- Record: found
- Abstract: found
- Article: found
The 5th Shanghai Gynecologic Oncology Group (SGOG)-Korean Gynecologic Oncology Group (KGOG) joint meeting and 2016 Asia-Pacific Ovarian cancer Laparotomy and Laparoscopic Operation (APOLLO) symposium in Shanghai
meeting-report
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
On June 18, 2016, the 5th Shanghai Gynecologic Oncology Group (SGOG)-Korean Gynecologic
Oncology Group (KGOG) Joint Meeting was held in Zhongshan Hospital, Fudan University,
Shanghai, China. Rongyu Zang (chairman of SGOG, KGOG-SGOG coordinator) from Zhongshan
Hospital, Fudan University hosted this meeting. Total 21 KGOG members including Byoung-Gie
Kim (president of KGOG, SGOG-KGOG coordinator), Yong-Man Kim (vice president of KGOG),
Jae-Weon Kim (chair of ovarian-fallopian tube tumor site committee of KGOG, SGOG-KGOG
coordinator), and Taek Sang Lee (secretary general of KGOG) attended the 5th joint
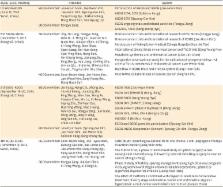
meeting. Eight young fellows were included in 21 KGOG attendees (Table 1, Fig. 1).
HISTORY OF SGOG-KGOG JOINT MEETINGS
To briefly look over the history of KGOG-SGOG joint meeting, the first KGOG-SGOG meeting
was held in Seoul on June 13, 2012, during the 10th Asian Clinical Oncology Society
(ACOS) meeting. The first joint meeting was chaired by Joo-Hyun Nam the prior president
of KGOG, and Rongyu Zang who represented SGOG. The second and third joint meetings
were held in Shanghai on December 8, 2012 and September 18 to 19, 2014. The fourth
meeting was held in Seoul, Korea together with the 4th biennial meeting of Asian Society
of Gynecologic Oncology (ASGO) on November 12, 2015 (Table 2, Fig. 2).
THE 5TH SGOG-KGOG JOINT MEETING
The aims of the 5th SGOG-KGOG Joint Meeting which comprised morning and afternoon
sessions were to introduce and discuss important issues on the study of upfront surgery
versus neoadjuvant chemotherapy (NACT) followed by interval debulking surgery for
patients with International Federation of Gynecology and Obstetrics (FIGO) stage IIIC
and IV ovarian cancer (SUNNY) trial and to promote friendship among young doctors
from SGOG and KGOG. An impressive opening ceremony co-chaired by Rongyu Zang, a principal
investigator of the SUNNY trial in the Asian quarter, and Byoung-Gie Kim, was followed
by scientific program (Table 1).
In the morning session, four speakers (two of each from SGOG and KGOG, respectively)
introduced interesting studies. Firstly, Rong Jiang from the SGOG young doctor group
introduced the SUNNY trial.
Epithelial ovarian cancer (EOC) is the most lethal gynecologic cancer. Although optimal
surgical cytoreduction with no residual tumor is associated with better survival outcomes,
it is often difficult to perform because most EOC is diagnosed at advanced stage with
extensive peritoneal seeding. NACT has been suggested as an option for feasibility
of optimal cytoreduction. NACT can decrease the tumor burden, so that subsequent complete
cytoreduction is more achievable than upfront surgery. Moreover, NACT may improve
performance status, shorten the operation time, spare as much crucial intraperitoneal
organs as possible, and therefore minimize perioperative morbidity and mortality.
Recently, two randomized controlled trials, the European Organisation for Research
and Treatment of Cancer (EORTC) 55971 and Chemotherapy or Upfront surgery (CHORUS)
studies, have reported that NACT followed by IDS is not inferior to primary debulking
surgery (PDS) in the management of patients with stages IIIC and IV EOC. However,
several issues were raised in the studies comparing PDS with NACT plus IDS. These
two studies were conducted in a setting of limited maximal surgical effort, as evidenced
by low rates of optimal cytoreduction and no gross tumor clearance. To investigate
the role of NACT in the treatment of advanced EOC, a well-designed prospective randomized
phase III clinical trial in specialized centers with experience in maximal surgical
effort is needed. And the SUNNY trial aimed to evaluate whether PDS can improve overall
survival (OS) compared with NACT followed by IDS.
Active discussions happened as follows. Michael Bookman, chair of the ovarian committee
of NRG Oncology, recommended core needle biopsy instead of cytology in the inclusion
criteria of the SUNNY trial. He suggested that it would be better to exclude low-grade
serous adenocarcinoma by using p53 immunohistochemistry and noted that a laparoscopic
biopsy tended to be followed by unnecessary operative procedures. However, Prof. Zang
indicated that laparoscopic biopsy could be useful in finding out that the ovarian
tumor was not a primary tumor but metastasis of another cancer such as stomach cancer.
