- Record: found
- Abstract: found
- Article: not found
Evaluation of renal nerve morphological changes and norepinephrine levels following treatment with novel bipolar radiofrequency delivery systems in a porcine model
Read this article at
Abstract
Objective:
To evaluate the safety and effectiveness of different bipolar radiofrequency system algorithms in interrupting the renal sympathetic nerves and reducing renal norepinephrine in a healthy porcine model.
Methods:
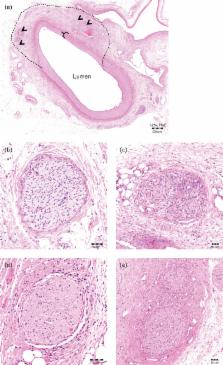
A porcine model ( N = 46) was used to investigate renal norepinephrine levels and changes to renal artery tissues and nerves following percutaneous renal denervation with radiofrequency bipolar electrodes mounted on a balloon catheter. Parameters of the radiofrequency system (i.e. electrode length and energy delivery algorithm), and the effects of single and longitudinal treatments along the artery were studied with a 7-day model in which swine received unilateral radiofrequency treatments. Additional sets of animals were used to examine norepinephrine and histological changes 28 days following bilateral percutaneous radiofrequency treatment or surgical denervation; untreated swine were used for comparison of renal norepinephrine levels.
Results:
Seven days postprocedure, norepinephrine concentrations decreased proportionally to electrode length, with 81, 60 and 38% reductions (vs. contralateral control) using 16, 4 and 2-mm electrodes, respectively. Applying a temperature-control algorithm with the 4-mm electrodes increased efficacy, with a mean 89.5% norepinephrine reduction following a 30-s treatment at 68°C. Applying this treatment along the entire artery length affected more nerves vs. a single treatment, resulting in superior norepinephrine reduction 28 days following bilateral treatment.
Related collections
Most cited references10
- Record: found
- Abstract: found
- Article: not found
Catheter-based renal sympathetic denervation for resistant hypertension: a multicentre safety and proof-of-principle cohort study.
- Record: found
- Abstract: found
- Article: not found
Sympathetic augmentation in hypertension: role of nerve firing, norepinephrine reuptake, and Angiotensin neuromodulation.
- Record: found
- Abstract: found
- Article: not found
