- Record: found
- Abstract: found
- Article: found
Vasoplegic syndrome after cardiopulmonary bypass surgery – associated factors and clinical outcomes: a nested case-control study
abstract
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
Introduction
Vasoplegic syndrome (VS) following heart surgery using cardiopulmonary bypass (CPB)
has been recently recognized and implicated in life-threatening complications. The
aim of this study was to identify associated factors for the development of VS after
CPB.
Methods
We performed a nested case–control study of 50 patients undergoing CPB, 27 (54%) men
and 23 (46) women, mean age 66.5 (SD 9.6) years. VS was defined as systemic vascular
resistance index <1,600 dyn∙seg/cm5/m2 and cardiac index >2.5 l/min/m2 within the
first postoperative 4 hours. Vasoplegic shock was defined as vasoplegic patients that
needed norepinephrine for at least 4 hours, after failure to respond to appropriate
volume expansion. Excessive bleeding was defined as blood loss >1 l/24 hours, while
total bleeding was considered as blood loss until chest tube withdrawal. Demographic
variables, surgical procedures and postoperative variables were collected. We recorded
data related to coagulation, fibrinolysis, complement, inflammation, blood loss at
different time points, preoperative, at 0, 4 and 24 hours after surgery, and hemoderivative
requirements. We used the Pearson chi-squared test, the Fisher exact test, the Student
t test and the Mann–Whitney U test for nonparametric variables. SPSS version 12.1
was used.
Results
Seventeen (34%) patients had VS, 11 (65%) men and six (35%) women. Longer aortic clamping
time (P = 0.007) and CPB time (P = 0.013) were associated with VS. These patients
showed a higher cardiac index at 4 hours (P < 0.001) and lactic acid within the first
24 hours. Seven of these patients (41%) fulfilled vasoplegic shock criteria (P < 0.001).
We found higher levels of IL-6 at 0 hours (P = 0.02) and 4 hours (P = 0.001), and
soluble TNF receptor at 0 hours (P = 0.044). At ICU admission (0 hours) there was
a higher coagulation activation: INR (P = 0.005), fibrinogen (P = 0.001), antithrombin
(P = 0.007); lower levels of plasminogen activator inhibitor-1 (P = 0.023) as well
as lower plasminogen activator inhibitor-1/tissue-plasminogen activator ratio (P =
0.021), and higher levels of D-dimer (P = 0.041); lower levels of C3 (P = 0.023),
B factor (P = 0.013), C4 (P = 0.015) as well as a significantly higher decrease between
preoperative and 0-hour levels of C1-inhibitor, C4, C3 and B factor. Lower levels
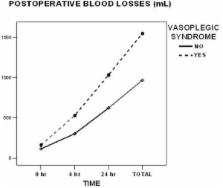
of leptins at 0, 4 and 24 hours were found. Vasoplegic patients showed higher blood
losses along all time points (Figure 1), higher incidence of excessive bleeding (60%
vs 40%; P = 0.011) and required more hemoderivatives during the ICU stay, plasma (P
= 0.016) and platelets (P = 0.002).
Figure 1
Conclusion
VS post-CPB was associated with activation of serin protease systems, which leads
to higher blood loss and excessive bleeding.