And he, therefore, argued that laparoscopic biopsy rather than cytology is appropriate
for diagnosis. Jae-Weon Kim, the Korean principal investigator in the SUNNY trial,
offered to include Asian countries other than Korea and China, such as Japan and Taiwan,
because SUNNY is intended to be an Asian trial. Furthermore, he said that some members
of Japan Gynecologic Oncology Group (JGOG) were interested in participating in the
SUNNY trial.
Second, Ha Kyun Chang proposed an ancillary study to the SUNNY trial. He suggested
that preoperative positron emission tomography-computed tomography (PET-CT) could
be used in predicting the clinical response to NACT in advanced-stage EOC. Using two
PET-CT images of before and after the 1st cycle of NACT, the change in standardized
uptake value (SUV) is assessed. Using tissues obtained at two time points, diagnostic
laparoscopy before the 1st cycle of NACT and IDS after the 3rd cycle of NACT, chemotherapy
response score as a pathologic parameter is decided through review of two paired slides
by pathologists. Correlation between SUV change, chemotherapy response score, and
survival is evaluated. Primary objective is to determine changes in tumor functional
parameters such as SUV, total lesion glycolysis, and metabolic tumor volume. Secondary
objectives include determining whether changes in tumor metabolism from sequential
PET-CT are prognostic of survival in NACT arms. By adding functional imaging to the
master treatment study, there is potential to identify the quantitative functional
parameters of PET-CT that are early predictors of the patient response to therapy
and survival in ovarian cancer. If changes in tumor metabolism after the 1st cycle
of conventional NACT (paclitaxel and carboplatin) are not satisfactory, it may well
be replaced by other strategies such as different regimen of NACT or immediate surgery.
Michael Bookman pointed out that this idea was interesting, but that conducting PET-CT
in only one arm could affect the results of the main study. Thus, PET-CT should be
performed in all groups. Prof. Zang also said that it would be a good idea to conduct
a subgroup study of the SUNNY trial; after a few modifications of the scheme, a subgroup
study could be set up.
Third, Xiaojun Chen, KGOG-SGOG coordinator, presented her study results which immunohistochemically
evaluated the expression of blood and tissue markers predicting lymph node metastasis
in endometrial cancer. In 370 endometrioid endometrial cancer patients undergoing
comprehensive surgical staging, a prediction model which could identify patients with
a low-risk of lymph node metastasis was created. In this model, both serum tumor marker,
cancer antigen 125 (CA-125), and tissue markers including estrogen receptor, progesterone
receptor (PR), Ki67, and p53 were used. The low-risk group could be characterized
as serum CA-125 <30.0 IU/mL and a tumor with either or both positive PR staining >50%
and Ki67 <40%. Byoung-Gie Kim had a comment on the necessity of central review of
immunohistochemical staining results because the results were quite variable between
the readers. He also argued that the extent of lymph node dissection should be considered
if there was recurrence at lymph nodes during follow-up. In line with Prof. Kim’s
comment, Jae-Weon Kim added that whether performing para-aortic lymph node dissection
or not should be counted in the analysis.
In the last lecture of the morning session, Jeong-Yeol Park talked about the KGOG
3033 study. The KGOG 3033 study is a prospective study evaluating a strategy of surgery
alone and surveillance in FIGO stage I malignant ovarian germ cell tumors. He said
that 75% of cases had been ‘cured’ by surgery alone. In the following discussion session,
it was suggested that, due to the rapidly progressive characteristics of yolk sac
tumors, a follow-up period of 3 months would be too long. Another opinion was that
3-year OS would be better than 2-year OS as the primary endpoint.
In the afternoon session, discussion about effective cooperation and authorship regarding
the SUNNY trial took place. Presentations about the data management systems of SGOG
and KGOG were followed. Given that over 70 participants including many young doctors
from KGOG and SGOG attended this joint meeting, the future of cooperation between
KGOG and SGOG is promising.
In the afternoon session, members of KGOG and SGOG actively discussed the SUNNY trial,
including cooperation and authorship bylaw. Overall, the discussions ran smoothly,
and it was decided that authorship would be supplemented and then decided on at a
future meeting. Then, Jae-Weon Kim elaborated on the history of KGOG-SGOG joint meeting
and suggested a concept for KGOG-SGOG cooperation. He called for a Korean co-principal
investigator, and recommended Suk-Joon Chang for this position.
During the last afternoon session, there were various presentations on data management
at SGOG and KGOG. The first was on data management and e-CRFs (clinical research forms)
by Zi-Yong Xiang, from SGOG, the second was about randomization in the SUNNY trial
by Wei Zhang from SGOG, and the last one on KGOG data management was by Kidong Kim.
They all spoke in detail and presented reasonable and secure approaches for data management.
During the Joint Meeting, every participant was interested in meeting topics and raised
a lot of questions, comments and discussions about the SUNNY trial. The Joint Meeting
was a good chance for mutual understanding as gynecologic oncologists for all the
participants, especially the young doctors.
