- Record: found
- Abstract: found
- Article: found
Personalized needle modification for CT-guided percutaneous infrazygomatic radiofrequency ablation of the maxillary nerve through the foramen rotundum in order to treat V2 trigeminal neuralgia
Abstract
Background: The computed tomography (CT)-guided radiofrequency ablation (RFA) of the maxillary nerve (V2) via foramen rotundum (FR) approach has been reported to offer the highest rates of pain relief in V2 trigeminal neuralgia (TN). However, the access to FR may be obstructed by the greater wing of the sphenoid bone.
Objectives: We report on an optimized CT-guided percutaneous infrazygomatic of maxillary nerve through the foramen rotundum (FR) to treat V2 trigeminal neuralgia (TN) using personalized RFA needles based on patient’s individual CT-image parameters.
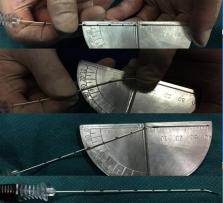
Patients and methods: 176 patients with isolated V2 TN were included. If the entry of the percutaneous needle into the FR canal was blocked by the greater wing of the sphenoid bone, straight RFA needles was bent at the tip with an angle α (the angle between the straight line from the external opening of FR to the skin entry point and the long axis of the FR canal). The maxillary nerve RFA was performed after confirmation with electrophysiological tests. Pain relief in the V2 territory and TN recurrence rate were followed for up to 60 months.
Results: Fifty-two patients (29.55%) required needle bending. The maxillary nerve thermal RFA resulted in analgesia in the V2 territory without affecting the V1 or V3 zone. TN recurrence rate at 6, 12, 24, 36, 48 and 60 months was 2.55%, 7.64%, 17.20%, 24.41%, 30.28% and 33.77%, respectively.
Conclusion: The personalized needle modification technique for maxillary nerve RFA through FR is safe and effective to treat V2 TN.
Most cited references26
- Record: found
- Abstract: found
- Article: not found
Percutaneous controlled radiofrequency trigeminal rhizotomy for the treatment of idiopathic trigeminal neuralgia: 25-year experience with 1,600 patients.
- Record: found
- Abstract: found
- Article: not found
Systematic review of ablative neurosurgical techniques for the treatment of trigeminal neuralgia.
- Record: found
- Abstract: found
- Article: not found