- Record: found
- Abstract: found
- Article: found
Novel Small Molecule Glucagon-Like Peptide-1 Receptor Agonist Stimulates Insulin Secretion in Rodents and From Human Islets
Read this article at
Abstract
OBJECTIVE
The clinical effectiveness of parenterally-administered glucagon-like peptide-1 (GLP-1) mimetics to improve glucose control in patients suffering from type 2 diabetes strongly supports discovery pursuits aimed at identifying and developing orally active, small molecule GLP-1 receptor agonists. The purpose of these studies was to identify and characterize novel nonpeptide agonists of the GLP-1 receptor.
RESEARCH DESIGN AND METHODS
Screening using cells expressing the GLP-1 receptor and insulin secretion assays with rodent and human islets were used to identify novel molecules. The intravenous glucose tolerance test (IVGTT) and hyperglycemic clamp characterized the insulinotropic effects of compounds in vivo.
RESULTS
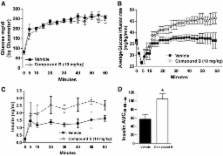
Novel low molecular weight pyrimidine-based compounds that activate the GLP-1 receptor and stimulate glucose-dependent insulin secretion are described. These molecules induce GLP-1 receptor-mediated cAMP signaling in HEK293 cells expressing the GLP-1 receptor and increase insulin secretion from rodent islets in a dose-dependent manner. The compounds activate GLP-1 receptor signaling, both alone or in an additive fashion when combined with the endogenous GLP-1 peptide; however, these agonists do not compete with radiolabeled GLP-1 in receptor-binding assays. In vivo studies using the IVGTT and the hyperglycemic clamp in Sprague Dawley rats demonstrate increased insulin secretion in compound-treated animals. Further, perifusion assays with human islets isolated from a donor with type 2 diabetes show near-normalization of insulin secretion upon compound treatment.
Related collections
Most cited references31

- Record: found
- Abstract: found
- Article: found
Efficacy and Safety Comparison of Liraglutide, Glimepiride, and Placebo, All in Combination With Metformin, in Type 2 Diabetes
- Record: found
- Abstract: found
- Article: not found
Reduced postprandial concentrations of intact biologically active glucagon-like peptide 1 in type 2 diabetic patients.
- Record: found
- Abstract: found
- Article: not found