- Record: found
- Abstract: found
- Article: found
The role of neuroinflammation on pathogenesis of affective disorders
Read this article at
Abstract
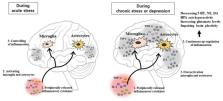
Accumulating evidence suggests that neuroinflammation plays an important role in etiology of psychiatric disorders. Neuronflammation involves a combination of psychological, neuroendocrine, and nervous systems resulting in changes of neurotransmitter metabolism, dysregulation of the hypothalamuspituitary-adrenal axis, pathologic microglial cell activation, impaired neuroplasticity, and structural and functional brain changes affecting cognition and emotional behavior. Inflammatory cytokines have been postulated to be the possible link and culprit in the disruption of these systems. The outcome of any type of dysregulation of the immune system in the brain might lead to occurrence of depression, anxiety. This review focuses on the possible impact of dysregulated cytokine networks which may cause pathogenesis of affective disorders such as depression and anxiety.
Related collections
Most cited references51
- Record: found
- Abstract: found
- Article: not found
The role of inflammation in depression: from evolutionary imperative to modern treatment target.
- Record: found
- Abstract: found
- Article: not found
Cytokines and major depression.
- Record: found
- Abstract: found
- Article: not found
