- Record: found
- Abstract: found
- Article: found
Fetal paroxysmal atrial fibrillation during transplacental therapy for supraventricular tachycardia
case-report
Takekazu Miyoshi , MD, PhD
∗
,
†
,
∗ ,
Heima Sakaguchi , MD, PhD
‡ ,
Isao Shiraishi , MD, PhD
‡ ,
Jun Yoshimatsu , MD, PhD
∗ ,
Tomoaki Ikeda , MD, PhD
†
10 October 2018
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
Key Teaching Points
•
Fetal paroxysmal atrial fibrillation (PAF) after transplacental administration of
digoxin for supraventricular tachycardia is rare. Fetuses could tolerate the mild-to-moderate
bradycardia caused by PAF.
•
M-mode recordings are useful for detecting the unique quivering of the atrial wall
specific to fetal PAF.
•
Serial real-time M-mode recordings can complement pulsed wave Doppler echocardiography
in assessing fetal arrhythmias in which atrial contractions are unable to generate
effective cardiac output.
Introduction
Fetal arrhythmias present as an irregular cardiac rhythm and heart rate. Despite the
theoretical advantage of fetoplacental circulation, rapid progression to hydrops is
found in fetuses with tachyarrhythmia due to the limited heart rate reserve.
1
Accurate diagnosis is essential for appropriate management of fetal arrhythmias. Fetal
cardiac rhythm and heart rate are assessed by using M-mode and pulsed wave Doppler
echocardiography.
2
A recent scientific statement from the American Heart Association has recommended
the antiarrhythmic treatment of fetal supraventricular tachyarrhythmia (SVT) when
it is sustained ≥ 50% of time monitored and/or is accompanied by fetal hydrops or
ventricular dysfunction.
3
For fetal SVT, which is the most common type of tachyarrhythmia, maternal administration
of digoxin, sotalol, or flecainide is used in many centers.
3
In our institution, digoxin is used as the first-choice therapy for SVT without fetal
hydrops because of its relatively safe profile, its long history of use during pregnancy,
and the familiarity with its use.
Atrial fibrillation is the most common arrhythmia in adults and is associated with
an increased risk of mortality and morbidity.
4
However, it has rarely been noted in fetuses.5, 6, 7 We describe a rare case of paroxysmal
atrial fibrillation (PAF) after transplacental administration of digoxin for fetal
SVT.
Case report
A 31-year-old woman, gravida 2, para 1, was referred to our institution at 30 weeks
of gestation for fetal tachycardia. She had no complications and took no medications.
Fetal echocardiographic evaluation revealed a structurally normal heart, but moderate
tricuspid regurgitation and ascites were observed (Voluson E8 ultrasound equipment,
GE Medical Systems, Zipf, Austria). Cardiothoracic area ratio of 33%, reversed ductus
venosus flow, and pulsatile flow in the umbilical vein were also found. Fetal arrhythmias
were assessed using fetal echocardiography and cardiotocography. Doppler recordings
of superior vena cava (SVC)–ascending aorta (aAo) flows showed incessant short ventriculoatrial
(VA) SVT (Figure 1A). M-mode recordings showed 1:1 atrioventricular (AV) conduction
with a ventricular rate of 215 beats per minute (bpm) (Figure 1B). The fetal baseline
heart rate was not constant, fluctuating between 210 and 220 bpm on cardiotocography
(Figure 1C).
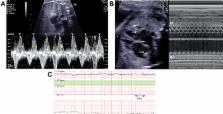
Figure 1
Supraventricular tachyarrhythmia (SVT). Sustained SVT was confirmed by Doppler and
M-mode recordings at 30 weeks of gestation. A: Doppler recording of superior vena
cava (SVC)–ascending aorta (aAo) flow showed short ventriculoatrial (VA) tachycardia
(VA/atrioventricular [AV] ratio = 0.44) with a ventricular rate of 215 beats per minute
(bpm). B: M-mode recording using a 4-chamber view showed 1:1 AV conduction with a
ventricular rate of 215 bpm. C: Fetal baseline heart rate varied between 210 and 220
bpm on cardiotocography. A indicates the retrograde A wave in the SVC corresponding
to atrial contraction. V indicates the aortic ejection wave (V wave). LV = left ventricle;
RA = right atrium.
After the transplacental administration of oral digoxin (0.75 mg/day), the maternal
serum digoxin level increased to 0.9 ng/mL. Subsequently, the incidence of fetal tachyarrhythmia
gradually decreased to less than 50% during monitoring, and there was no evidence
of progression of fetal hydrops or ventricular dysfunction. Irregular bradycardia
was intermittently detected by Doppler recording of SVC–aAo flow (Figure 2A). M-mode
recording also showed irregular bradycardia; AV dissociation was present, with a ventricular
rate of 70–90 bpm and an atrial rate of 40–50 bpm (Figure 2B). Detailed observation
during M-mode recording showed the unique quivering of the atrial wall subsequent
to a clear atrial contraction, suggesting PAF. Serial recordings using fetal echocardiography
detected the transition between PAF and SVT (Supplemental Videos 1–3). The fetal baseline
heart rate intermittently fluctuated between 70 and 215 bpm on cardiotocography (Figure 2C).
