- Record: found
- Abstract: found
- Article: found
A Comparison of the Effects of Benzalkonium Chloride on Ocular Surfaces between C57BL/6 and BALB/c Mice
Read this article at
Abstract
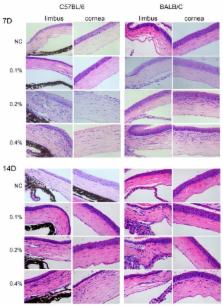
Models of benzalkonium chloride (BAC)-induced ocular disruption have been created and are widely used in various animals. This study aimed to compare the effects of BAC on the ocular surfaces of C57BL/6 and BALB/c mice. C57BL/6 and BALB/c mice were treated separately with BAC eye-drops at different concentrations. Eyes were evaluated by scoring epithelial disruption, corneal opacity and neovascularization in vivo, and by histological assays with hematoxylin/eosin (H/E) and periodic acid-Schiff stainings and by determining the expression of inflammatory factors in vitro on Days 7 and 14. The in vivo corneal epithelial disruption, corneal edema/opacity and neovascularization, which were in accordance with the results of the H/E staining and peaked at Day 7, were observed in a dose-dependent manner in the BAC-treated mice, with more severe signs in the C57BL/6 mice than the BALB/c mice. The loss of conjunctival goblet cells in the conjunctivas and the increasing expression of monocyte chemoattractant protein 1 (MCP-1), growth-regulated protein alpha (GROa) and macrophage inflammatory protein-1 alpha (MIP-1a) in the corneas were found in a dose-dependent manner in both strains of mice. Topical application of BAC can dramatically disrupt the ocular surfaces of C57BL/6 and BALB/c mice, and the disruptions were much more severe in the C57BL/6 mice that received high doses of BAC.
Related collections
Most cited references40
- Record: found
- Abstract: found
- Article: not found
Preservatives in eyedrops: the good, the bad and the ugly.
- Record: found
- Abstract: found
- Article: not found
Conjunctival proinflammatory and proapoptotic effects of latanoprost and preserved and unpreserved timolol: an ex vivo and in vitro study.
- Record: found
- Abstract: found
- Article: not found