- Record: found
- Abstract: found
- Article: found
Teratogenicity of Antiepileptic Drugs
Read this article at
Abstract
Objective
Antiepileptic drugs (AED) have chronic teratogenic effects, the most common of which are congenital heart disease, cleft lip/palate, urogenital and neural tube defects. The aim of our study is to examine teratogenic effects of AED and the correlation between these malformations and AED in single or multiple pregnancies.
Methods
This is a retrospective study of malformations in children born to mothers currently followed up by our outpatient clinics who used or discontinued AED during their pregnancy. Their children were then investigated using echocardiography, urinary ultrasound, cranial magnetic resonance image, and examined by geneticists and pediatric dentists.
Results
One hundred and seventeen children were included in the study. Ninety one of these children were exposed to AED during pregnancy. The most commonly used AED were valproic acid and carbamazepine in monotherapy. The percentage of major anomaly was 6.8% in all children. Dysmorphic features and dental anomalies were observed more in children exposed especially to valproic acid. There were 26 mothers with two and four mothers with three pregnancies from the same fathers. No correlation was found between the distribution of malformations in recurring pregnancies and AED usage.
Conclusion
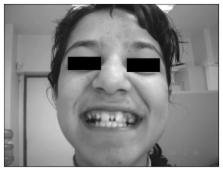
Our study has the highest number of dysmorphism examined in literature, found in all the children exposed to valproic acid, which may account for the higher rate of facial dysmorphism and dental anomalies. On lower doses of valproic acid, major malformations are not seen, although the risk increases with polytherapy. Our data also indicate possible effects of genetic and environmental factors on malformations.
Related collections
Most cited references37
- Record: found
- Abstract: found
- Article: not found
Fetal antiepileptic drug exposure and cognitive outcomes at age 6 years (NEAD study): a prospective observational study.
- Record: found
- Abstract: found
- Article: not found
Dose-dependent risk of malformations with antiepileptic drugs: an analysis of data from the EURAP epilepsy and pregnancy registry.
- Record: found
- Abstract: found
- Article: not found