- Record: found
- Abstract: found
- Article: found
Statins use and risk of new-onset diabetes in hypertensive patients: a population-based retrospective cohort study in Yinzhou district, Ningbo city, People’s Republic of China
Abstract
Background
Reports have suggested that statin use is associated with an increased incidence of type 2 diabetes mellitus (T2DM). Guidelines suggested that statins should be prescribed in hypertensive patients for primary prevention. However, there were very few studies on the risk of T2DM associated with statin use among patients with hypertension in mainland People’s Republic of China.
Purpose
To determine the association between statin use and new-onset diabetes mellitus among patients with hypertension in mainland People’s Republic of China.
Patients and methods
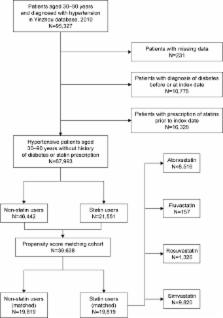
We performed a retrospective cohort study of hypertensive patients using the Yinzhou regional health care database from January 1, 2010, to August 31, 2016. Patients aged 30–90 years old without T2DM were eligible for inclusion. We identified new statin initiators and nonusers by using prescription records of inpatients and outpatients. Multivariate Cox model and propensity score methods were used to adjust potential confounders, including age, sex, body mass index, comorbidities, lifestyle characteristics, and baseline antihypertensive drug use. The risk of incident T2DM among statin initiators compared to nonusers was estimated by the Cox proportional hazards model. Propensity scores for statin use were then developed using logistic regression, statin initiators were matched 1:1 with nonusers according to propensity scores with the nearest neighbor matching method within 0.2 caliper width, and Cox regression was again conducted.
Results
Among 67,993 patients (21,551 statin initiators; 46,442 nonusers), the unadjusted incidence rate of incident T2DM was higher in statin initiators than nonusers (25.68 versus 14.19 events/1,000 person-years; adjusted hazard ratio: 1.55; 95% confidence interval: 1.44–1.66). After propensity score 1:1 matching (19,818 statin initiators; 19,818 nonusers), baseline characteristics between 2 groups were balanced except that the nonusers group was 0.53 years older on average ( P<0.001). Then statin use was still associated with a significant increased risk for T2DM in the matched cohort (adjusted hazard ratio: 1.54; 95% confidence interval: 1.41–1.67). Subgroup analyses also demonstrated similar findings.
Conclusion
Our study indicated an association between statin use and an increased risk of new-onset diabetes mellitus. It provides better understanding of statin and new-onset diabetes mellitus association among hypertensive patients in real-word setting. As an observational study, our findings were prone to unmeasured confounding and bias.
Most cited references24
- Record: found
- Abstract: found
- Article: not found
Diabetes, Hypertension, and Cardiovascular Disease
- Record: found
- Abstract: found
- Article: not found
Survival bias associated with time-to-treatment initiation in drug effectiveness evaluation: a comparison of methods.
- Record: found
- Abstract: found
- Article: not found