On the 10th day after the transplacental administration of digoxin, complete cardioversion
to sinus rhythm with a ventricular rate of 140 bpm was achieved, and fetal ascites
resolved. Transplacental administration of digoxin was continued until delivery. A
female infant weighing 2989 g was delivered at 38 weeks of gestation. The newborn’s
1- and 5-minute Apgar scores were 9 and 9, respectively, and her umbilical artery
blood pH was 7.29. Basal electrocardiography at birth showed 120 bpm with sinus rhythm.
No recurrence of arrhythmia was found after birth.
Figure 2
Paroxysmal atrial fibrillation (PAF). PAF was confirmed by M-mode recording at 30
weeks of gestation. A: Doppler recording of superior vena cava (SVC)–ascending aorta
(aAo) flow showed irregular bradycardia with a ventricular rate of 70–90 beats per
minute (bpm). The A wave frequently disappeared. B: M-mode recording using a 4-chamber
view also showed irregular bradycardia. Atrioventricular dissociation was present,
with a ventricular rate of 70–90 bpm and an atrial rate of 40–50 bpm. After a clear
atrial contraction, the unique quivering of the atrial wall (*) was observed, suggesting
PAF. C: Fetal baseline heart rate intermittently fluctuated between 70 and 215 bpm
on cardiotocography. LV = left ventricle; RA = right atrium.
Discussion
Pulsed wave Doppler echocardiography has become the standard tool for the diagnosis
of fetal arrhythmias.8, 9 Simultaneous pulsed wave Doppler evaluation of SVC–aAo flow
is used to examine the sequence and temporal relationship of blood flow events secondary
to atrial and ventricular contractions.
10
Atrial contraction (the retrograde A wave in the SVC) is the mechanical consequence
of atrial depolarization, whereas the aortic ejection wave (V wave) is the mechanical
consequence of the QRS complex. The diagnosis of fetal arrhythmias is made based on
the relationship between the A and V waves. Although fetal echocardiography is a mechanical
rather than electrical assessment, serial Doppler echocardiography recordings are
comparable to fetal magnetocardiography for the prenatal diagnosis of arrhythmias.
11
Furthermore, the Doppler approach provides functional assessment, which can help guide
management. Chao and colleagues
5
used pulsed wave Doppler and M-mode recordings to demonstrate atrial fibrillation
manifesting as irregular atrial and ventricular contractions. Ventricular contraction
occurs after maternal digitalization, allowing for the identification of rapid fibrillation
waves after AV valve motion by Doppler echocardiography. Since digoxin depresses AV
nodal conduction and prolongs the AV nodal refractory period, it might make the dyssynchrony
between atrial and ventricular contraction more obvious. In our case, however, retrograde
A and SVC waves during PAF were difficult to detect by pulsed wave Doppler echocardiography,
because the atrial contractions associated with PAF did not result in effective cardiac
output. In contrast, serial real-time M-mode recordings demonstrated the unique quivering
of the atrial wall, which reflects the ineffective atrial contractions of PAF.
Since in adult cardiology digoxin is usually used to achieve rate control in patients
with atrial fibrillation, it is unclear whether digoxin could induce fetal atrial
fibrillation. To our knowledge, there are no reports of fetal atrial fibrillation
occurring with other antiarrhythmic agents such as flecainide and sotalol. There are
cases in which fetal SVT and atrial flutter or fibrillation coexist. Thus, we speculate
that treating SVT with digoxin might have resulted in latent atrial fibrillation.
Incessant fetal tachyarrhythmias are associated with a high incidence of fetal hydrops,
a preterminal manifestation of cardiovascular decompensation.
1
Pulsed wave Doppler analysis of ventricular diastolic filling in fetuses suggests
that the myocardium is stiffer than during childhood and adulthood.
12
Thus, the fetal heart behaves like an older heart with little cardiac reserve. In
this case, fetal ascites developed owing to elevation of right atrial pressure during
incessant SVT, whereas it gradually resolved when the ventricular rate fell to 70–90
bpm during PAF. This indicates that mild-to-moderate bradycardia was able to maintain
fetal circulation. However, since hemodynamics are unstable, especially in fetuses
with SVT and hydrops, serial assessments including ventricular valve regurgitation,
effusion, and venous Doppler findings are required.
Conclusion
We described a rare case of PAF after transplacental administration of digoxin for
fetal SVT. Fetuses could tolerate the mild-to-moderate bradycardia caused by PAF.
M-mode recordings were useful for detecting the unique quivering of the atrial wall
specific to PAF. Thus, serial real-time M-mode recordings can complement pulsed wave
Doppler echocardiography in assessing fetal arrhythmias in which atrial contractions
are unable to generate effective cardiac output.
Related collections
Most cited references11
- Record: found
- Abstract: not found
- Article: not found
Rhythm abnormalities of the fetus.
Lisa Hornberger, David Sahn (2007)
- Record: found
- Abstract: found
- Article: not found
Fetal tachycardia: mechanisms and predictors of hydrops fetalis.
Zahra J. Naheed, Janette Strasburger, Barbara Deal … (1996)
- Record: found
- Abstract: found
- Article: not found
Atrial flutter: Clinical risk factors and adverse outcomes in the Framingham Heart Study.
Faisal Rahman, Na Wang, Xiaoyan Yin … (2016)