- Record: found
- Abstract: found
- Article: found
No association between exacerbation frequency and stroke in patients with COPD
Abstract
Background
Patients with chronic obstructive pulmonary disease (COPD) have a higher risk of stroke than the general population. Chronic inflammation associated with COPD is thought to contribute to this risk. Exacerbations of COPD are associated with a rise in inflammation, suggesting that there may be an association between exacerbation frequency and the risk of stroke. This study examined that association.
Methods
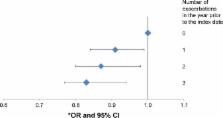
Using the UK Clinical Practice Research Datalink, COPD patients with a first stroke between January 2004 and December 2013 were identified as cases and matched on age, sex, and general practice to controls with COPD but without a stroke (6,441 cases and 19,323 controls). Frequent exacerbators (FEs) were defined as COPD patients with ≥2 exacerbations, and infrequent exacerbators (IEs) have ≤1 exacerbation in the year prior to their stroke. Conditional logistic regression was used to estimate the association between exacerbation frequency and stroke overall, and by stroke subtype (hemorrhagic, ischemic, or transient ischemic attack). Exacerbations were also categorized into 0, 1, 2, or ≥3 exacerbations in the year prior to stroke.
Results
There was no evidence that FE had an increased odds of stroke compared to IE (OR [odds ratio] =0.95, 95% CI [confidence interval] =0.89–1.01). There was strong evidence that the risk of stroke decreased with each exacerbation of COPD experienced per year ( P trend =0.003). In the subgroup analysis investigating stroke subtype, FE had 33% lower odds of hemorrhagic stroke than IE (OR =0.67, 95% CI =0.51–0.88, P=0.003). No association was found within other stroke types.
Conclusion
This study found no evidence of a difference in the odds of stroke between IE and FE, suggesting that exacerbation frequency is unlikely to be the reason for increased stroke risk among COPD patients. Further research is needed to explore the association through investigation of stroke risk and the severity, duration, treatment of exacerbations, and concurrent treatment of cardiovascular risk factors.
Most cited references13
- Record: found
- Abstract: found
- Article: not found
Alternative projections of mortality and disability by cause 1990–2020: Global Burden of Disease Study
- Record: found
- Abstract: found
- Article: not found
Susceptibility to exacerbation in chronic obstructive pulmonary disease.
- Record: found
- Abstract: found
- Article: not found