- Record: found
- Abstract: found
- Article: found
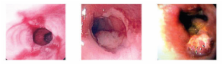
Barrett’s esophagus: Incidence, etiology, pathophysiology, prevention and treatment
Read this article at
Abstract
Barrett’s esophagus is a metaplastic alteration of the normal esophageal epithelium that is detected on endoscopic examination and pathologically confirmed by the presence of intestinal metaplasia on biopsy. Its major significance is as a predisposing factor for esophageal adenocarcinoma, which carries a high mortality rate and a rapidly growing incidence in the United States. Detection of Barrett’s esophagus allows for endoscopic surveillance in order to detect the potential development of dysplasia and early cancer before symptoms develop, and thereby significantly increases treatment options and may lower mortality from esophageal adenocarcinoma. Much current work in the field is aimed at reducing the risk of progression from Barrett’s esophagus to cancer, and in the identification of biomarkers that may predict progression towards cancer. Barrett’s esophagus is present in 10%–20% of patients with gastroesophageal reflux disease (GERD) and has also been detected in patients who deny classic GERD symptoms and are undergoing endoscopy for other indications. We used an evidence-based approach to describe treatment options for patients with Barrett’s esophagus.
Most cited references97
- Record: found
- Abstract: found
- Article: not found
Changing patterns in the incidence of esophageal and gastric carcinoma in the United States.
- Record: found
- Abstract: found
- Article: not found
Symptomatic gastroesophageal reflux as a risk factor for esophageal adenocarcinoma.
- Record: found
- Abstract: found
- Article: not found