- Record: found
- Abstract: found
- Article: found
Comparison of the Chronic Kidney Disease Epidemiology Collaboration, the Modification of Diet in Renal Disease study and the Cockcroft-Gault equation in patients with heart failure
Read this article at
Abstract
Background
It is unknown how the creatinine-based renal function estimations differ for dose adjustment cut-offs and risk prediction in patients with heart failure.
Method and results
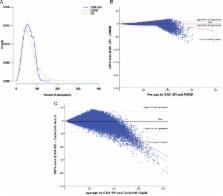
The renal function was similar with the Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) (median 59 mL/min/1.73 m 2, IQR 42 to 77) and Modification of Diet in Renal Disease Study (MDRD) (59 mL/min/1.73 m 2, IQR 43 to 75) and slightly lower with the Cockcroft-Gault (CG) equation (57 mL/min, IQR 39 to 82). Across the commonly used renal function stages, the CKD-EPI and the MDRD classified patients into the same stage in 87.2% (kappa coefficient 0.83, p<0.001); the CKD-EPI and the CG equation agreed in 52.3% (kappa coefficient 0.39, p<0.001). Hence, a differing number of patients will receive dose adjustment depending on which formula is used as cut-off. The CG equation predicted worse prognosis better (c-statistics 0.740, 95% CI 0.734 to 0.746) than CKD-EPI (0.697, 95% CI 0.690 to 0.703, p<0.001) and MDRD (0.680, 95% CI 0.734 to 0.746). Using net reclassification improvement (NRI), the CG identified 12.8% more patients at higher risk of death as compared with the CKD-EPI equation.
Patients registered in the Swedish Heart Failure Registry (n= 40 736) with standardised creatinine values between 2000 and 2012 had their renal function estimated with the CKD-EPI, the MDRD and the CG. Agreement between the formulas was compared for categories. Prediction of death was assessed with c-statistics and with NRI.
Related collections
Most cited references17
- Record: found
- Abstract: found
- Article: not found
Prediction of creatinine clearance from serum creatinine.
- Record: found
- Abstract: found
- Article: not found
Measuring agreement in method comparison studies.
- Record: found
- Abstract: found
- Article: not found