- Record: found
- Abstract: found
- Article: found
Twenty-Seven Years of Phase III Trials for Patients with Extensive Disease Small-Cell Lung Cancer: Disappointing Results
Read this article at
Abstract
Background
Few studies have formally assessed whether treatment outcomes have improved substantially over the years for patients with extensive disease small-cell lung cancer (ED-SCLC) enrolled in phase III trials. The objective of the current investigation was to determine the time trends in outcomes for the patients in those trials.
Methods and Findings
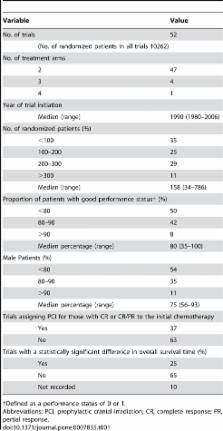
We searched for trials that were reported between January 1981 and August 2008. Phase III randomized controlled trials were eligible if they compared first-line, systemic chemotherapy for ED-SCLC. Data were evaluated by using a linear regression analysis. Results: In total, 52 trials were identified that had been initiated between 1980 and 2006; these studies involved 10,262 patients with 110 chemotherapy arms. The number of randomized patients and the proportion of patients with good performance status (PS) increased over time. Cisplatin-based regimens, especially cisplatin and etoposide (PE) regimen, have increasingly been studied, whereas cyclophosphamide, doxorubicin, and vincristine–based regimens have been less investigated. Multiple regression analysis showed no significant improvement in survival over the years. Additionally, the use of a PE regimen did not affect survival, whereas the proportion of patients with good PS and the trial design of assigning prophylactic cranial irradiation were significantly associated with favorable outcome.
Related collections
Most cited references21
- Record: found
- Abstract: found
- Article: not found
Irinotecan plus cisplatin compared with etoposide plus cisplatin for extensive small-cell lung cancer.
- Record: found
- Abstract: found
- Article: not found
Prophylactic cranial irradiation in extensive small-cell lung cancer.
- Record: found
- Abstract: found
- Article: not found