- Record: found
- Abstract: found
- Article: found
The Therapeutic Efficacy and Safety of Compound Kushen Injection Combined with Transarterial Chemoembolization in Unresectable Hepatocellular Carcinoma: An Update Systematic Review and Meta-Analysis
Read this article at
Abstract
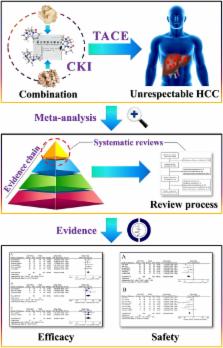
Background: Compound Kushen Injection (CKI) is a Chinese patent medicine approved by the China Food and Drug Administration for the treatment of various types of solid tumors. CKI, combined with transarterial chemoembolization (TACE), is believed to increase the therapeutic efficacy of unresectable hepatocellular carcinoma (HCC). We report an updated and extended meta-analysis with detailed outcomes of both the efficacy and adverse events (AEs) of CKI combined with TACE therapy.
Materials and methods: Electronic databases, including PubMed, Embase, the Cochrane Library, the Chinese Biomedical Database (CBM), Wanfang, the VIP medicine information system (VMIS) and the China National Knowledge Infrastructure (CNKI), were examined for relevant articles before November 13, 2015. An odds ratio (OR) was used to estimate tumor response (TR), Karnofsky Performance Scale (KPS) improvement, Child-Pugh (CP) improvement, survival rate (SR) and AEs. A publication bias and a subgroup analysis were also assessed.
Results: Eighteen studies, with a total of 1,338 HCC patients who met the criteria for the meta-analysis, were included. TR, KPS improvement and CP improvement were significantly enhanced for the combination therapy compared to TACE alone (OR = 1.84, 95% CI: [1.46, 2.33], P < 0.00001; OR = 2.37, 95% CI: [1.76, 3.18], P < 0.00001; OR = 1.81, 95% CI: [1.08, 3.03], P = 0.02, respectively). The combination therapy was associated with an improvement in 1-year and 2-year SRs but not an improved 3-year SR (OR = 2.40; 95% CI: [1.59, 3.62], P < 0.0001; OR = 2.49, 95% CI: [1.24, 5.00], P = 0.01; OR = 2.49, 95% CI: [0.94, 6.61], P = 0.07, respectively). A safety analysis indicated that AEs (including nausea/vomiting, fever, hepatalgia, increased transaminase, increased bilirubin and leukopenia) were reduced for the combination treatment compared to TACE alone.
Conclusion: The combination treatment of TACE and CKI was associated with improved TR, KPS and CP improvement and improved 1- and 2-year SRs in patients with unresectable HCC. The 3-year SR was not improved. The combination therapy resulted in a reduction in AEs. The findings of this study should be interpreted with caution because of the small sample size and study limitations.
Related collections
Most cited references14
- Record: found
- Abstract: found
- Article: not found
Randomized, multicenter, open-label study of oxaliplatin plus fluorouracil/leucovorin versus doxorubicin as palliative chemotherapy in patients with advanced hepatocellular carcinoma from Asia.
- Record: found
- Abstract: found
- Article: not found
Phase III study of sorafenib after transarterial chemoembolisation in Japanese and Korean patients with unresectable hepatocellular carcinoma.
- Record: found
- Abstract: found
- Article: not found