- Record: found
- Abstract: found
- Article: found
Characteristics of patients with axial spondyloarthritis by geographic regions: PROOF multicountry observational study baseline results
Read this article at
Abstract
Objectives
To compare demographic and clinical characteristics of patients with axial SpA (axSpA) across geographic regions.
Methods
Patients With Axial Spondyloarthritis: Multicountry Registry of Clinical Characteristics (PROOF) is an observational study that enrolled recently diagnosed (≤1 year) axSpA patients fulfilling the Assessment of SpondyloArthritis international Society classification criteria from rheumatology clinical practices in 29 countries across six geographic regions. Demographics and disease-related parameters were collected. Here we present baseline data for patients who were classified as radiographic axSpA (r-axSpA) or non-radiographic axSpA (nr-axSpA) confirmed by central reading.
Results
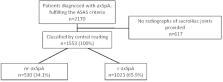
Of the 2170 patients enrolled, 1553 were classified based on central evaluation of sacroiliac radiographs [r-axSpA: 1023 (66%); nr-axSpA: 530 (34%)]. Patients with nr-axSpA had a significantly higher occurrence of enthesitis (40% vs 33%), psoriasis (10% vs 5%) and IBD (4% vs 2%) vs r-axSpA patients. Significant differences in axSpA characteristics were observed between geographic regions. The highest occurrence of peripheral arthritis (60%), enthesitis (52%) and dactylitis (12%) was in Latin America, and the lowest was in Canada (9%, 9% and 2%, respectively). The occurrence of uveitis and psoriasis was highest in Canada (18% and 14%, respectively) and lowest in China (6% and <1%, respectively). IBD was highest in Arabia (21%), and no cases were observed in China. In multivariable analysis adjusted for factors potentially affecting peripheral and extramusculoskeletal manifestations, geographic regions still exhibited significant differences in frequencies of uveitis ( P < 0.01), psoriasis ( P < 0.0001) and peripheral arthritis ( P < 0.0001).
Related collections
Most cited references36
- Record: found
- Abstract: found
- Article: not found
Evaluation of diagnostic criteria for ankylosing spondylitis. A proposal for modification of the New York criteria.
- Record: found
- Abstract: found
- Article: found
2016 update of the ASAS-EULAR management recommendations for axial spondyloarthritis
- Record: found
- Abstract: found
- Article: not found