- Record: found
- Abstract: found
- Article: found
Schisandrin B elicits the Keap1-Nrf2 defense system via carbene reactive metabolite which is less harmful to mice liver
Abstract
Background
Schisandrin B (Sch B) a main active component of Schisandra chinensis, has been shown to act as a liver protectant via activation of the Nrf2 pathway. Nevertheless, it remains unclear whether its reactive metabolite is responsible for Nrf2 activation; also, the effects of its reactive metabolite on liver function are still unknown.
Methods
The present study determined and identifed the carbene reactive metabolite of Sch B in human and mice liver microsomes. Its roles in activating Nrf2 pathway and modifying macromolecules were further explored in human liver microsomes. Moreover the potential cytotoxicity and hepatoxicity of carbene on HepG-2 and mice were also investigated.
Results
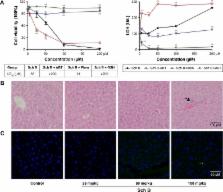
In the present study, cytochromes P450 (CYP450s) metabolized Sch B to carbene reactive metabolite, which, with the potential to modify peptides, were identifed and observed in human and mice liver microsomes. Moreover, the relevance of carbene in Nrf2 activation was verifed by co-incubation in the presence of CYP450 inhibitors in HepG-2 cells, as well as by molecular docking study of carbene and Keap1. Additionally, the cytotoxicity of Sch B on HepG-2 cells was signifcantly aggravated by CYP450 inducer (with LD 50 decreasing from 63 to 21 µM) and signifcantly alleviated by CYP450 inhibitor and glutathione (with LD 50 increasing from 63 µM to 200 µM). Besides, after oral administration of mice with Sch B (25–100 mg/kg) for 21 days, only the highest dose induced mild hepatotoxicity, which was accompanied by increasing the aminotransferase activity and centrilobular hepatocellular infltration of lymphocytes. In addition, upregulation of CYP450 activity; Nrf2, NQO-1, and GST expression; and glutathione level was observed in Sch B treatment groups.
Most cited references28
- Record: found
- Abstract: found
- Article: not found
Oral medications with significant hepatic metabolism at higher risk for hepatic adverse events.
- Record: found
- Abstract: found
- Article: not found
The protective effects of Schisandra chinensis fruit extract and its lignans against cardiovascular disease: a review of the molecular mechanisms.
- Record: found
- Abstract: found
- Article: not found