- Record: found
- Abstract: found
- Article: found
Yam Daabo interventions’ effects on postpartum family planning use in Burkina Faso at 24 months after childbirth
Read this article at
Abstract
Introduction
After testing the interventions for improving the prevalence of contraceptive use, very few studies have measured the long-term effects thereafter the end of the implementation. This study aimed to measure Yam Daabo interventions’ effects on contraceptive use in Burkina Faso at twelve months after completion of the intervention.
Methods
Yam Daabo was a two-group, multi-intervention, single-blind, cluster randomized controlled trial. Interventions comprised refresher training for the provider, a counseling tool, supportive supervision, availability of contraceptive services 7 days a week, client appointment cards, and invitation letters for partners. We used generalized linear mixed-effects models (log Poisson) to compare the modern contraceptive prevalence at 12 months post-intervention in the two groups. We collected data between September and November 2018. We conducted an intention-to-treat analysis and adjusted the prevalence ratios on cluster effects and unbalanced baseline characteristics.
Results
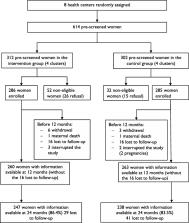
Twelve months after the completion of the Yam Daabo trial, we interviewed 87.4% (485 out of 555 women with available data at 12 months, that is, 247/276 in the intervention group (89.5%) and 238/279 in the control group (85.3%). No difference was observed in the use of hormonal contraceptive methods between the intervention and control groups (adjusted prevalence ratio = 1.21; 95% confidence interval [CI] = [0.91–1.61], p = 0.191). By contrast, women in the intervention group were more likely to use long-acting reversible contraceptives (LARC) than those in the control group (adjusted prevalence ratio = 1.35; 95% CI = [1.08–1.69], p = 0.008).
Conclusion
Twelve months after completion of the intervention, we found no significant difference in hormonal contraceptive use between women in the intervention and their control group counterparts. However, women in the intervention group were significantly more likely to use long-acting reversible contraceptives than those in the control group.
Trial registration
The trial registration number at the Pan African Clinical Trials Registry is PACTR201609001784334. The date of the first registration is 27/09/2016.
Related collections
Most cited references14

- Record: found
- Abstract: found
- Article: found
Trends in contraceptive prevalence rates in sub-Saharan Africa since the 2012 London Summit on Family Planning: results from repeated cross-sectional surveys
- Record: found
- Abstract: found
- Article: not found
Interventions to Improve Postpartum Family Planning in Low- and Middle-Income Countries: Program Implications and Research Priorities.

- Record: found
- Abstract: found
- Article: found