- Record: found
- Abstract: found
- Article: found
Patient-Centered Care in Psoriatic Arthritis—A Perspective on Inflammation, Disease Activity, and Psychosocial Factors
Read this article at
Abstract
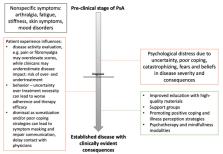
Psoriatic arthritis (PsA) is a seronegative spondyloarthropathy characterized by skin lesions, dactylitis, and enthesitis. Patients with PsA suffer from a variety of psychosocial difficulties and nonspecific symptoms early on in the disease course and continue to experience progressive disease due to delays in diagnosis and treatment. Symptoms initially viewed as somatization could lead to undertreatment and promote psychological distress, poor coping, and negative patient–provider relationships. Pain and fatigue are important complaints that affect the patient’s perception and may need to be addressed with a multidisciplinary approach. Maladaptive cognitive responses can lead to a negative illness perception and impact patient beliefs and concerns over treatment, as well as nonadherence. An underlying inflammatory component in affective disorders has been examined, though whether and how it may interact mechanistically in PsA warrants interest. Cognitive behavioral therapy represents a nonpharmacological treatment modality that can be combined with cytokine-targeted therapy to address both somatic and psychological complaints. Future directions for research include: (1) Elucidating nonspecific manifestations (e.g., subclinical stage, differential with functional syndromes) of PsA and how they impact diagnosis and management; (2) characterizing immune-mediated components of mood disorders in PsA; and (3) whether a bidirectional approach with abrogating inflammation and psychotherapeutic support leads to improved outcomes.
Related collections
Most cited references111
- Record: found
- Abstract: found
- Article: not found
From stress to inflammation and major depressive disorder: a social signal transduction theory of depression.
- Record: found
- Abstract: found
- Article: not found
Cytokines sing the blues: inflammation and the pathogenesis of depression.
- Record: found
- Abstract: not found
- Article: not found