- Record: found
- Abstract: found
- Article: found
Awareness of Cognitive Decline in Patients With Alzheimer's Disease: A Systematic Review and Meta-Analysis
Read this article at
Abstract
Background: Identifying a poor degree of awareness of cognitive decline (ACD) could represent an early indicator of Alzheimer's disease (AD).
Objectives: (1) to understand whether there is evidence of poor ACD in the pre-dementia stages of AD; (2) to summarize the main findings obtained investigating ACD in AD; (3) to propose a conceptual framework.
Data Sources: We searched Scopus, Pubmed, and the reference lists for studies published up to August 2020. Original research articles must report a measure of ACD and included individuals with AD dementia, or prodromal AD (or MCI), or being at risk for AD.
Data Synthesis: All studies covering preclinical, prodromal, and AD dementia were systematically reviewed. We intended to perform a meta-analysis of empirical studies on preclinical AD or prodromal AD (or MCI), to compare ACD between clinical groups. Due to the paucity of literature on preclinical AD, meta-analysis was only possible for prodromal AD (or MCI) studies.
Results: We systematically reviewed 283 articles, and conducted a meta-analysis of 18 articles on prodromal AD (or MCI), showing that ACD was not significantly different between patients with amnestic and non-amnestic MCI (SMD = 0.09, p = 0.574); ACD was significantly poorer in amnestic MCI (SMD = −0.56, p = 0.001) and mild AD (SMD = −1.39, p < 0.001) than in controls; ACD was also significantly poorer in mild AD than in amnestic MCI (SMD = −0.75, p < 0.001), as well as poorer than in non-amnestic MCI (SMD = −1.00, p < 0.001). We also discuss key findings on ACD in AD, such as its neural and cognitive correlates.
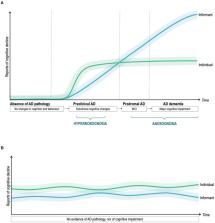
Conclusions and Implications: We propose that patients may be complaining of their initial subtle cognitive changes, but ACD would soon start to decrease. The individual would show mild anosognosia in the MCI stage, and severe anosognosia in dementia. The evaluation of ACD (comparing self-report to cognitive scores or to informant-report) could be useful to guide the clinician toward a timely diagnosis, and in trials targeting early-stage AD.
Related collections
Most cited references115

- Record: found
- Abstract: found
- Article: found
NIA-AA Research Framework: Toward a biological definition of Alzheimer’s disease
- Record: found
- Abstract: found
- Article: not found
A conceptual framework for research on subjective cognitive decline in preclinical Alzheimer's disease
- Record: found
- Abstract: found
- Article: found