- Record: found
- Abstract: found
- Article: found
Perineal discomfort in prostatic adenocarcinoma
case-report
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
We highlight the risk of missing a high-grade (Gleason Grade 7/8) transition zone
adenocarcinoma in a patient presenting with perineal discomfort on sitting.
Introduction
Prostate cancer is the most frequent malignancy of men of all races
1
and is the biggest cause of cancer deaths in men
2
but there is continuing controversy surrounding screening for prostate cancer
3
even though the seriousness of prostate cancer is unquestioned
4
with 0.6% of cases diagnosed as early as 35–44 years of age.
5
The limitations of PSA use and, more specifically, false positives and false negatives
are well known and some investigators have tried to improve the method's sensitivity
and specificity, including PSA adjusted by age, as well as PSA density, velocity and
fractions,
6
i.e. free/total PSA ratio (%fPSA).
Despite imperfections which limit their interpretation, the recently published large
randomized screening trials show there is only a small – or no – improvement in survival
from early detection over the first 10 years.
7
However, in the recent European Randomized Study of Screening for Prostate Cancer
(ERSPC) by Schröder et al.,
8
most centres involved in the trial used a PSA cut-off value of 3 ng/mL (range of 3.0–10.0
ng/mL depending on the country involved) as an indication for biopsy; in the large
American randomized study by Andriole et al.
9
the standard US threshold of 4 ng/mL was used. Using their PSA values, Schröder et
al.
8
concluded that PSA-based screening reduced the rate of death from prostate cancer
by 20% in their 55–69 year age group of men at entry to the trial. The Andriole et
al.
9
trial concluded that, after 7–10 years of follow-up, the death rate was very low,
not differing significantly between their two study groups.
Significant prostate cancer can exist with PSA levels of 2.5–4 ng/mL.
10
Thompson et al.
11
looked at the prevalence of prostate cancer, including high-grade cancer, with PSA
levels of ≤4.0 ng/mL and found 15% had prostate cancer despite ‘normal PSA levels’,
i.e. levels generally thought to be in the normal range (4.0 ng/mL or less). A transrectal
ultrasound (TRUS) guided biopsy of the prostate gland is the only way that prostate
cancer can be diagnosed with certainty.
12
However, TRUS alone has poor test characteristics for the diagnosis of prostate cancer
with a positive predictive value of 52.7%, a negative predictive value of 72%, and
an accuracy of 67%.
13
Biopsy cancer tissue is graded microscopically using the Gleason score
14
with a possible total rating from 2–10. Fast-growing (i.e. ‘high-grade’ cancers with
a Gleason score of 7–10 usually need more radical treatment.
12
Prostate cancer frequently originates from the peripheral zone and only approximately
24% arise from the transition zone where they are difficult to diagnose.
15
Barry
16
refers to many available treatment options including surgery, radiation, cryotherapy,
and expectant management, and Jang et al.
17
state it is essential for men to have access to balanced information before choosing
a particular therapy. Hoffman et al.
18
highlight the importance of an informed and shared decision-making process between
the patient and urologist for prostate cancer screening, treatment decisions, and
their possible sequelae.
Anatomy
There are four basic anatomical regions (Figure 1): (i) anterior fibromuscular stroma;
19
(ii) peripheral zone constituting over 70% of the glandular prostate; (iii) central
zone (25%); and (iv) small transition zone consisting of two lobes essentially located
anteriorly between the proximal urethra and the lateral parts of the peripheral zone.
20
Figure 1
Side view diagram of the prostate showing the anterior fibromuscular stroma (FM),
central zone (CZ), posterior zone (PZ), transition zone (TZ), prostatic urethra (PU),
and a seminal vesicle (SV). Modified from Prostate UK (http://www.prostateuk/prg/prostate/aboutprostate.htm)
Case presentation
A healthy, active and employed 68-year-old man on no medication, and with no family
history of prostate cancer in his long-living male relatives except for his maternal
grandfather, consulted his general medical practitioner for minor discomfort/paraesthesia
in the perineal region, while seated, of approximately three weeks duration. A current
digital rectal examination (DRE) of the prostate indicated a suspicious ridge on the
right and a current PSA test showed a level of 1.8 ng/mL, the overall rise being from
only 1.2 to 1.8 ng/mL over a 15-year period. However, in view of the perineal symptom,
and the DRE finding, he was referred for an urosurgical opinion. Two questionnaires,
respectively, were completed as diagnostic tools for any possible erectile dysfunction
(International Index of Erectile Function
21
) and prostate symptoms (International Prostate Symptom Score
22
); the scores showed no dysfunction. In view of the patient's unexplained minor perineal
discomfort/paraesthesia on sitting and the DRE finding, the urologist recommended
a TRUS biopsy of the prostate gland with 12 biopsy cores. The TRUS did not show any
abnormality but the biopsy indicated a T2a adenocarcinoma with a Gleason score of
6 on the left side. Treatment options were discussed with the patient, consideration
being given to one of three approaches: ‘watchful waiting’, radiation therapy, or
a laparoscopic radical prostatectomy; the patient chose the latter approach as, in
the urologist's experience, the actual Gleason score could be higher when the excised
gland was sent for pathological evaluation.
