- Record: found
- Abstract: found
- Article: found
The accuracy of a handheld “disposable pneumotachograph device” in the spirometric diagnosis of airway obstruction in a Chinese population
Abstract
Background and aim
It is desirable to facilitate the use of an affordable, reliable, and portable spirometer, for earlier diagnosis of COPD in China, particularly in rural areas. The aim of this study was to assess the agreement of a handheld “disposable pneumotachograph” (D-PNEU) spirometer with the gold standard spirometer and to evaluate its diagnostic accuracy of spirometric classification of airflow obstruction.
Subjects and methods
A total of 241 adult Chinese subjects ranging from healthy to those with mixed levels of pulmonary disease performed spirometry in a conventional body plethysmograph, and using a D-PNEU device in randomized order. The three best spirometric tests were recorded for comparative analysis. A Bland–Altman graph was created to assess the agreement between devices. Using FEV 1/FVC <70% as the “gold standard” for obstruction, the accuracy of classifying the severity of airway obstruction for all subjects was assessed. For the specific individuals (n=159) able to exhale for at least 6 seconds, the accuracy of classifying airway obstruction was further assessed. For this purpose, a receiver operating characteristic curve was used to determine an optimal cutoff point of FEV 1/FEV 6 ratio obtained by the D-PNEU device, which matched the global definition of FEV 1/FVC <70% by the traditional spirometer.
Results
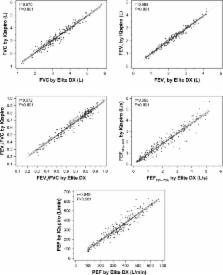
The Bland–Altman analysis showed that the between-device agreement for key airflow metrics was within clinically acceptable limits. The D-PNEU device had 87.1% accuracy in the classification of severity of obstruction in all 241 subjects, when using FEV 1/FVC<70% as the “gold standard” for both devices. The D-PNEU device had 93.7% accuracy in the 159 individuals able to exhale for at least 6 seconds, when a cutoff point of FEV 1/FEV 6 was 74%.
Most cited references20
- Record: found
- Abstract: found
- Article: not found
Statistical methods for assessing agreement between two methods of clinical measurement.
- Record: found
- Abstract: not found
- Article: not found
Tips for learners of evidence-based medicine: 3. Measures of observer variability (kappa statistic).
- Record: found
- Abstract: found
- Article: not found