- Record: found
- Abstract: found
- Article: found
Non-inferiority trial of a pedal controlled injection device: a step toward enhancing patient safety and operator independence during neural blockade
Abstract
Background and objectives
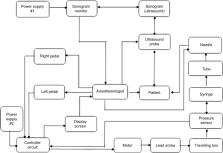
Limitations in manpower in health care facilities, both in civilian and military settings, can severely affect patient safety as well as overall outcomes. Regional anesthesia via neural blockade is an effective means of managing uncontrolled acute pain, which has been associated with cardiopulmonary, endocrine, immunologic, and hematologic derangement in addition to the development of potentially life-threatening coagulopathy. We have designed a remote-controlled injection device that may expedite the performance of regional nerve blocks in these situations.
Methods
This work examines how the device affects the ability of the operator to act independently with respect to various block component times by statistically comparing device-assisted blockade with usual or clinically relevant techniques. The classic or two-person technique was compared with the foot-controlled technique.
Most cited references4
- Record: found
- Abstract: found
- Article: not found
The ASRA evidence-based medicine assessment of ultrasound-guided regional anesthesia and pain medicine: Executive summary.
- Record: found
- Abstract: found
- Article: not found
Characterizing novice behavior associated with learning ultrasound-guided peripheral regional anesthesia.
- Record: found
- Abstract: not found
- Article: not found