- Record: found
- Abstract: found
- Article: found
Mechanisms underlying low-clinical responses to PD-1/PD-L1 blocking antibodies in immunotherapy of cancer: a key role of exosomal PD-L1
Read this article at
Abstract
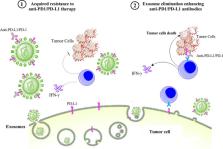
Exosomes, as the main group of extracellular vesicles, are biologically active lipid-bilayer vesicles that are naturally released from different types of normal or tumor cells. These vesicles play an important role in intercellular communication and influence the extracellular environment and the immune system. Emerging evidence demonstrates that cancer-derived exosomes are enriched in immunosuppressive proteins, such as the programmed death-ligand 1 (PD-L1). PD-L1 and its receptor programmed cell death protein 1 (PD-1) are the key immune checkpoint molecules that promote tumor progression via negative regulation of immune responses. PDL-1 is highly expressed on the surface of tumor cells and binds to PD-1 on the surface of activated T cells, leading to suppression of T cells, which consequently enables cancer cells to escape antitumor immunity. Currently, there are several Food and Drug Administration-approved monoclonal antibodies blocking PD-1/PD-L1 interaction, which are clinically used for cancer treatment. However, despite impressive treatment outcomes, some patients show poor response to PD-1/PD-L1 blockade. Of note, tumor-derived exosomes containing PD-L1 can recapitulate the effect of cell-surface PD-L1. There is evidence that reveals a significant association between levels of circulating exosomal PD-L1 and rate of response to anti-PD-1/PD-L1 antibody therapy. The present article reviews the role of exosomal PDL-1 in the therapeutic resistance to anti-PD-1/PD-L1 treatment. Importantly, it is suggested that the removal of exosomal PDL-1 could serve as a therapeutic adjuvant for enhancing the efficacy of anti-PD-1/PD-L1 therapy in patients with cancer.
Related collections
Most cited references95
- Record: found
- Abstract: found
- Article: not found
Pembrolizumab versus Chemotherapy for PD-L1–Positive Non–Small-Cell Lung Cancer
- Record: found
- Abstract: found
- Article: not found
PD-1 Blockade in Tumors with Mismatch-Repair Deficiency.
- Record: found
- Abstract: found
- Article: not found