- Record: found
- Abstract: found
- Article: found
Release of experimental retinal vein occlusions by direct intraluminal injection of ocriplasmin
Read this article at
Abstract
Purpose
Retinal vein occlusions (RVO) are a major cause of vision loss in people aged 50 years and older. Current therapeutic options limit the consequences of RVO but do not eliminate the cause. Cannulation of the involved vessel and removal of the clot may provide a more permanent solution with a less demanding follow-up. However, cannulation of smaller retinal veins remains challenging. This paper explores the use of ocriplasmin (recombinant plasmin without its kringles) to clear RVO, using a robotic micromanipulator.
Methods
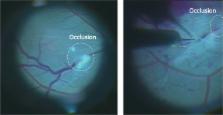
Branch RVO were induced in a porcine model with rose bengal followed by 532 nm endolaser to the superior venous branch of the optic nerve. The vein was cannulated proximal to the occlusion or beyond the first branching vessel from the obstruction. The vein was infused with a physiologic citric acid buffer solution (CAM) or CAM/ocriplasmin. The time of cannulation, number of attempts, and the ability to release the thrombus were recorded.
Results
Cannulation and infusion was possible in all the cases. The use of a micromanipulator allowed for a consistent cannulation of the retinal vein and positional stability allowed the vein to remain cannulated for up to 20 min. In none of the attempts (5/5) with CAM did the thrombus dissolve, despite repeat infusion/relaxation cycles. In 7/7 injections of CAM/ocriplasmin near to the point of obstruction, the clot started to dissolve within a few minutes of injection. An infusion, attempted beyond the first venous branch point proximal to the clot, was unsuccessful in 2/3 attempts.
Related collections
Most cited references14
- Record: found
- Abstract: found
- Article: found
Branch Retinal Vein Occlusion: Pathogenesis, Visual Prognosis, and Treatment Modalities
- Record: found
- Abstract: found
- Article: not found
Endogenous Fibrinolysis: An Important Mediator of Thrombus Formation and Cardiovascular Risk.
- Record: found
- Abstract: found
- Article: not found