Rongyu Zang hosted this meeting together with Asia-Pacific Ovarian Cancer Laparotomy
and Laparoscopic Operation (APOLLO) symposium in June 19, 2016, in which one Korean
moderator, Jae-Weon Kim preside a session and two Korean speakers, Byoung-Gie Kim
and Sang-Yoon Park (National Cancer Center, Korea) gave lectures on ‘novel molecular
targets for EOC’ and ‘upper abdominal surgery in advanced ovarian cancer,’ respectively.
WHICH IS BETTER: UPFRONT SURGERY OR NACT? DISPUTE KEEPS GOING ON, BUT THE SUNNY TRIAL
IS ON THE WAY - A REPORT OF 2016 APOLLO SYMPOSIUM IN SHANGHAI
Despite modest improvements in the outcome of ovarian cancer patients over the past
decades, EOC, especially high-grade serous type remains most commonly diagnosed with
advanced stages and associated with poor prognosis. PDS followed by platinum-based
chemotherapy is still the standard treatment for recent decade. In addition, the lack
of well-trained oncologic gynecologists for ovarian cancer surgery has repercussions
on patients’ outcome. Therefore, updated knowledge and surgery training generated
from translational researches and well-designed clinical trials are more needed.
Zhongshan Hospital, Fudan University initiated the 2016 Shanghai APOLLO symposium
(Fig. 3). APOLLO means exploration of novel and precise surgical treatment for ovarian
cancer, translational research of precision medicine. The annual APOLLO symposium
and China National Continuing Medical Education (CME) program for ovarian cancer surgery,
was successfully held at Huisheng Hall of Shanghai Zhongshan Hospital, Fudan University
from June 19th to 21st, 2016. To our knowledge, this is the first international symposium
focused on ovarian cancer surgery held in China. The APOLLO symposium and CME program
was hosted by Zhongshan Hospital, Fudan University and supported by SGOG. A total
of more than 120 gynecologic oncologists from United States, Korea, Hong Kong, and
China attended this meeting under the theme of ‘Ovarian Cancer Surgery’.
Fig. 3
2016 Asia-Pacific Ovarian Cancer Laparotomy and Laparoscopic Operation (APOLLO) Symposium
in Shanghai.
The purpose of this year’s symposium was to conduct a high level of discussion and
debate on ovarian cancer surgery, live surgery training for laparotomy, laparoscopic,
and robotic, multidisciplinary team (MDT) cooperation in the management of ovarian
cancer. The opening ceremony was chaired by Rongyu Zang. Across the meeting sessions,
a total of 30 presentations were given, which comprised of two opening speeches, six
radical surgery speeches, five translational medical research speeches, four laparoscopic
diagnosis and surgery speeches, five MDT cooperation speeches, four speeches on ovarian
cancer surgery and MDT perioperative management, as well as four academic seminar
presentations. Invited international speakers are Michael Bookman (USA), two from
KGOG: Byoung-Gie Kim and Sang-Yoon Park, one from Hong Kong, Hextan Ngan.
Specifically, in the radical surgery session, Rongyu Zang and Michael Bookman present
their comments and discussions for radical surgery of ovarian cancer from oncologic
gynecologists’ and from medical oncologists’ perspectives. Then Hextan Ngan gave her
lecture about the National Comprehensive Cancer Network (NCCN)/FIGO guideline of radical
surgery. Sang-Yoon Park presented the issues of upper abdominal surgery in advanced
ovarian cancer. The SUNNY trial, which has recently started its first site under the
cooperation of Chinese and Korean teams, will benefit from those topics and active
discussions. Although 40% patients with advanced EOC receive NACT today in the United
States, upfront radical surgery is still the primary choice in those centralized centers
for EOC care in the United States, Korea, and China as well. Despite such a confused
situation around the world remains, randomized clinical trials from professional surgical
teams will finally resolve the dispute, probably around 2025. In the translational
research session, Byoung-Gie Kim presented novel molecular targets for EOC. Then other
Chinese speakers gave lectures about molecular mechanisms and progresses on ovarian
cancer therapy. In the laparoscopic diagnosis and surgery session, Chinese oncologic
gynecologists presented improved technology of laparoscopic surgery in EOC. In MDT
session, medical oncologists, pathologists, radiologists and oncologic gynecologists
elucidated the systemic treatments of advanced EOC by their opinions. In the perioperative
management session, the speakers debated on the issues of retroperitoneal lymphadenectomy,
colorectectomy, urinary surgery, and perioperative complications.
Except for the intensive lectures with accompanying discussions during the academic
sections, the symposium had two live surgery and two tumor board sections. Live operations
of radical surgery for primary and recurrent disease were presented. One was diagnosed
with EOC stage IIIC and treated by PDS, diaphragmatic stripping and Dixon surgery.
The other was a second relapse case undergoing secondary cytoreductive surgery, partial
ileal resection and enteroenterostomy. In the tumor board section, two ovarian cancer
patients were discussed vigorously by ovarian cancer MDT committee. One was an initial
treatment case, and the other was a recurrent case.
Related collections
Author and article information
Comments
Comment on this article
scite_