Results
The prostate and some associated tissues were sent for pathological evaluation. In
summary, the pathology report concluded: prostate adenocarcinoma representing a high-grade
transition zone carcinoma occupying the anterior aspect on the left (Figure 2) consistent
with Gleason Grade 4 + 3 = 7, Grade 4/5 = 70% (pattern 5 = 10%), with associated intraductal
carcinoma. Tumour is prostate and specimen confined, with a volume of 2.13cc and a
pathological stage of T2a. Sections through the ejaculatory ducts, seminal vesicles
and bladder neck margin confirm all structures to be free of tumour.
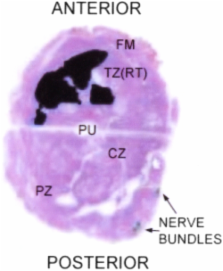
Figure 2
Prostate gland histopathology macroscopic section showing the darkly-stained transition
zone adenocarcinoma occupying the anterior aspect on the left. FM=fibromuscular stroma
anteriorly; CZ=central zone; PZ=posterior zone; TZ (RT)=transition zone on the right;
PU=prostatic urethra
Postoperatively at six weeks and three months, respectively, the patient's PSA level
was found to be 0.03 ng/mL.
Discussion
Worldwide, in 2002, more than 670,000 men were diagnosed with prostate cancer; the
highest rates were in the USA and the lowest in Asian countries.
23
It is estimated that 192,280 USA men will be diagnosed with, and 27,360 men will die
from, prostate cancer in 2009.
5
In Australia, more than 61,000 men are diagnosed with prostate cancer and another
19,000 will be diagnosed in the next year;
2
in spite of these figures, population-wide PSA screening is not recommended.
24
According to Hoffman,
3
a PSA threshold below 4.0 ng/mL should not be used to trigger biopsy referral, however,
Dall'oglio et al.
4
suggest that prostate biopsy is indicated in men with a PSA level of 2.5–4.0 ng/mL,
highlighting the current uncertainty regarding a meaningful PSA value. The PSA level
of only 1.8 ng/mL in the case presented above indicates that even a PSA level of 2.5
ng/mL can be too high. Perhaps the real indicators of the prostate adenocarcinoma
in this case were the perineal symptoms while seated, as perineal pain sometimes occurs
with prostate cancer,
25
coupled with the overall increase in PSA from 1.2 to 1.8 ng/mL over the 15-year period.
Conclusions
Of relevance to general practitioners it should be noted that, although Holmström
et al.
26
concluded from their longitudinal study that PSA has a relatively high validity for
prediction of subsequent prostate cancer, no cut-off value was established, although
PSA concentrations below 1.0 ng/mL were considered to ‘virtually rule out a diagnosis
of prostate cancer during follow-up and high PSA concentrations expressed a continuum
of prostate cancer risk’. In spite of this, Schröder et al.
8
used a cut-off value of 3.0–10.0 ng/mL depending on the European country involved
and Andriole et al.
9
used a cut-off value of 4.0 ng/mL – had they used a l.0 ng/mL cut-off they may well
have reached different conclusions, particularly as Hugosson et al.
27
recently found that mortality was reduced almost by half over a 14-year period when
using a PSA cut-off value of 3.0 ng/mL. Perhaps a 1.0 ng/mL cut-off would further
reduce mortality until newer diagnostic technology becomes available.
Based on the above, it is suggested the PSA risk level for patients should be revised
downwards and that a large clinical study should be performed using a much lower PSA
level such as 1.0 ng/mL.
DECLARATIONS
Competing interests
None declared
Funding
None
Ethical approval
Written informed consent to publication has been obtained from the patient or next
of kin
Guarantor
LG
Contributorship
LG is the sole contributor
Acknowledgements
None
Reviewer
George Fowlis
Related collections
Most cited references21
- Record: found
- Abstract: found
- Article: not found
Mortality results from a randomized prostate-cancer screening trial.
Gerald Andriole, E David Crawford, Robert L Grubb … (2009)
- Record: found
- Abstract: found
- Article: not found
Prevalence of prostate cancer among men with a prostate-specific antigen level < or =4.0 ng per milliliter.
Ian Thompson, Donna Pauler, Phyllis J. Goodman … (2004)
- Record: found
- Abstract: found
- Article: not found
Development and evaluation of an abridged, 5-item version of the International Index of Erectile Function (IIEF-5) as a diagnostic tool for erectile dysfunction.
R Rosen, J Cappelleri, M. D. Smith … (1999)