- Record: found
- Abstract: found
- Article: not found
Endothelial cell infection and endotheliitis in COVID-19
letter
Zsuzsanna Varga
a ,
Andreas J Flammer
b ,
Peter Steiger
c ,
Martina Haberecker
a ,
Rea Andermatt
c ,
Annelies S Zinkernagel
d ,
Mandeep R Mehra
e ,
Reto A Schuepbach
c ,
Frank Ruschitzka
b ,
Holger Moch
a
21 April 2020
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
Cardiovascular complications are rapidly emerging as a key threat in coronavirus disease
2019 (COVID-19) in addition to respiratory disease. The mechanisms underlying the
disproportionate effect of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2)
infection on patients with cardiovascular comorbidities, however, remain incompletely
understood.1, 2
SARS-CoV-2 infects the host using the angiotensin converting enzyme 2 (ACE2) receptor,
which is expressed in several organs, including the lung, heart, kidney, and intestine.
ACE2 receptors are also expressed by endothelial cells.
3
Whether vascular derangements in COVID-19 are due to endothelial cell involvement
by the virus is currently unknown. Intriguingly, SARS-CoV-2 can directly infect engineered
human blood vessel organoids in vitro.
4
Here we demonstrate endothelial cell involvement across vascular beds of different
organs in a series of patients with COVID-19 (further case details are provided in
the appendix).
Patient 1 was a male renal transplant recipient, aged 71 years, with coronary artery
disease and arterial hypertension. The patient's condition deteriorated following
COVID-19 diagnosis, and he required mechanical ventilation. Multisystem organ failure
occurred, and the patient died on day 8.
Post-mortem analysis of the transplanted kidney by electron microscopy revealed viral
inclusion structures in endothelial cells (figure A, B
). In histological analyses, we found an accumulation of inflammatory cells associated
with endothelium, as well as apoptotic bodies, in the heart, the small bowel (figure
C) and lung (figure D). An accumulation of mononuclear cells was found in the lung,
and most small lung vessels appeared congested.
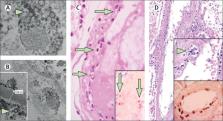
Figure
Pathology of endothelial cell dysfunction in COVID-19
(A, B) Electron microscopy of kidney tissue shows viral inclusion bodies in a peritubular
space and viral particles in endothelial cells of the glomerular capillary loops.
Aggregates of viral particles (arrow) appear with dense circular surface and lucid
centre. The asterisk in panel B marks peritubular space consistent with capillary
containing viral particles. The inset in panel B shows the glomerular basement membrane
with endothelial cell and a viral particle (arrow; about 150 nm in diameter). (C)
Small bowel resection specimen of patient 3, stained with haematoxylin and eosin.
Arrows point to dominant mononuclear cell infiltrates within the intima along the
lumen of many vessels. The inset of panel C shows an immunohistochemical staining
of caspase 3 in small bowel specimens from serial section of tissue described in panel
D. Staining patterns were consistent with apoptosis of endothelial cells and mononuclear
cells observed in the haematoxylin-eosin-stained sections, indicating that apoptosis
is induced in a substantial proportion of these cells. (D) Post-mortem lung specimen
stained with haematoxylin and eosin showed thickened lung septa, including a large
arterial vessel with mononuclear and neutrophilic infiltration (arrow in upper inset).
The lower inset shows an immunohistochemical staining of caspase 3 on the same lung
specimen; these staining patterns were consistent with apoptosis of endothelial cells
and mononuclear cells observed in the haematoxylin-eosin-stained sections. COVID-19=coronavirus
disease 2019.
Patient 2 was a woman, aged 58 years, with diabetes, arterial hypertension, and obesity.
She developed progressive respiratory failure due to COVID-19 and subsequently developed
multi-organ failure and needed renal replacement therapy. On day 16, mesenteric ischaemia
prompted removal of necrotic small intestine. Circulatory failure occurred in the
setting of right heart failure consequent to an ST-segment elevation myocardial infarction,
and cardiac arrest resulted in death. Post-mortem histology revealed lymphocytic endotheliitis
in lung, heart, kidney, and liver as well as liver cell necrosis. We found histological
evidence of myocardial infarction but no sign of lymphocytic myocarditis. Histology
of the small intestine showed endotheliitis (endothelialitis) of the submucosal vessels.
Patient 3 was a man, aged 69 years, with hypertension who developed respiratory failure
as a result of COVID-19 and required mechanical ventilation. Echocardiography showed
reduced left ventricular ejection fraction. Circulatory collapse ensued with mesenteric
ischaemia, and small intestine resection was performed, but the patient survived.
Histology of the small intestine resection revealed prominent endotheliitis of the
submucosal vessels and apoptotic bodies (figure C).
We found evidence of direct viral infection of the endothelial cell and diffuse endothelial
inflammation. Although the virus uses ACE2 receptor expressed by pneumocytes in the
epithelial alveolar lining to infect the host, thereby causing lung injury, the ACE2
receptor is also widely expressed on endothelial cells, which traverse multiple organs.
3
Recruitment of immune cells, either by direct viral infection of the endothelium or
immune-mediated, can result in widespread endothelial dysfunction associated with
apoptosis (figure D).
The vascular endothelium is an active paracrine, endocrine, and autocrine organ that
is indispensable for the regulation of vascular tone and the maintenance of vascular
homoeostasis.
5
Endothelial dysfunction is a principal determinant of microvascular dysfunction by
shifting the vascular equilibrium towards more vasoconstriction with subsequent organ
ischaemia, inflammation with associated tissue oedema, and a pro-coagulant state.
6
Our findings show the presence of viral elements within endothelial cells and an accumulation
of inflammatory cells, with evidence of endothelial and inflammatory cell death. These
findings suggest that SARS-CoV-2 infection facilitates the induction of endotheliitis
in several organs as a direct consequence of viral involvement (as noted with presence
of viral bodies) and of the host inflammatory response. In addition, induction of
apoptosis and pyroptosis might have an important role in endothelial cell injury in
patients with COVID-19. COVID-19-endotheliitis could explain the systemic impaired
microcirculatory function in different vascular beds and their clinical sequelae in
patients with COVID-19. This hypothesis provides a rationale for therapies to stabilise
the endothelium while tackling viral replication, particularly with anti-inflammatory
anti-cytokine drugs, ACE inhibitors, and statins.7, 8, 9, 10, 11 This strategy could
be particularly relevant for vulnerable patients with pre-existing endothelial dysfunction,
which is associated with male sex, smoking, hypertension, diabetes, obesity, and established
cardiovascular disease, all of which are associated with adverse outcomes in COVID-19.
Related collections
Most cited references7
- Record: found
- Abstract: found
- Article: not found
Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study
Fei Zhou, Ting Yu, Ronghui Du … (2020)
- Record: found
- Abstract: found
- Article: not found
Inhibition of SARS-CoV-2 Infections in Engineered Human Tissues Using Clinical-Grade Soluble Human ACE2
Vanessa Monteil, Hyesoo Kwon, Patricia Prado … (2020)
- Record: found
- Abstract: found
- Article: not found
Trials of anti-tumour necrosis factor therapy for COVID-19 are urgently needed
Marc Feldmann, Ravinder Maini, James N. Woody … (2020)
