- Record: found
- Abstract: found
- Article: found
Inhalation of honey reduces airway inflammation and histopathological changes in a rabbit model of ovalbumin-induced chronic asthma
Read this article at
Abstract
Background
Honey is widely used in folk medicine to treat cough, fever, and inflammation. In this study, the effect of aerosolised honey on airway tissues in a rabbit model of ovalbumin (OVA)-induced asthma was investigated. The ability of honey to act either as a rescuing agent in alleviating asthma-related symptoms or as a preventive agent to preclude the occurrence of asthma was also assessed.
Methods
Forty New Zealand white rabbits were sensitized twice with mixture of OVA and aluminium hydroxide on days 1 and 14. Honey treatments were given from day 23 to day 25 at two different doses (25% (v/v) and 50% (v/v) of honey diluted in sterile phosphate buffer saline. In the aerosolised honey as a rescue agent group, animals were euthanized on day 28; for the preventive group, animals were further exposed to aerosolised OVA for 3 days starting from day 28 and euthanized on day 31. The effects of honey on inflammatory cell response, airway inflammation, and goblet cell hyperplasia were assessed for each animal.
Results
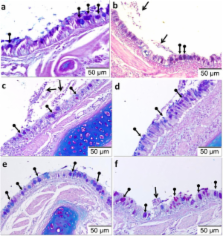
Histopathological analyses revealed that aerosolised honey resulted in structural changes of the epithelium, mucosa, and submucosal regions of the airway that caused by the induction with OVA. Treatment with aerosolised honey has reduced the number of airway inflammatory cells present in bronchoalveolar lavage fluid and inhibited the goblet cell hyperplasia.
Conclusion
In this study, aerosolised honey was used to effectively treat and manage asthma in rabbits, and it could prove to be a promising treatment for asthma in humans. Future studies with a larger sample size and studies at the gene expression level are needed to better understand the mechanisms by which aerosolised honey reduces asthma symptoms.
Related collections
Most cited references17
- Record: found
- Abstract: found
- Article: not found
Pulmonary expression of interleukin-13 causes inflammation, mucus hypersecretion, subepithelial fibrosis, physiologic abnormalities, and eotaxin production.
- Record: found
- Abstract: found
- Article: not found