-risk anatomic sites were involved, the rates of tumor invasion into the adjacent medium-risk sites increased; if not, the rates were significantly lower ( P < 0.01). Among the 1920 (81.1%) patients with positive LN, the incidence rates of LN metastasis in the upper, middle, and lower neck were 99.6%, 30.2%, and 7.2%, respectively, and skip metastasis happened in only 1.2% of patients. In the 929 patients who had unilateral upper neck involvement, the rates of contralateral middle neck and lower neck involvement were 1.8% and 0.4%, respectively. Thus, local disease spreads stepwise from proximal sites to distal sites, and LN metastasis spreads from the upper neck to the lower neck. Individualized CTV delineation for NPC may be feasible.
Related collections
Most cited references29
- Record: found
- Abstract: found
- Article: not found
How does intensity-modulated radiotherapy versus conventional two-dimensional radiotherapy influence the treatment results in nasopharyngeal carcinoma patients?
- Record: found
- Abstract: found
- Article: not found
Intensity-modulated radiotherapy in the treatment of nasopharyngeal carcinoma: an update of the UCSF experience.
- Record: found
- Abstract: found
- Article: not found