- Record: found
- Abstract: found
- Article: found
Cerebellar resting-state functional connectivity in Parkinson's disease and multiple system atrophy: Characterization of abnormalities and potential for differential diagnosis at the single-patient level
Read this article at
Abstract
Background
Recent studies using resting-state functional connectivity and machine-learning to distinguish patients with neurodegenerative diseases from other groups of subjects show promising results. This approach has not been tested to discriminate between Parkinson's disease (PD) and multiple system atrophy (MSA) patients.
Objectives
Our first aim is to characterize possible abnormalities in resting-state functional connectivity between the cerebellum and a set of intrinsic-connectivity brain networks and between the cerebellum and different regions of the striatum in PD and MSA. The second objective of this study is to assess the potential of cerebellar connectivity measures to distinguish between PD and MSA patients at the single-patient level.
Methods
Fifty-nine healthy controls, 62 PD patients, and 30 MSA patients underwent resting-state functional MRI with a 3T scanner. Independent component analysis and dual regression were used to define seven resting-state networks of interest. To assess striatal connectivity, a seed-to-voxel approach was used after dividing the striatum into six regions bilaterally. Measures of cerebellar-brain network and cerebellar-striatal connectivity were then used as features in a support vector machine to discriminate between PD and MSA patients.
Results
MSA patients displayed reduced cerebellar connectivity with different brain networks and with the striatum compared with PD patients and with controls. The classification procedure achieved an overall accuracy of 77.17% with 83.33% of the MSA subjects and 74.19% of the PD patients correctly classified.
Highlights
-
•
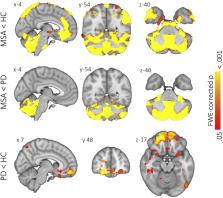
Reduced cerebellar functional connectivity in MSA compared with healthy controls.
-
•
Reduced cerebellar-striatal functional connectivity in MSA compared with PD.
-
•
Reduced connectivity between cerebellum and brain networks in MSA compared with PD.
-
•
Cerebellar connectivity might help discriminate between MSA and PD patients.
Related collections
Most cited references44
- Record: found
- Abstract: found
- Article: not found
The accuracy of diagnosis of parkinsonian syndromes in a specialist movement disorder service.
- Record: found
- Abstract: found
- Article: not found
The cerebellum and cognition
- Record: found
- Abstract: found
- Article: not found